| Contents |
|---|
 NoPINOs NoPINOs | July, 2024 |
 Single payer! Single payer! | June, 2024 |
 DocGPT DocGPT | Apr., 2024 |
 Gut bugs Gut bugs | Mar., 2024 |
 Fix ER waits Fix ER waits | Feb., 2024 |
 Winning strategy Winning strategy | Jan., 2024 |
 Nursing ed v.2 Nursing ed v.2 | Jan., 2024 |
 The Benjamins The Benjamins | Oct., 2023 |
 Sex in the SNF Sex in the SNF | Sep., 2023 |
 Perel wisdom Perel wisdom | Aug., 2023 |
 Politics and death Politics and death | July, 2023 |
 Colonoscopy sense Colonoscopy sense | June, 2023 |
 Prolon fast Prolon fast | May, 2023 |
 Nursing Education 2.0 Nursing Education 2.0 | Feb., 2023 |
 Kleptocapitalism Kleptocapitalism | Jan., 2023 |
 Covid ICU Covid ICU | Jan., 2023 |
 Under attack Under attack | Dec., 2022 |
 Guns! Regulate! Guns! Regulate! | Dec., 2022 |
 Time management Time management | Nov., 2022 |
 Medical disinformation Medical disinformation | Oct., 2022 |
 Nurses? Models? Nurses? Models? | Sep., 2022 |
 CPR: Wrong Default CPR: Wrong Default | Aug., 2022 |
 Rethinking nursing informatics Rethinking nursing informatics | Aug., 2022 |
 Advance care Advance care | July, 2022 |
 RaDonda redux RaDonda redux | May, 2022 |
 Overhaul SNFs Overhaul SNFs | May, 2022 |
 Wilderness Wilderness | May, 2022 |
 Criminal error? Criminal error? | Apr., 2022 |
 Data in the rigs Data in the rigs | Apr., 2022 |
 Gov't wants SNF quality Gov't wants SNF quality | Apr., 2022 |
 I got rhythm I got rhythm | Feb., 2022 |
 Hospital at home? Hospital at home? | Dec., 2021 |
 We SAFER? We SAFER? | Dec., 2021 |
 Falls Falls | Dec., 2021 |
 A giant has passed A giant has passed | Nov., 2021 |
 Ageism is a thing Ageism is a thing | Oct., 2021 |
 Covid future Covid future | Oct., 2021 |
 We have Covid We have Covid | Sep., 2021 |
 NY Tristate NY Tristate | Sep., 2021 |
 Dottoressa Dottoressa | Sep., 2021 |
 ANIA 2021 ANIA 2021 | Aug., 2021 |
 Hesitancy schmesitancy Hesitancy schmesitancy | July, 2021 |
 Go Nursing Informatics! Go Nursing Informatics! | June, 2021 |
 LACEd Up! LACEd Up! | Apr., 2021 |
 Covid Staffing? Covid Staffing? | Mar., 2021 |
 New blog New blog | Mar., 2021 |
 Vaxes 'r us! Vaxes 'r us! | Jan., 2021 |
 Biden? Nurses! Biden? Nurses! | Nov., 2020 |
 Fix pandemic Fix pandemic | Nov., 2020 |
 Wear that mask! Wear that mask! | Nov., 2020 |
 Herd immunity? Herd immunity? | Nov., 2020 |
 Incompetents in charge Incompetents in charge | Nov., 2020 |
 Medicare and Youpays Medicare and Youpays | Oct., 2020 |
 Burdensome EHRs Burdensome EHRs | Sept., 2020 |
 Innovate! Perform! Innovate! Perform! | Sept., 2020 |
 Droplet? Airborne? Droplet? Airborne? | July, 2020 |
 Madison Covid Screening Madison Covid Screening | July, 2020 |
 Goodbye Zakheim Goodbye Zakheim | June, 2020 |
 Clinicians and computers Clinicians and computers | June, 2020 |
 RN = IT RN = IT | June, 2020 |
 What SNFs must do What SNFs must do | May, 2020 |
 Eating my own dogfood Eating my own dogfood | May, 2020 |
 In defense of SNFs In defense of SNFs | May, 2020 |
 Big babies Big babies | May, 2020 |
 Covid Times Covid Times | Apr., 2020 |
 NEJM on SNFs NEJM on SNFs | Apr., 2020 |
 SNF musings SNF musings | Apr., 2020 |
 Sitting ducks Sitting ducks | Apr., 2020 |
 Nursing plans dead Nursing plans dead | Apr., 2020 |
 Informatics for pandemics Informatics for pandemics | Mar., 2020 |
 Coronawisdom Coronawisdom | Mar., 2020 |
 Wrongheaded graph Wrongheaded graph | Mar., 2020 |
 Corona no conference Corona no conference | Mar., 2020 |
 Cruel bills Cruel bills | Feb., 2020 |
 Year of the nurse Year of the nurse | Jan., 2020 |
 Shopping around Shopping around | Jan., 2020 |
 Ber-nie! Ber-nie! | Jan., 2020 |
 Checklist is ten Checklist is ten | Jan., 2020 |
 Portals suck Portals suck | Dec., 2019 |
 Nurses assess Nurses assess | Dec., 2019 |
 Another behemoth fails? Another behemoth fails? | Dec., 2019 |
 Rethinking nutrition Rethinking nutrition | Dec., 2019 |
 RN, heal thineself RN, heal thineself | Dec., 2019 |
 Still volunteering Still volunteering | Oct., 2019 |
 Vegan works Vegan works | Sep., 2019 |
 Patient engagement Patient engagement | Sep., 2019 |
 Linked In Linked In | Sep., 2019 |
 Afib Afib | July, 2019 |
 Goodbye Kaiser Goodbye Kaiser | June, 2019 |
 HIMSS hype HIMSS hype | June 2019 |
 Not interested Not interested | June 2019 |
 Numbers Numbers | June 2019 |
 Break fast Break fast | May 2019 |
 It works! It works! | May 2019 |
 Get well Get well | May 2019 |
 Allopaths 'r us Allopaths 'r us | May 2019 |
 Going fast Going fast | May 2019 |
 Free radical Free radical | May 2019 |
 Nurse informaticians 'r us! Nurse informaticians 'r us! | Apr. 2019 |
 EHR report card EHR report card | Mar. 2019 |
 Paying for m4a Paying for m4a | Mar. 2019 |
 Bad behavior points Bad behavior points | Feb 2019 |
 No vax? Die! No vax? Die! | Feb. 2019 |
 Still turkeys Still turkeys | Dec. 2018 |
 Nursing orders Nursing orders | June 2018 |
 Sugar = poison Sugar = poison | Aug. 2018 |
 Another nurse hero Another nurse hero | June 2018 |
 EHR market shares EHR market shares | June 2018 |
 Reboot education Reboot education | June 2018 |
 Gun research Gun research | Apr. 2018 |
 Epic Mecca Epic Mecca | Dec. 2017 |
 Not documented not done Not documented not done | Jan. 2018 |
 Econ 101 Econ 101 | Jan. 2018 |
 Nursing the system Nursing the system | Nov. 2017 |
 Choke it down Choke it down | June 2017 |
 Kaiser Ed Kaiser Ed | May 2017 |
 Never events Never events | Apr. 2017 |
 Reconciling Reconciling | Apr. 2017 |
 High reliability High reliability | Apr. 2017 |
 Comms metaphor Comms metaphor | Apr. 2017 |
 Pleading the fifth Pleading the fifth | Feb. 2017 |
 Synapse firing Synapse firing | Oct. 2014 |
 Gold standard Gold standard | Jan. 2017 |
 Data for sale Data for sale | Jan. 2017 |
 Quandary solved Quandary solved | Jan. 2017 |
 Nurse, Advocate Nurse, Advocate | Jan. 2017 |
 Escaping the spotlight Escaping the spotlight | Dec. 2016 |
 TrumpCare? TrumpCare? | Dec. 2016 |
 Nursonomics Nursonomics | Nov. 2016 |
 Trumbers Trumbers | Oct. 2016 |
 Learn informatics! Learn informatics! | Aug. 2016 |
 Balancing act Balancing act | Aug. 2016 |
 It's the workflow, stupid It's the workflow, stupid | Aug. 2016 |
 RN + Rx? RN + Rx? | July 2016 |
 More war stories More war stories | June 2016 |
 Nurses are underserved Nurses are underserved | June 2016 |
 War story War story | June 2016 |
 Bundling & engagement Bundling & engagement | Apr. 2016 |
 PHC 62 PHC 62 | Mar. 2016 |
 Little guys Little guys | Mar. 2016 |
 Financial incentives Financial incentives | Mar. 2016 |
 Big data Big data | Mar. 2016 |
 Vaccinations, revisited Vaccinations, revisited | Mar. 2016 |
 Healthcare Econ 101 Healthcare Econ 101 | Feb. 2016 |
 Obstacle? Opportunity! Obstacle? Opportunity! | Feb. 2016 |
 Get real Get real | Feb. 2016 |
 Cool gig Cool gig | Jan. 2016 |
 Work to do Work to do | Nov. 2015 |
 General Zuckerberg General Zuckerberg | Nov. 2015 |
 Coding Nursing Coding Nursing | Nov. 2015 |
 AMIA 2015 AMIA 2015 | Nov. 2015 |
 Innovate! Innovate! | Nov. 2015 |
 Boot camp Boot camp | Sep. 2015 |
 Yes vault Yes vault | Sep. 2015 |
 No vault No vault | Sep. 2015 |
 Good vault? Good vault? | Aug. 2015 |
 How sick? How sick? | Aug. 2015 |
 Nurses more than ever Nurses more than ever | Aug. 2015 |
 Numbers Numbers | Aug. 2015 |
 Yes, patients Yes, patients | Aug. 2015 |
 Go Bernie! Go nurses! Go Bernie! Go nurses! | Aug. 2015 |
 ACA for whom? ACA for whom? | Aug. 2015 |
 Cool clear Brooke Cool clear Brooke | July 2015 |
 Interopera-wha? Interopera-wha? | June 2015 |
 Defending their turf Defending their turf | June 2015 |
 Dentist regent Dentist regent | May 2015 |
 Woulda shoulda Woulda shoulda | May 2015 |
 Nursing volunteer Nursing volunteer | May 2015 |
 Military RNs Military RNs | May 2015 |
 Overkill Overkill | May 2015 |
 BANIA BANIA | Apr. 2015 |
 World domination World domination | Apr. 2015 |
 HIMSS and HERSS HIMSS and HERSS | Apr. 2015 |
 HIMSS15 HIMSS15 | Apr. 2015 |
 Patient-centric? Patient-centric? | Apr. 2015 |
 We've come a long way... We've come a long way... | Apr. 2015 |
 Pepsi apples Pepsi apples | Apr. 2015 |
 Counting Counting | Jan. 2015 |
 New Guy New Guy | Jan. 2015 |
 PHC 57 PHC 57 | Dec. 2014 |
 Supes vs soda Supes vs soda | Dec. 2014 |
 23 and Anne 23 and Anne | Dec. 2014 |
 Pride and precision Pride and precision | Dec. 2014 |
 Play with FHIR Play with FHIR | Nov. 2014 |
 AMIA! AMIA! | Nov. 2014 |
 Et tu, RNs? Et tu, RNs? | Nov. 2014 |
 Wise Cutting Wise Cutting | Oct. 2014 |
 Talking Sense Talking Sense | Oct. 2014 |
 Lava Mae Lava Mae | Oct. 2014 |
 Hey Obama Hey Obama | Oct. 2014 |
 Schmebola Schmebola | Oct. 2014 |
 New Vectors New Vectors | Sep. 2014 |
 Teachers Teachers | Sep. 2014 |
 Ebola Gates Ebola Gates | Sep. 2014 |
 Ebola death Ebola death | Sep. 2014 |
 Corporate genetics Corporate genetics | Aug. 2014 |
 A nurse hero A nurse hero | Aug. 2014 |
 Talking soda tax Talking soda tax | Aug. 2014 |
 Ebola hysteria Ebola hysteria | Aug. 2014 |
 A garden to tend A garden to tend | Aug. 2014 |
 Medicare for all Medicare for all | July 2014 |
 Back in the saddle Back in the saddle | July 2014 |
 Astro Truth Astro Truth | July 2014 |
 Health Health | July 2014 |
 MU phase 2 MU phase 2 | July 2014 |
 Save VistA Save VistA | July 2014 |
 Apple Health Apple Health | July 2014 |
 Vocabulary 101 Vocabulary 101 | June 2014 |
 End employer-provided End employer-provided | May 2014 |
 ACA in real life ACA in real life | Apr. 2014 |
 Go SF Go SF | Apr. 2014 |
 New Model New Model | Mar. 2014 |
 Too HIPAA Too HIPAA | Mar. 2014 |
 Big soda spending Big soda spending | Mar. 2014 |
 Who was first? Who was first? | Mar. 2014 |
 How we die How we die | Mar. 2014 |
 Big soda Big soda | Feb. 2014 |
 Politics or health? Politics or health? | Jan. 2014 |
 Disaster not Disaster not | Jan. 2014 |
 Wing nuts Wing nuts | Dec. 2013 |
 Heroic senator Heroic senator | Dec. 2013 |
 More homeless More homeless | Dec. 2013 |
 Nurses next Nurses next | Dec. 2013 |
 Empire emerging Empire emerging | Dec. 2013 |
 Obamacare and me Obamacare and me | Oct. 2013 |
 Future now Future now | Sep. 2013 |
 Get Social Get Social | Sep. 2013 |
 Bedside blogger Bedside blogger | Aug. 2013 |
 Homeless connect Homeless connect | Aug. 2013 |
 Mere apps Mere apps | Aug. 2013 |
 Roadmap to Single-Payer Roadmap to Single-Payer | July 2013 |
 Nursing Iceberg Nursing Iceberg | July 2013 |
 Gimme Data Gimme Data | June 2013 |
 Simple Dollar Simple Dollar | May 2013 |
 Data ownership, redux Data ownership, redux | Apr. 2013 |
 Doc-by-mail? Doc-by-mail? | Mar. 2013 |
 Biggest carriers Biggest carriers | Jan. 2013 |
 Not a moment too soon Not a moment too soon | Dec. 2012 |
 Partisans Partisans | Dec. 2012 |
 Against the tide Against the tide | Dec. 2012 |
 Scan this! Scan this! | Dec. 2012 |
 Being Present Being Present | Sept. 2012 |
 UCSF's APeX Go-Live UCSF's APeX Go-Live | June 2012 |
 Silent organs Silent organs | Jan. 2012 |
 Lateral violence Lateral violence | Dec. 2011 |
 Healthcare & advertising Healthcare & advertising | Nov. 2011 |
 UC is in trouble UC is in trouble | Sep. 2011 |
 Greedy nurses? Greedy nurses? | Sep. 2011 |
 Hear us roar! Hear us roar! | Sept. 2011 |
 Strikes, yikes! Strikes, yikes! | Sept. 2011 |
 Trimming the fat Trimming the fat | Sept. 2011 |
 New fraud New fraud | Sept. 2011 |
 National Health IT Week National Health IT Week | Sept. 2011 |
 MDs & RNs are not enough MDs & RNs are not enough | July 2011 |
 A good guy at the top A good guy at the top | July 2011 |
 You'll be safe here You'll be safe here | July 2011 |
 Google Health dead Google Health dead | June 2011 |
 Cancer cures? Cancer cures? | May 2011 |
 Woo Hoo! We're Winning! Woo Hoo! We're Winning! | May 2011 |
 Profits for Insurers Profits for Insurers | May 2011 |
 Foreshadow things to come? Foreshadow things to come? | May 2011 |
 Profit? Profit? | May 1, 2011 |
 Calif. Healthcare Act Calif. Healthcare Act | Apr. 2011 |
 Beware the 3 Ds Beware the 3 Ds | Apr. 2011 |
 Quantity or Quality? Quantity or Quality? | Apr. 2011 |
 Words! Words! | Mar. 2011 |
 Start Something Start Something | Feb. 2011 |
 Government = Inefficient? Government = Inefficient? | Feb. 2011 |
 Mind = Brain? Mind = Brain? | Feb. 2011 |
 Capped! Capped! | Feb. 2011 |
 Planning for prevention Planning for prevention | Feb. 2011 |
 Penny-wise... Penny-wise... | Jan. 2011 |
 Pinned! Pinned! | Dec. 2010 |
 Men at work Men at work | Dec. 2010 |
 Dear diary Dear diary | Dec. 2010 |
 Brainy nurses Brainy nurses | Dec. 2010 |
 Emergency! Emergency! | Dec. 2010 |
 Public option, public sector Public option, public sector | Nov. 2010 |
 Change the world Change the world | Oct. 2010 |
 Want a hero? Or a checklist? Want a hero? Or a checklist? | Oct. 2010 |
 Environursing Environursing | Oct. 2010 |
 Don't call it compliance Don't call it compliance | Sep. 2010 |
 Shoppin' spree? Shoppin' spree? | Aug. 2010 |
 Double mandate? Double mandate? | Aug. 2010 |
 Control your medical data? Control your medical data? | May 2010 |
 Conform & stethoscopes Conform & stethoscopes | May 2010 |
 Do nurses compute? Do nurses compute? | Apr. 2010 |
 Addiction phobia Addiction phobia | Apr. 2010 |
 Krugman nails it again Krugman nails it again | Mar. 2010 |
 Recognizing diabetes Recognizing diabetes | Mar. 2010 |
 A new stethoscope... A new stethoscope... | Mar. 2010 |
 Blame the Lawyers Blame the Lawyers | Feb. 2010 |
 Turkeys vote for Xmas Turkeys vote for Xmas | Jan. 2010 |
 The Incentive that Works The Incentive that Works | Dec. 2009 |
 Doctors? Businessmen? Doctors? Businessmen? | Nov. 2009 |
 Gullibles Gullibles | Sep. 2009 |
 Speier Gets It! Speier Gets It! | Sep. 2009 |
 Snowe Job Snowe Job | June 2009 |
 Chronic Disease Systems Chronic Disease Systems | May 2009 |
 Vaccinate! Vaccinate! | Jan. 2009 |
 Health Sites Health Sites | Jan. 2009 |
 Obama Gets It! Obama Gets It! | Jan. 2009 |
 Unfair Advantages? Unfair Advantages? | Jan. 2009 |
 USHealthCrisis: Francine? USHealthCrisis: Francine? | Jan. 2009 |
 Google knows you... Google knows you... | Nov. 2008 |
 Heart Attack Grill Heart Attack Grill | Nov. 2008 |
 How Do Italians Pay for It? How Do Italians Pay for It? | Oct. 2008 |
 Yes on Calif Bill 840! Yes on Calif Bill 840! | Sep. 2008 |
 Pat Rants Pat Rants | Aug. 2008 |
 Medical-Industrial Medical-Industrial | July 2008 |
 Nosocomial Infections Nosocomial Infections | June 2008 |
 Gore Gets It! Gore Gets It! | May 2008 |
 Kucinich Gets It! Kucinich Gets It! | Apr. 2008 |
 Neurosurgery in Vietnam Neurosurgery in Vietnam | Mar. 2008 |
 Americans Pay for It? Americans Pay for It? | Mar. 2008 |
 Google Gets It Google Gets It | Mar. 2008 |
 Surprised! ...Again Surprised! ...Again | Feb. 2008 |
 EMR: Still Waiting EMR: Still Waiting | Jan. 2008 |
 Medical System Ashamed! Medical System Ashamed! | Dec. 2007 |
 Gavin Gets It! Gavin Gets It! | Sep. 2007 |
 Cato Schmato Cato Schmato | Sep. 2007 |
 Do You Read Me? Do You Read Me? | Aug. 2007 |
 Clear about Single Payer Clear about Single Payer | May 2007 |
 "Socialized medicine" "Socialized medicine" | Feb. 2007 |
 Post-Oil World Post-Oil World | Jan. 2007 |
 Getting It Explained? Getting It Explained? | July 2006 |
 Pritikin's Still Got It! Pritikin's Still Got It! | June 2006 |
 No Butts No Butts | May 2006 |
 Nurses On the Job? Nurses On the Job? | Apr. 2006 |
 Beat It Beat It | Mar. 2006 |
 Homework-O-Matic Homework-O-Matic | Feb. 2006 |
 That Is Sick! That Is Sick! | Jan. 2006 |
 Go Aussies! Go Aussies! | Dec. 2005 |
 Shifting paradigms Shifting paradigms | Nov. 2005 |
 My Own Medical Data? My Own Medical Data? | Oct. 2005 |
 Higher Ed: Revolution Higher Ed: Revolution | Sep. 2005 |
 Doesn't Compute Doesn't Compute | Aug. 2005 |
 Emotion Emotion | July 2005 |
 Don't Just Protect Me Don't Just Protect Me | June 2005 |
 The Art of Volunteering The Art of Volunteering | May 2005 |
 About Dan About Dan | |
|
| |

NoPINOs
again
July 22, 2024 --
NoPINOs -- a term I coined here -- have become a common financial structure in US healthcare, and stray ever further from their original purpose. What's a NoPINO? It's a non-profit in name only. In Why many nonprofit (wink, wink) hospitals are rolling in money, Elizabeth Rosenthal writes in the Washington Post:
When many U.S. hospitals were founded over the past two centuries, mostly by religious groups, they were accorded nonprofit status for doling out free care during an era in which fewer people had insurance and bills were modest. The institutions operated on razor-thin margins. But as more Americans gained insurance and medical treatments became more effective � and more expensive � there was money to be made.
And make it they do. Without being taxed. The notion of "community benefit" is ill-defined by the IRS and the hospital executives' pay packages are bloated, running into the millions.
...they are not channeling Mother Teresa. Maybe it�s time to end the community benefit charade for those that exploit it, and have these big businesses pay at least some tax? Communities could then use those dollars in ways that directly benefit residents� health.
top
|
| |
 Single
Single
Payer
Now!
June 19, 2024 --
Dear SFC Editor,
I write to commend the comments in Linda Baumann's letter in today's SFC. As she points out, single-payer health is long past due. This deserves a little elucidation: why single-payer?
When there is more than one payer -- and often the payer winds up being the patient -- the incentive is to stick the other guy with the bill. Thus, unconscionable mountains of paperwork confront our hapless healthcare providers and vast insurance company and State and Federal bureaucracies are erected.
Numerous studies demonstrate that 15% to 30% of our healthcare dollars are thus consumed. Compare this to any country (such as, say, Canada) that does actually have a single payer. There, the bureaucratic overhead is typically 4% to 8%. And no medical bankruptcies.
Come on, California! We are compassionate people. We lead the nation in so many ways... Let's do this!
Go California!
-- Dan Keller RN MS
top
|
| |

DocGPT
April 12, 2024 --
We knew it was coming. Now it's here. Computers diagnose better than humans.
In Are You Ready for AI to Be a Better Doctor Than You? published today in Medscape Medical News, Joe Kita writes of artificial intelligence applied to medicine.
ChatGPT made the correct diagnosis in 97% of patients compared to 87% for human doctors.
Missed diagnoses are a big problem in healthcare today so this is good news for patients, right?
Often, the doctors are not pleased. Sometimes with good reason. For example, clinical labs are an area of effective AI enhancement. One doc observed, "...he's had several instances where patients received their cancer diagnosis from the lab through an automated patient-portal system rather than from him." Surely patients would prefer to hear this from humans.
My own opinion? On balance, AI in healthcare is a good thing. MDs will grow accustomed to using AI for its strengths (esp. diagnoses). But let's not fall for the hype cycle. AI is having a media frenzy right now. Eventually, AI-based tools in healthcare will settle into place -- they won't replace doctors (or nurses!) -- and quality of care will rise.
Go tech-savvy clinicians!
top
|
| |

Gut
bugs
March, 2024 --
I have blogged about how the kidneys run the show. But I've changed my mind. Now I think it's the gut. And its all-important microbiome:
Over the last 20 years, research has linked problems in the gut microbiome to a wide variety of conditions, including inflammatory bowel disease, autoimmune diseases like rheumatoid arthritis, metabolic ones like diabetes, and cardiovascular disease, asthma, and even autism. [Medscape]
What's a microbiome? Wikipedia calls it a "community of microorganisms that can usually be found living together in any given habitat." In this case, the habitat is your gut. There are, technically speaking, zillions of bacteria living in there, each demanding its own type of nutrients and thriving or starving depending on what you eat. They then poop out body-regulating chemicals. So you want to feed the good ones.
Wikipedia goes on, "The mammalian gut microbiome has emerged as a key regulator of host physiology." In other words, eating bad stuff grows bad bugs that poop out chemicals that regulate your body toward disease states, especially chronic conditions: "...dysregulation of the gut flora has been correlated with a host of inflammatory and autoimmune conditions."
So it's not quite accurate to say that the gut regulates our bodies; it's the bugs that live in it that do this. Eat right -- mainly plant-based foods and lots of fiber -- and you'll feed the beneficial bugs and stay healthy.
Go nutrition-savvy clinicians! Go forces for change in the American diet!
top
|
| |

Fix
ER
waits
February, 2024 --
Hurry up and wait!
The benjamins, the benjamins... yet again.
The incentives in American healthcare continue to be wrong. It's bad for us!
When's the last time you went to an ER? No doubt you wondered why you were kept waiting for so many hours.
Why is this system so badly broken?
Dr. Morhaim explains it well: How to fix Maryland's ER wait times: Cut executive salaries. A lot.
He also explains what
happens when for-profits take over hospitals... It's not pretty.
Viewed through a financial lens, the purpose of an ER in a hospital is to be the primary admissions portal.
Typically, at least half of a hospital's patients arrive that way.
When the admitting process gets backed up, patients are backlogged in the ER.
Why the process slowdown? Cost cutting. Corporate bean counters.
They are doing their job... but it's a job that shouldn't exist, or at least today's incentives shouldn't.
Quality of care and outcomes should be the drivers, not corporate
(including NOPINOs!) profits.
Single-payer is a big part of the solution.
But given the present incentive structure (and the political might that perpetuates it)
don't expect change anytime soon...
Instead, hurry up and wait!
Dr. Morhaim's message?
Don�t let anyone tell you that we don�t have the money to do better. We do. The money is there. It�s just not going to where it�s needed: to those who perform the front-line work of patient care and for preventive services and public health.
Go Dr. Morhaim! Go front-line nurses! Go forces for change!
-- cartoon by my Dad, Charles Keller
top
|
| |

A winning
strategy
at last
January, 2024 --
How do you sell a nursing app? How do you sell two of them?
Yes, I have developed two -- NurseAssess and NurseMind -- each more brilliant than the last. Workflow-centric... reality-based... developed by nurses for nurses... making nursing better... or should. Alas, the marketplace hasn't cooperated.
In my first approach, I expected nurses far and wide to use and love my apps and subscribe for just four bucks a month. Alas, this approach was a flop; on the Internet, everything is free. Even just four bucks scared people off.
My second approach I termed "come from below". I expected nurses everywhere to enthusiastically adopt my apps and use them on the job. This would get management's attention and lead to sales. Though many nurses did indeed use the apps, they needed to be surreptitious; they weren't officially sanctioned. Often, cellphone use at work (BYOD) is unauthorized. So successes were covert, the opposite of what I'd hoped.
Approach #3: talk to hospital management. Demonstrate improved nursing workflow, increased efficiency, enhanced job satisfaction and data reporting accuracy. They'll surely license the product and direct IT to connect it to the EHR. This, too, flopped. Managers are largely fear-driven. Looking at a product to buy or a workplace strategy to employ, a manager seeks reduced cost or increased revenue. Something more subtle -- improved workflow, job satisfaction, or data quality -- is rarely worth sticking out your neck.
 Yet we know we have a valuable improvement for nurses. How do we get it into their hands?
Yet we know we have a valuable improvement for nurses. How do we get it into their hands?
Approach number four is surely the answer: the EHR vendors will welcome this mobile solution as a value-add for their product. Sure, they already have mobile solutions. E.g. Epic has Rover and Haiku. Other EHR vendors, too, offer mobile extensions. But none is nursing workflow-centric. Nurses rarely use them. These vendors' products will benefit mightily from NurseAssess and NurseMind.
Go tech-savvy nurses! Go enlightened management! Go brilliant EHR vendors!
top
|
| |

Nursing
ed
v.2
January, 2024 --
In some ways, classroom-based education is like airplane travel. Each seat has a price, and if it's empty at takeoff it goes unfilled. For the school, filling those seats is essential for financial survival. For the student, occupying those seats is essential for acquiring professional expertise and a degree. What's the best way to match them up? A new business model could make these matches better.
Selling education according to an air travel model would solve some of the problems of the existing educational system. One such problem is the lack of incentives for quality. There is little motivation to make the educational experience a good one, since -- once they matriculate -- the buyer (the student) is locked in.
Imagine instead that the student has a shopping list of courses that must be taken, determined by the certifying State Board, e.g.
California's Board of Registered Nursing (BRN) that decides what topics must be mastered in order to receive the degree (Associate, BSN, MSN) and how many units (classroom hours) of each.
 Attendance at a given course is sold by a clearinghouse (like a travel agent selling tickets on many airlines). The student chooses by price, quality, reputation, schedule, and location. The schools become incentivized to deliver a quality product at a competitive price. Reviews and ratings become important. Teachers become driven to do a good job. The student has a new-found flexibility and consumer power in the marketplace. And nursing education at last must be good.
Attendance at a given course is sold by a clearinghouse (like a travel agent selling tickets on many airlines). The student chooses by price, quality, reputation, schedule, and location. The schools become incentivized to deliver a quality product at a competitive price. Reviews and ratings become important. Teachers become driven to do a good job. The student has a new-found flexibility and consumer power in the marketplace. And nursing education at last must be good.
Go radical educators! Go innovative students! Go fearless nurses!
top
|
| |

The
Benjamins
October 15, 2023 --
The things that primary care providers (PCPs) can do to get the best outcomes for patients
with chronic conditions are disincentivized by our medical-industrial complex. Why?
In the deathless words of Rep. Ilhan Omar, "It's all about the Benjamins, baby."
What could PCPs do to improve outcomes? Promote lifestyle change, educate about
healthful diet and fasting, and encourage and support
regular exercise.
Why don't they? These things don't make money so the system disincentivizes them.
In How
PCPs Are Penalized for Positive Outcomes From Lifestyle Change, Medscape reports that
they are rewarded not when the patient gets better but when the patient adheres to their medication regimen.
Yet often the medication is not the best therapy.
"In fact, some quality measures unintentionally penalize physicians for successfully treating
or reversing disease through lifestyle behavior interventions while rewarding clinicians
for meeting process measures � usually adherence to medication � regardless of whether
health outcomes improved."
Is this yet another ugly conspiracy? If so, the docs are not in on it.
Indeed, according to Medscape, they are among the victims, discouraged from doing what they know to be best.
How do we fix it? Implied by the Medscape article, one obvious solution is to tie
MD ratings to outcomes (did patients get better?) not just to process (did they do as they were told?)
But the more effective solution -- surely harder to implement -- is better regulation
of Big Pharma and the health insurance industry.
It's still about the Benjamins.
Go regulators! Go courageous PCPs! Go positive lifestyle-encouraging nurses!
top
|
| |

Sex
in the
SNF
September 21, 2023 --
Old people have sex? Who knew?
By a Medscape article, Love and Sex in the Nursing Home? Ethicist Says, 'Why Not?'
published today, we are shocked. Or maybe not.
 My mother, Judith Keller -- also an RN -- made a movie --
Rose by Any Other Name
on this very topic 35 years ago. It...
My mother, Judith Keller -- also an RN -- made a movie --
Rose by Any Other Name
on this very topic 35 years ago. It...
"Challenges stereotypes most of us don't even know we have."
--Indiana University Center on Aging
My mother...
Explores the reactions of other people to a loving relationship between
an aging pair and the pressures that are brought to end its "unseemliness".
Says the Ethicist...
Stopping nonconsensual activities, yes. [But] when mom chooses to have a
little romance in the nursing home, my attitude is to butt out.
This has been obvious to us for 35 years...
It's good to see the world catching up.
Go Ethicist! Go Mom (his and mine)! Go compassionate nurses!
top
|
| |

The
wisdom of
Esther Perel
August, 2023 --
Perel writes beautifully and her mastery of language and metaphor is delightful.
But she attains her full stride in person in her podcast, counseling a struggling couple,
conducting a therapeutic session, actively listening, reflecting, challenging with supreme skill.
Her 2017 book The State of Affairs: Rethinking Infidelity
captures the lessons she teaches in that context which, by its rawness --
neither rehearsed nor edited (as a book can be but a live session cannot) --
show the depth of her insight.
She perceives the subtlest cues and drives straight to the heart of her client's quandary.
Her performances are nothing short of spectacular.
My essay about this and her is here.
Go Esther! Go wise nurses!
top
|
| |

Politics
and
death
July 24, 2023 --
Politics is noisy but is it life and death? Evidently so.
This recent study in JAMA, Excess Death Rates for Republican and Democratic Registered Voters in Florida and Ohio During the COVID-19 Pandemic found:
"... In this cohort study evaluating 538�159 deaths in individuals aged 25 years and older in Florida and Ohio between March 2020 and December 2021, excess mortality was significantly higher for Republican voters than Democratic voters... the excess death rate for Republican voters was... 15%, higher than the excess death rate for Democratic voters..."
There are smart people in both parties. But are some willing to die for their ideologies?
Go political nurses!
top
|
| |

Colonoscopy
sense
June, 2023 --
Being 68 years old, I have undergone several routine colonoscopies (even a virtual colonoscopy once), as have my peers. Everyone has an opinion about the procedure, and so do I. Trouble is, most are excessively medicalized. This procedure intersects with two of our culture's strongest fetishes, which I'll describe. But first, here is the right way to prep for and then undergo this procedure.
How to prep: Driven by our culture's food fetish, you think you can't go without it for more than a few hours. Yet the doctor needs an empty bowel to examine so your task is to make it so. Standard prep recommendations call for laxatives and suppositories and diarrhea.
There's an easier way: just stop eating for three days prior. "But I can't do that!" you say. Of course you can; we homo sapiens evolved to handle long periods without sustenance. Think cavemen in wintertime. It's easier than people believe. After three days of fasting (clear liquids are OK as long as they're not red), your bowel will be nicely empty and you won't have poisoned yourself with those noxious chemicals.

How to undergo the procedure: Driven by our culture's phobia about things anal, many squeamish folk demand anesthesia. But that's not necessary; pain, if any, is mild; perhaps some brief stomach cramping, nothing you can't easily sustain. Not taking drugs is always better.
You want to be awake and alert so you can watch the video screen. No one is more interested in your insides than you. It's a rare opportunity for a guided tour. Your doctor can explain what he/she sees and does -- perhaps snip a polyp (which you don't feel because polyps have no enervation.)
Don't let the phobias drive you. Colonoscopy's just not a big deal. You can handle it!
Go enlightened patients! Go supportive providers!
top
|
| |

Prolon
fast
May 5, 2023 --
I've done it again. Not at Truenorth this time but at home. Not for three weeks but for five days. Not water-only but with a scientific "fasting nutrition program designed to nourish your body & mind while providing fasting benefits" (quoted from the box the food comes in).
 The method? A package named Prolon, designed by nutrition guru Valter Longo (see
www.dan-keller.com/nursing/vegan
), revered in the nutrition/fasting world. I've just finished day five of five and I feel great!
The method? A package named Prolon, designed by nutrition guru Valter Longo (see
www.dan-keller.com/nursing/vegan
), revered in the nutrition/fasting world. I've just finished day five of five and I feel great!
Prolon: "5-day fasting with food." The Prolon box (5-day fasting kit: $190) is beautiful, elaborate packaging with some powdered soups, fancy crackers, vitamin pills, nut bars, a few olives, and a liquid they call L-drink (I presume the L is for Longo). You measure and consume the L-drink according to your body weight.
Fasting means intake of zero calories. Prolon is not that. There is doubtless some real science behind these components but I'm convinced that the real value of the Prolon fast is simply calorie reduction, even if it's not quite to zero.
Prolon is 1150 calories on Day 1 and 750 calories on Days 2-5. This is a third or a fourth of typical daily intake,
enough to stave off hunger yet reach a mild ketosis and fasting metabolic state.
 The fast was facilitated by my friend Darcie Ellyne, nutritionist formerly at Mills Hospital (where I used to work).
She ran pre-, mid-, and post-fast Zoom sessions for the five of us participants. We did check-ins and chair yoga.
All helpful!
The fast was facilitated by my friend Darcie Ellyne, nutritionist formerly at Mills Hospital (where I used to work).
She ran pre-, mid-, and post-fast Zoom sessions for the five of us participants. We did check-ins and chair yoga.
All helpful!
The beauty of the plan is that when you get really hungry, you have some morsels to nibble, so it's easier than water-only fasts such as I have done previously. That matters, because those previous fasts were at a site where everyone was fasting, there was medical supervision, and opportunities to stray (i.e. eat) were absent. Prolon is done at home, in the course of ordinary daily life, where temptations abound.
But is the science real? Sure, I don't doubt it. The company claims to have done decades and millions of dollars of research and this, too, I don't doubt. They do call it "fasting mimicking" [italics mine] described as "...micro- and macro-nutrients in precise quantities and combinations that nourish you, but are not recognized as food by your body." But the real value, I believe, is simply the calorie restriction. The rest is window dressing and fancy packaging.
Why five days? They claim the duration is scientifically devised. I believe their marketing tells them that longer would be harder to sell. Cleverly, Prolon makes the five days relatively easy, with little disruption of our busy lives. Though -- I'm also certain -- the longer you fast, the more you benefit. No doubt their marketing is right. In the five days, I have lost five pounds... Hurray!
Would I do it again? Indeed I shall, perhaps quarterly (unless I repeat those stricter, longer water fasts.)
Go Prolon! And go nutrition-savvy nurses!
top
|
| |

Nursing
Education
2.0
February 20, 2023 --
Today I sat down with Sharon Goldfarb, DNP, RN, FNP-BC. We talked about nursing education, its shortcomings, and visions for improvement.
Until recently the Dean of Health Sciences at the College of Marin, Sharon is now an advisor at HealthImpact, the California Nursing and Policy center headed by Dr. Garrett Chan, which runs the Benner Institute for Teaching and Learning at my alma mater UCSF. It is a California State-funded nursing workforce development organization, billing itself as a "Revolutionary Solution to Remake Nursing Education and Support Professional Development for Nursing Educators". Sharon and I agreed that a revolutionary solution is sorely needed!
...read more.
Go enlightened nursing educators! Go Sharon!
top
|
| |

Kleptocapitalism
January 30, 2023 --
In today's JAMA, Salve Lucrum: The Existential Threat of Greed in US Health Care,
the venerable, conservative AMA complains of the cruel economics (they actually
call it a kleptocracy) of America's health care system.
The author is Don Berwick, former Administrator of the Centers for Medicare
and Medicaid Services under Obama. He knows of what he writes.
...Let's start here: regulate what I term
NoPINOs -- non-profits in name only (you saw it here first!) -- such as Kaiser
and -- especially called-out in this article -- Oak Street Health -- which
have special tax advantages in return for obligation to provide
services to broader populations. Today, instead, they
create "kleptocapitalist" grotesque wealth for those at the top of their hierarchies,
paying CEOs and others millions and even tens of millions of dollars.
Call those non-profits? As the humorist said,
there ought to be a law! But it's not funny.
...read more.
Go Dr. Berwick, go enlightened legislators, go principled clinicians!
top
|
| |

Covid
ICU
Watch the video.
What an ICU is really like. Great footage from nurse-worn GoPros.
I watched it when it came out and, two years later, it still moves me:
New York Times: Death, Through a Nurse's Eyes by
nursing hero Pat Benner (of my alma mater UCSF).
Been there, done that, hated it. I have nursed on Covid-infected units.
Here, the topic is Covid-infected ICUs.
California is the only state in the nation that has legally mandated
nurse staffing ratios.
In med/surg (the kind of nursing I do like) it's
5:1 (one nurse has up to five patients). In ICU it's 2:1. California is
enlightened. Be proud.
Go sustainably-staffed nursing units! Go Pat Benner! Go California nurses!
top
|
| |

Under
attack
December 20, 2022 --
My colleague and friend Karen Hunter, an informatics nurse and director at CommonSpirit Health, America's second-largest non-profit healthcare chain, spoke with me about how her work was hugely impacted by a recent cyber attack. (Becker describes it here and here.) Their computers were immobilized. 620,000 patient records were stolen. For Karen on the front lines it was a nightmare.
Even on a normal day, the job of the informatics nurse is challenging... Read more.
Go cyber-savvy informatics nurses!
top
|
| |

Guns!
Wise
regulation!
December, 2022 --
I have blogged previously about the endlessly ghastly problem of gun violence in America.
I (and many others) have observed that
it
is a public health crisis.
In recent years, much of this mayhem is done with assault weapons.
Part of the solution is, of course, legislation. My brilliant friend Dr. Jeff Johnson,
in a letter to the San Francisco Chronicle, proposed a most rational way to address this scourge:
Assault rifles are a danger to the public (6/20/2021)
...Assault rifles are NOT good for self defense
("Gun debate propelled by assault rifle's allure", June 20).
The rounds they fire are so high powered that they are a danger to people who are not
the target because they usually pass through the intended target and even through walls,
or they ricochet off hard surfaces creating showers of high-energy shrapnel.
Laws to restrict assault rifles should be based strictly on:
- The power of the rounds
they fire (proportional to bullet-mass x velocity-squared),
- How quickly successive rounds
can be fired,
- How many rounds their magazines hold, and
- How quickly magazines can be swapped.
Above a threshold on each of those measures, assault rifles should be deemed weapons of war
and banned for civilian use. Other aspects, such as whether they are styled to look military,
how many handles they have, or how they are named are irrelevant and should not be
factors in determining their legality.
Go Jeff! Go sensible regulation! Go life-saving public health legislation!
top
|
| |

Why Is Nursing
Time Management
Hard?
October 2, 2022 --
You know what it feels like: the shift ends and everything's done...
no staying late (on the clock? off the clock?) to finish charting,
no "missed care," all patients making good progress.
Effective time management is a great feeling: you're at your best,
and your patients have received truly good care. But how do you get there?
Time management is one of the hardest parts of the job of the nurse.
There is always more to do, and never enough time. Setting priorities,
not losing sight of the big picture, multi-tasking (especially while
juggling interruptions), and delegating are essential skills, subtle
and complex, acquired only with years of experience.
Here
are some of the issues I've confronted in my own practice.
Go time-managing nurses!
top
|
| |

Medical
disinformation
September 23, 2022 --
Lots of people believe things that are simply wrong. Why?
Social media are a powerful vector. In today's JAMA Network,
Social Media and Medical Misinformation:
Confronting New Variants of an Old Problem the reasons are summarized:
"declining trust in institutions, splintering of the media ecosystem,
deepening political polarization, and worsening economic inequality."
Real harm is done:
During the COVID-19 pandemic, for example, misinformation contributed
to the use of unproven treatments, nonadherence to mitigation measures,
and high levels of vaccine hesitancy... higher immunization rates
could have prevented nearly half of COVID-19�related deaths...
The temptation is to say that the platforms are neutral and
deliver only what users post. But in fact their algorithms are tuned
to "...promote extreme and sensational content with the goal of sustaining
user engagement." Their bottom lines are driven by eyeballs.
"Free" media are bought by advertisers. Advertisers pay for eyeballs.
Eyeballs are drawn by inflammatory material.
It would be contrary
to the incentives of Facebook, YouTube, Instagram, TikTok, Reddit,
Twitter, and Snapchat to turn down the heat. They could, but they won't.
They'd make less money.
Concludes JAMA Network:
Mitigating the effects of misinformation requires a multifaceted
approach that includes partnerships among clinicians,
public health officials, technologists, patient groups, and community leaders.
My own solution is simpler: Use social media only for social things:
keeping in touch with friends and family. Avoid the clickbait.
Don't look at political or "scientific/medical" postings on these sites.
If everybody did this, these problems would go away.
Go misinformation-correcting nurses!
top
|
| |

Nurses?
Models?
September 2022 --
When I first put up my web site
www.nursemind.com
with numerous images of nurses
(by a professional artist I'd hired) I got a surprising
amount of blowback from folks who didn't like them.
Here is why their opinions are ill-considered.
My policy regarding images of nurses is
to shun the typical marketing blather.
Unlike most nursing-related web sites, our
images are not of fashion models in tight scrubs.
Instead, the idea is to portray people as they
really are. Some are fat. Many are non-white; indeed,
ours is a majority-minority profession.
The world must learn to accept us however we look.
We are proud of what we do and what counts is the
quality of our work, not the svelteness of our physiques.
That big Black lady is doing a hard job and she's
doing it with intelligence and skill. (Of course,
she's running our nursing app on her smartphone.)
Maybe she's saving somebody's life. I hope that's
the message that people get from the image.
 As a counter-example, consider Nurse Jackie (played by Edie Falco).
In the TV series, she wears white scrubs
(only students wear white though Jackie is supposed
to be a grizzled veteran) and instead of scrubs pants
she wears a tight white skirt. I have never, not once,
seen a nurse dressed that way.
TV audiences may like to see that, but they won't
on the NurseMind web site.
As a counter-example, consider Nurse Jackie (played by Edie Falco).
In the TV series, she wears white scrubs
(only students wear white though Jackie is supposed
to be a grizzled veteran) and instead of scrubs pants
she wears a tight white skirt. I have never, not once,
seen a nurse dressed that way.
TV audiences may like to see that, but they won't
on the NurseMind web site.
Go, real life nurses!
top
|
| |

CPR:
wrong
default
September 10, 2022 --
In today's Medscape Should
We Always Offer CPR? Dr. Mallidi of our very own San Francisco General Hospital
(I loved working there) writes
movingly of CPR given ineffectually to a dying patient. Since no DNR nor Advance Directive
directed otherwise, medical staff was obliged to implement the default: all available measures.
To no avail, or worse. But why beat him up on his inevitable way out?
Dr. Mallidi suggests we change the default. She cites a proposal by physicians from
Columbia University Medical Center, Harvard Medical School,
Massachusetts General Hospital, and Boston Children's Hospital.
They proposed changes to how we decide whether to attempt resuscitation. Instead of CPR by default:
- Consider CPR when the benefits vs. risks are uncertain, and the patient is not end-stage;
- Recommend against CPR when there is a low likelihood of benefit and high likelihood of harm (e.g. patients with anoxic brain injury, advanced incurable cancer, or end-stage multiorgan dysfunction); and
- Do not offer CPR to patients who will die imminently and have no chance of surviving CPR (e.g. patients with multiorgan dysfunction, increasing pressor requirements, and those who are actively dying without a single immediately reversible cause).
And -- everybody! -- write that Advance Directive!
Go Dr. Mallidi! Go enlightened caregivers!
top
|
| |

Rethinking
nursing
informatics
August 31, 2022 --
I've been doing informatics for decades -- four decades, to be exact --
focusing on the sub-specialty of nursing informatics (NI) for the last of those decades.
You'd think it would be a mature technology... And you'd be right.
But much of the world hasn't figured this out yet.
Each quarter, my BANIA group delivers an educational event to address the question,
what is nursing informatics? You wouldn't need to do that for, say, car mechanics.
Everyone knows what that is. It's a mature technology.
So why, if my contention is correct, must we do so for nursing informatics?
Read the story here.
Go informatics nurses!
top
|
| |

Advance
care
July 14, 2022 --
Dr. Dan Morhaim urges caregivers not to shy away from sometimes-uncomfortable but essential
conversations with patients about their values and wishes regarding treatments in their final days.
Advance Care Planning documents and portable medical orders, he urges, are essential.
Today, in the authoritative journal Medical Economics, he published Why your patients need advance care plans. He writes,
We should be encouraging and assisting our patients to complete an advance directive and
to make sure these forms are electronically securely stored and readily available across
the healthcare continuum 24/7.
Dr. Morhaim is expert on POLSTs, MOLSTs, DNRs, Living Wills, Advance Directives, Durable Powers of Attorney, organ/tissue donation wishes, and the informatics mechanisms that make these documents accessible. His book Preparing for a Better End was published in 2020 by Johns Hopkins Press. Essential reading for anyone who expects someday to die. In other words, all of us!
Interested? Here are some recommended readings.
On Saturday, October 29th at 11:00 am PST, he will speak on this topic to our Bay Area chapter of the American Nursing Informatics Association. As informaticians, we are especially interested in learning about tools and methods to support the electronic availability of these documents. What good are documents if you can't find them when you need them? We informatics nurses can fix that.
Go Dr. Morhaim! Go informatics nurses!
top
|
| |

RaDonda
redux
May 13, 2022 --
We wrote earlier of our dismay at the criminal charges for the nursing errors of RaDonda Vaught.
Today we have the sentence: three years supervised probation.
Her mistakes were severe and she paid a high price -- career, license, and a lifetime of regret. But no prison time.
The nursing community has breathed a sigh of relief. We are vindicated in our belief that errors are not crimes.
Go justice for nurses!
top
|
| |

Overhaul
SNFs
May 11, 2022 --
Having worked in a few SNFs (skilled nursing facilities, i.e. nursing homes), I implore my children not to let me end up in one. Even the ones that don't reek of urine are depressing places. Even the ones that cost $8000/month. Let alone the ones that are largely federally-funded.
But change is coming. In an article today in JAMA, National Academies: US Nursing Home System Needs Fundamental Overhaul, the problems are identified and solutions proposed.
Problems
- Understaffing -- a critical problem.
- Funding and reimbursements -- "Medicaid, the dominant payer of long-term care services, doesn�t fully cover nursing homes� costs � especially the cost of providing quality care."
- "Predatory owners and operators who seek to maximize their profits at the expense of vulnerable residents� health and safety."
Solutions
- Improve low-paid nursing home workers� wages and benefits.
- Shore up minimum staffing standards and education requirements.
- Provide smaller and more home-like environments with single- rather than multiple-occupancy bedrooms and bathrooms.
- Incorporate residents' families experiences into enhanced quality measures in the Centers for Medicare & Medicaid Services (CMS) Care Compare website, where consumers can research facilities, for the first time.
- All health care professionals to receive geriatrics training, ideally with nursing home experience.
- Give state agencies that conduct nursing home surveys the resources they need to monitor facilities, investigate complaints, and enforce rules.
- Create incentives to increase adoption of electronic health records in nursing home facilities. (Yes! Go informatics!)
- Collect, audit, and make publically available data on nursing homes' often opaque finances, operations, and ownership.
- Develop a federal long-term care benefit. (I have long-term care (LTC) insurance; I don't count on the gummint to take care of me in my dotage.)
Go government reforms! Go SNF nurses!
top
|
| |

Wilderness
May 9, 2022 --
I just completed Advanced
Wilderness Life Support, a weekend of hiking and training in the woods by Lake
Tahoe. It was great.
 We practiced treating the ills that befall hikers, river rafters, skiers, and other
outdoorsy types as they revel in nature, far from urban health care systems.
Lightning strikes, snake bites, contaminated water, broken limbs, wounds,
diving accidents, sunburn, frostbite, and a zillion more.
How far do you go before you summon the helicopter?
We practiced treating the ills that befall hikers, river rafters, skiers, and other
outdoorsy types as they revel in nature, far from urban health care systems.
Lightning strikes, snake bites, contaminated water, broken limbs, wounds,
diving accidents, sunburn, frostbite, and a zillion more.
How far do you go before you summon the helicopter?
The course materials were developed at the U. of Utah School of Medicine.
Hey, if you love being a nurse -- and I do! -- you couldn't ask for a nicer place
to be it. And great teachers sharing their experience.
Go wilderness nurses!
top
|
| |

Criminal
error?
April, 2022 --
We nurses joke that a mistake by us could kill a patient so we must never cease to be at the top of our game. But it's not a joke -- it happened. So now the question is, is a medical mistake a crime? Should the nurse be punished?
The story is gripping nurses across the country. Here is NPR on March 25th:
RaDonda Vaught, a former nurse criminally prosecuted for a fatal drug error in 2017, was convicted of gross neglect of an impaired adult and negligent homicide on Friday after a three-day trial in Nashville, Tenn.
She has not yet been sentenced but likely faces years behind bars. Is that fair? Appropriate? This nurse says no. We make mistakes but we never intend harm.
We are passionate about our work and care deeply about and for our patients. The job is extraordinarily difficult, opportunities for error abound, and Nurse Vaught had unusually many obstacles on that fateful day. Her life is already ruined and her career is destroyed. If punishment is warranted (and I believe it is not) this is already more than enough. I urge the authorities to suspend whatever sentence their vindictive little hearts mete out.
Go overworked, imperfect but well-intended nurses!
top
|
| |

Data
in
the
rigs
April, 2022 --
My nursing informatics group BANIA (Bay Area Chapter of the American Nursing Informatics Association)
gives quarterly presentations on topics related to our work.
This quarter's talk is on the Emergency Medical Services Authority (EMSA) project.
Our speakers will be:
- Ian Brown (Medical Informatics Director at Stanford Emergency Services)
- Carlye Hatwood (Health IT - Assistant Chief Information Officer at San Mateo County Health, President-elect of BANIA)
- Tamara Muccia (Business Intelligence Health IT Director at San Mateo County Health)
- Dave Anderson - Project/Technical Analyst team member at San Mateo County Health)
The event will be Apr 25, 2022 from 18:00 to 19:15 (PT) online (Zoom). It awards 1 CEU of nursing training credit.
Register to attend here.
The system that will be described -- EMSA -- has a component named SAFR (search, alert, file, reconcile) that
provides patient data in realtime to the EMS personnel in ambulances ("rigs") as they transport patients.
It also alerts the emergency room what to expect.
In 2021 when I was employed by San Mateo County's health department I worked on this project.
My role included documentation for clinical staff and live testing as a ride-along.
It was fascinating, and is making a big difference in the coordination of caregiver
teams and in the quality of care being delivered. Click the pic to see me in action!
There's a lot of tech in those rigs!
Go EMS! Go tech-inspired nurses!
top
|
| |

Gov't
wants
SNF quality
April, 2022 --
This week, Centers for Medicare and Medicaid Services (CMS) proposed a rule on a couple of topics dear to nurses: safety and quality in nursing homes (SNFs), and nurse staffing there.
Some statistics were provided: Medicare pays "over 15,000 nursing homes, serving more than 1.5 million people.
Medicare spending to nursing homes is projected to be approximately $35 billion in FY 2022."
As we cannot manage what we do not measure, CMS proposes to add three important metrics to its value-based purchasing (VBP).
VBP rewards facilities with incentive payments based on the quality of care they provide to people with Medicare. These are:
- Skilled Nursing Facility Healthcare Associated Infections Requiring Hospitalization (SNF HAI -- hospital-acquired infections) especially Covid;
- Total Nursing Hours per Resident Day -- more nursing care correlates with improved outcomes; and
- Discharge to Community (DTC) -� Post Acute Care Measure for SNFs counts successful discharges to community from SNF settings.
Our government is listening, and we are moving in the right direction.
Indeed, Biden mentioned these things in his recent State of the Union Address.
Here is his FACT SHEET: Protecting Seniors by Improving Safety and Quality of Care in the Nation's Nursing Homes.
Having worked in SNFs, I have seen the good and the bad and care deeply about these issues.
So should you.
Go CMS! Go SNF nurses!
top
|
| |

I
got
rhythm
February, 2022 --
An insight about nursing from when I was a student and thinking deeply about it:
What makes an expert nurse?
I remember distinctly a comment made by one of my clinical instructors.
She observed that I was having difficulty finding my "rhythm".
Rhythm was a well-chosen word.
When you're an expert, you know without hesitation what is your top
priority, what to do now, what can wait, when something is a crisis and you must hurry,
and even more importantly when it's not yet a crisis but it could become one.
All these things are about time management.
Music, too, is all about time. Skilled musicians (for a few years in a former career this was how I
made my living, though having worked with a few geniuses I wouldn't have rated myself above
"competent") always know where "one" (the first beat of every measure) is.
Their job, too, is about time.
Finding that rhythm -- more a head thing than a hand thing -- is about mastery, flow.
Exhortations from our professor to find out when meds are due but not look
them up until time permits -- get our head-to-toe done first! -- help us
develop time management instincts.
Perhaps a better word than instinct is reflex.
A reflex is an action taken as a result of a decision made at a sub-cortical level.
When you know something thoroughly, you do it without having to think about it. You just know.
That's where I strive to get to.
I feel like it's a long way away yet, but at least I have a sense of where I want to go.
It will take years of practice to arrive at that sense of confidence, of mastery.
Someday I will have that rhythm.
Go nurses who've got rhythm!
top
|
| |

Hospital
at
home?
December, 2021 --
Kaiser is in the news again. As a cost-saving measure, it now promotes "hospital-at-home" --
care-at-home programs that use iPads and other digital technology for remote patient monitoring 24/7.
They conflate this with "aging in place" -- who doesn't prefer home to hospital?
But nurses slam the program. My nurse friend Ann Farrel points out,
Hospitals (bean counters) see RNs on balance sheet as largest expense labor [cost],
easy to cut to optimize profits though it's long proven RN hrs. per patient day
is a key driver of inpatient mortality and morbidity...
[I blogged about this here.]
Acute and critical nursing care cannot be replicated by family and technology
(often unreliable) connected to call center and visits by roving "care teams".
But what a money saver! We've forced lower RN staff, now let's transfer nursing
care to home and family unable to assume this role, even with patients wired to multiple monitors.
Another RN friend, Saskia, offers this nuanced view:
I'd rather see it as a choice. Some patients may be cut out for it.
However, after 'getting discharged home too early' now we have 'too early and without proper resources', double whammy.
No, we don't want nosocomial infections.
But people need to be over the hump, symptoms well-controlled, before going home.
Want top-notch nursing care, reliable and competent?
Don't expect it from family, often overtaxed and stressed-out.
Go to the hospital!
Go Ann! Go Saskia! Go inpatient nurses!
top
|
| |

We
SAFER?
December, 2021 --
The Office of the National Coordinator for Health Information Technology, funded by the HITECH Act
under the American Recovery and Reinvestment Act of 2009 has released the Safety Assurance Factors for
EHR Resilience (SAFER) Guides by Sittig et al, 2014. That's a mouthful.
What's the point?
Health information technology (HIT) -- most notably electronic health records (EHRs) --
is as vulnerable to cyberattack as any other industry, several of which have recently
sustained horrific and highly damaging assaults from miscreants both domestic and foreign.
Government systems as well as private enterprise (for example, earlier this year,
hackers shut down the Colonial Pipeline) have been attacked.
Health care institutions, too, are not immune.
Why fret about this here? Because nurse informaticists need education, skills,
and action to confront these threats. The SAFER Guides
outline approaches to informatics responsibilties including:
- High Priority Practices
- Organizational Responsibilities
- Infrastructure Design and Management
- Contingency Planning

- System Configuration
- System Interfaces
- Clinical Processes
- Patient Identification
- Computerized Provider Order Entry
- Decision Support
- Test Results Reporting and Follow-Up
- Clinician Communication
A video
introduction to these issues is available. Watch it!
"The SAFER Guides are self-assessment tools to help you and your team
identify these risks and mitigate them." And get smart about health data security.
Go nursing informatics security experts!
top
|
| |

Falls
December, 2021 --
Falling is, of course, a serious health risk and one often assessed by nurses. A popular tool for this purpose is the
Morse Fall Scale.
It is one of many such tools offered by NurseAssess.
To use the tool, click the radio buttons and then Calculate. The degree of risk is then displayed.
  
A helpful web site that describes fall risk factors and hazards, and prevention strategies, is
Sixty and Me. Recommended reading.
top
|
| |

A giant
has
passed
November 24, 2021 --
With great sadness we acknowledge the passing of a giant of nursing informatics.
Dr. Virginia Saba was a true visionary. "...Researcher, developer, and matriarch of the Clinical
Care Classification system" (In Memoriam: Dr. Virginia Saba).
She invented CCC, the best of the coding schemes for nursing data.
I have met her, discussed this, and blogged about it and about her
and again here.
Here is her autograph.
Go informatics nurses! Go Virginia and your disciples!
top
|
| |

Ageism
is
a thing
October 21, 2021 --
Ageism in health care? Is that a thing? You better believe it! And none of us is getting younger.
Here is the story: a panel of experts moderated by my friend Judy Graham of
Kaiser Health News,
Confronting Ageism in Health Care: A Conversation for Patients, Caregivers and Clinicians.
It presents statistics and issues as well as several personal stories that make the facts and figures real.
It's an hour and a half and well worth it especially if, like me, you are old, or caring
for someone who is. Or planning to be old some day.
How does health care fail us oldsters?
- We are often not involved in decisions.
- It is assumed that we are incompetent or cognitively compromised.
- We are often not heard and often not treated as fully human.
- We are omitted from clinical trials though new drugs and procedures are given to us anyway.
- Most medical education does not require training in geriatrics.
- It is often assumed that infirmity and pain are inevitable as we age and thus do not warrant attention.
- Another common assumption is that eventual relegation to institutions such as SNFs is inevitable.
- "Old people consume a disproportionate share of health care dollars."
But do we complain that children consume a disproportionate share of education dollars?
These are some of the negative results and claims of ageism and ageists in health care.
Judy's panel talks about what ageism is and what we can do about it.
Go Judy! Go elder-savvy nurses!
top
|
| |

Covid
future
October 12, 2021 --
Dr. Adam Lauring (my cousin, ahem)
is quoted in today's New York Times article,
What
the Future May Hold for the Coronavirus and Us,
predicting the future course of the Covid-19 pandemic.
"There was, I think, a sense [that the evolution of the virus]
would work in our favor, and that the nightmare scenario of it
being like influenza -- constantly changing and needing updated
vaccines all the time -- would probably not be the case,"
said Dr. Adam Lauring, a virologist and infectious disease
physician at the University of Michigan.
The article goes on:
Eventually, as viral evolution slows down and our immune systems catch up,
we will reach an uneasy equilibrium with the virus, scientists predict.
We will never extinguish it, but it will smolder rather than rage...
The future, [Dr. Jonathan Quick, author of The End of Epidemics]
said, "depends much, much more on what humans do than on what the virus does."
Translation: get your shots, people!
Go Adam! Go vaccination-dispensing nurses!
top
|
| |

We
have
Covid
 September 30, 2021 --
No, not the disease, the assessment.
September 30, 2021 --
No, not the disease, the assessment.
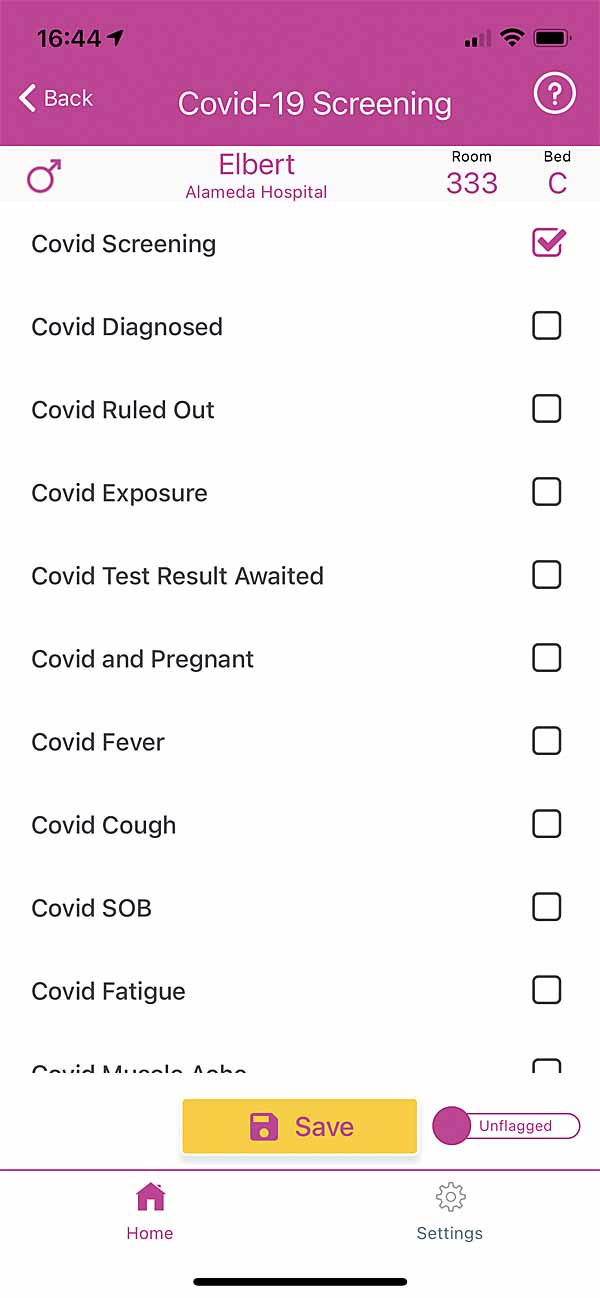
Now NurseAssess
users can screen their patients for Covid-19 and capture their findings in the app.
The data you enter into this app screen are encoded as ICD-10-CM assessments
and uploaded to your EHR when you click "Save".
Useful and timely.
Go NurseAssess!
top
|
| |

NY TriState
Chapter of ANIA
September 25, 2021 --
Today I gave a brief presentation at the Symposium of the NY TriState
Chapter of the American Nursing Informatics Association (ANIA).
My topic was the research results in the Doctor of Nursing Practice (DNP)
thesis of recently-graduated student Stella Eliboh RN and now DNP.
She studied the issues related to the use of professional-grade
mobile applications (apps) by nurses on the job. Her case study
subject was my new NurseAssess app.
Here is my Powerpoint.
The nurse informatician attendees were gracious and my talk was well-received.
As seasoned bedside nurses, all shared our professional vexation with the
documentation burdens of our work which motivated development of
this app. Often we must spend more time with the computer than with the patient.
The app offers a step toward overcoming this, and this audience "got" it.
Go NY TriState nurses!
top
|
| |

Dottoressa
September, 2021 --
I just finished reading Dr. Susan Levenstein's wise and witty
Dottoressa (2019).
She recounts her experience as an American doctor
in Rome where I grew up. We are contemporaries and
I recognized several of the people she mentions whom I
knew during the years (1961-1973) I lived there. Also of
great interest are her reflections on medicine and health
care systems about which I, too, have many opinions (as
readers of this blog are surely aware).
Perhaps my favorite part of this book is Dr. Levenstein's
observations on Italian culture -- its quirks, the wisdom
and superstitions of its people, and their
endless "medical" strictures.
Here are some I, too, have observed: Don't swim after
eating... never mind science, this is your mother speaking.
Got the sniffles? Must be from a colpo d'aria
(hit of air) from that open window.
Feeling unwell? It's surely your fegato (liver).
It's always the fegato.
Dr. Levenstein's timely and polemic blog -- she waxes
strident and well-informed on matters Covid --
is at www.stethoscopeonrome.com.
Highly recommended.
In Rome for a couple of weeks' vacation (July, 2021)
I called her up. She was most welcoming to this stranger
and we had an aperitivo and a chat.
With our Italophilia and medical backgrounds in common,
there was much to talk about. Thank you, Susan!
Go expat doctors! And nurses!
top
|
| |

ANIA
2021
August 7, 2021 --
I'm home now from yet another enjoyable and educational American Nursing Informatics Association (ANIA)
national conference, held this year in San Diego.
We're all vaccinated so Covid worries were none. Hurray, no masks!
And as far as I know, there was no super-spreading.
 In the photo: front row: half the Board (Helen Lu, Tip Tilton, Dan Keller) of the Bay Area (BANIA) chapter.
Back row: half the Board of the San Diego chapter (Matthew Binder, Kathy Topp).
In the photo: front row: half the Board (Helen Lu, Tip Tilton, Dan Keller) of the Bay Area (BANIA) chapter.
Back row: half the Board of the San Diego chapter (Matthew Binder, Kathy Topp).
Hot topic of the day? "Documentation burden" on nurses. In other
words, too much time in front of the computer. Evidently, it's a
national goal to re-engineer these processes and UIs to reduce
this by 75% within a couple of years or so.
While well-intentioned, this misses the point. It's not that we have to
do too much documentation (though we do) it's that the job
definition is misguided. Much of the excessive picking and
clicking is driven by that "doctor's handmaiden" view of nursing
that we can't seem to shake.
It's nit-picky because it assumes
no clinical judgment; we must be prompted for every detail
because we wouldn't think of (or do) it independently. (No one
said these things in the presentations; it's my own opinion.)
Nostalgia was expressed for the charting-by-exception
we used to do in the "good ol' days" of paper charts. I do
remember that. We got our charting done quickly
that way. An efficient process that has been lost in the
transition away from paper. I guess I'm an old-timer,
sigh. Somebody even wistfully mentioned the Kardex.
The youngsters just said, "Huh?"
Go wise old nurses and smart, up-and-coming young ones!
top
|
| |

Hesitancy
schmesitancy
July, 2021 --
Why call it "vaccine hesitancy"? That legitimizes what must be
called what it truly is, idiocy. These fools imperil themselves
and those around them. A cynic might call it natural selection
or Darwin awardees.
Denial of science and well-established public health principles
will remove them from the gene pool. In other words, Covid kills.
A kinder view
(The Atlantic,
Sept. 2020, "How the Virus Won")
ascribes this idiotic behavior to complacency:
Vaccines eradicated smallpox and polio, and brought measles, diptheria,
and rubella to heel... These achievements brought complacency.
In fact, I have known people of my parents' generation
crippled by polio. Suffering and death brought by uncontrolled disease
was ended by science not many generations ago; have we already forgotten?
The
evidence is indisputable. Covid death rates are inversely proportional
to vaccination rates. Less vax, more death. Simple numbers.
They are not "hesitant". They are fools.
To my amazement, there are even some nurses among them.
We are taught -- above all -- to practice safely. Do no harm.
Would these nurses infect their patients?
They should be banished from the workplace until they're vaccinated or
the virus subsides.
Especially in nursing homes!
45%
of Nursing Home Staff Still Unvaccinated Against COVID-19 --
Why do these
Typhoid Marys still have licenses?
Go vaccinated nurses!
top
|
| |

Go
nursing
informatics
June 1, 2021 --
Are you a nurse? Of course you are; otherwise you wouldn't be reading this.
Do you use computers in your work? Of course you do; we all do, especially for the electronic medical record.
Do you design, build, implement, train or support users of those systems? Aha, maybe not; this is a nursing specialty still in its infancy.
If you do do this, you're a nursing informaticist. You're one of us.
 And you should be a member of the American Nursing Informatics Association.
If you live in the Bay Area, you should also be in our local chapter, BANIA.
And you should be a member of the American Nursing Informatics Association.
If you live in the Bay Area, you should also be in our local chapter, BANIA.
Why? Many benefits, especially professional networking. But what does that mean?
- Looking for a job or a gig? It's who you know.
- Solving hard problems? Discuss project strategies with others tackling similar issues.
- Share experience and wisdom.
- Keep on top of the hot issues of the day.
- See what others are working on; you may soon work on those things, too.
- Hobnob with the movers and shakers in our industry.
- Attend conferences and see the cutting edge.
Another benefit is free/cheap CEUs (continuing education units):
- In California, to maintain our RN licenses, we must get at least 30 hours every two years.
- Attendance at conferences, workshops, and webinars often yield CEUs and are offered by ANIA and BANIA.
Go informatics nurses!
top
|
| |

LACEd
Up!
April 30, 2021 --
We are proud to announce a valuable addition to the widely-used LOINC clinical terminology standard.
This addition is the LACE scale.
It identifies patients who are at risk for readmission or death within thirty days of discharge.
This is of great import to hospitals in deciding whether and when it is safe and appropriate to discharge a patient.
Readmission or death of a patient within thirty days of discharge is considered an "adverse event"
and can result in a financial penalty to the hospital from Medicare as a provision of the Affordable Care Act.
For the sakes of both the hospital and the patient, premature discharges are to be avoided.
Read more...
top
|
| |

Covid
Staffing?
March 1, 2021 --
A perennially hot topic in nursing is staffing ratios: for how many patients does a nurse care at one time? It is well-proven that keeping these low saves lives. California alone in the nation legislated nurse staffing ratios with Assembly Bill AB394 in 1999.
(Hospitals opposed it because payroll -- specifically nursing payroll -- is their highest-cost budget line item.)
Several factors must be considered, mainly the acuity of the patients' conditions and the type of nursing unit. For example, the level of care required in an ICU is much higher than in med/surg. And, of course, when there is a pandemic everything is impacted.
Read more...
top
|
| |

New
blog
March, 2021 --
After 16 years of blogging at this location (wow! we are proud!)
we're moving.
Going forward, please come see us at
NurseAssess News!
New location, new up-to-date look, same feisty nurse activism.
See you there! Go nurses!
top
|
| |

Vaxes
'r
us!
January 12, 2021 --
Spectacular logistical triumph by my new employer, San Mateo County Health Department's
Coronavirus
program: 3000 cars/day processed in drive-through vaccinations.
It's been running most of January and will continue until all San Mateans
are immunized.
(My photos.)

|
Ours is the first California county to get such a program into operation
(San Diego is #2).
Each occupant briefly rolls down their window, gets the Covid shot, proceeds
to 15-minute pause to make sure of no adverse reaction, and done.
|
The result?
- We health workers can give care without fear.
- Teachers can return to their classrooms.
- People can go back to work.
- Grandparents can hug their grandchildren.
- Back to normal? We're getting there!
|
|
Sounds simple... not! Logistical challenges include managing signups (online),
confirming identities,
managing materials (ultra-cold freezers store vaccines), tracking who's
received what (the Moderna vaccine, in our case) and when they are to receive
the booster (after 4 weeks), the huge facility (San Mateo Event Center),
security, traffic direction, and more.
My tiny role (job title: Clinical Nurse Informatics Educator)
was IT support. And as a healthcare provider I, too, got the shot.
Hurray!
|

Dan gets the shot.
|
top
|
| |

Biden?
Hey!
Nurses!
November 2020 --
My newest nurse hero: Jennifer Shepherd.
She looks at president-elect Biden's Covid task force and
asks, where are the nurses?
"NO other profession in the world understands and deals with this more than we do!
You don't get to claim nurses as heroes, be thankful for our work, and then not include us at the table!"
And everyone knows, if you're not at the table you're on the menu.
Go Jennifer! Go nurses!
top
|
| |

How to fix
the pandemic
November 4, 2020 --
In a succinct article,
Seven
Ways to Fix This Pandemic -- and Stop the Next One, Medscape maps out for
us the sensible steps we must take.
I hope Biden's listening.
Trump sure wasn't.
Clear thinking like this gives me hope.
top
|
| |

Wear
that
mask!
November, 2020 --
The reason this virus is so elusive and virulent (rapid-spreading) is its two-week incubation period.
People spread it when they don't yet know they have it. Most devious, that virus!
The defensive strategy is obvious though, evidently not to everybody including our president:
you could have the virus without knowing it, so wear a mask just in case.
This will prevent you from spreading it to other people. Duh!
top
|
| |

Herd
immunity?
November, 2020 --
In an October 19, 2020 JAMA article,
Herd
Immunity and Implications for SARS-CoV-2 Control by Saad et al is an
excellent and succinct explanation of herd immunity.
We all want society to return to normal. Can we do that through herd immunity?
This article gives the answer. I summarize it here.
What is immunity? Having the antibodies that protect you from the virus.
How do you get these antibodies? Either by catching the virus and growing
them yourself as part of the defense process or by getting them from a vaccine.
What is herd immunity? It is when enough people have immunity that exposure
to the virus of people who don't yet is infrequent enough that the virus dies out.
What percentage of the population must have the antibody to reach herd immunity?
This number is different for each communicable disease.
For Covid-19 it's 60%.
What percentage has it today? The article posits 10% but admits that this is
an assumption.
How long will it take to get from 10% to 60%? The article doesn't say, but my
guess is 10 years if we have no vaccine, sooner if we do.
How much quicker? It depends on how many people are vaccinated and how soon.
The USA has a population of 330M. Assuming that 33M (the article estimates 10% of
the population) have grown the antibody themselves, 330M x 0.6 - 33M = 165M would
need to be vaccinated to get us to herd immunity. To deliver that number of
vaccinations will demand a massive manufacturing and distribution infrastructure.
It's a tall order but we're doing it!
There is an additional factor: the duration of the immunity.
The article guesses 2 to 3 years but admits that this is not yet known.
If immunity is shorter, the percentage of population requiring immunity
is substantially higher.
Conclusion? "...infection-induced herd immunity is not realistic at this
point to control the pandemic." We've got to have that vaccine.
Go JAMA!
top
|
| |

Incompetents
in
charge
October 8, 2020 --
Traditionally, the venerable NEJM (perhaps the world's
premier healthcare mag) has stayed clear of politics.
Clearly, we've reached a tipping point.
This scathing editorial, Dying in a Leadership Vacuum, is eloquent on
the topic of our Idiot-in-Chief: Though they don't name
him, much of this failure can be laid squarely at the feet
of Donald Trump: "[He has] taken a crisis and turned it
into a tragedy."
How did NEJM reach this conclusion?
Here are just a few of the compelling points
(quoted from the editorial):
-
China [held
its] death rate to a reported 3 per million, as compared
with more than 500 per million in the United States... In
general, ...many [countries] ...have outperformed us by
orders of magnitude.
-
We had ample warning [and squandered it].
-
We continue to be way behind the curve in
testing. [In] the number of tests performed per infected
person [we are] below such places as Kazakhstan, Zimbabwe,
and Ethiopia, countries that cannot boast the biomedical
infrastructure or the manufacturing capacity that we have.
-
Quarantine and isolation are sloppy or not
done at all. Masks are often not worn, largely because our
leaders have stated outright that masks are political tools
rather than effective infection control measures.
-
The government has appropriately invested
heavily in vaccine development, but its rhetoric has
politicized the development process and led to growing
public distrust.
-
Anyone else who recklessly squandered lives and money in
this way would be suffering legal consequences...
[In] the
largest public health crisis of our time, our current
political leaders have demonstrated that they are
dangerously incompetent. We should not abet them and enable
the deaths of thousands more Americans by allowing them to
keep their jobs.
The editorial is a quick read and an excellent
summary of our unforgiveably mishandled crisis... no, tragedy.
Go NEJM!
top
|
| |

Medicare
and
YouPays
October, 2020 --
I am 66 and I've had Medicare for a year.
My parents (may they rest in peace) had it, too (as do most 65+ Americans) and were pleased although,
in his last two days of life, my father was not afforded a private room in the hospital
(Mt. Sinai in New York City which we dubbed Mt. Cyanide) and we
-- an endless stream of family paying last respects and we three his distraught offspring --
had to tiptoe and whisper so as not to disturb the saintly heart patient in the other bed.
Medicare is no Rolls Royce.
And it's complicated! Ok, I get the distinction between Parts A, B, and D (yup, there's no C). But that's just the beginning.
...read more
top
|
| |

EHR
Burdens
September 17, 2020 --
My friend and hero Patty Sengstack DNP RN-BC FAAN
is leading yet another ground-breaking
project, documented in an American Nursing Informatics Association
(ANIA) position paper:
The
Six Domains of Burden:
A Conceptual Framework to Address the Burden of
Documentation in the Electronic Health Record.
I have groused about
the
heavy toll taken by EHRs on nursing
and welcome Patty's formal analysis.
Central to the concept of burden is what the authors
term "The Six Domains" -- the reasons why we use
EHRs and why they make nursing work more
onerous. I have pontificated elsewhere about
the motivations for EHRs
and how they are the opposite of what I term
"nurse-centric". The "burdens" are:
- Reimbursement (charge capture)
- Regulatory (keep the gov't off our backs)
- Quality (proof that we're doing a good job;
when we do a great job our hospitals are paid more
thanks to value-based pricing)
- Usability (with time we'll get this right but
today the perception is that working the computers
is slow and painful)
- Interoperability (data entered in one system
must often be re-entered in another)
- Self-Imposed: "We've done it to ourselves"
(artifacts of institutional culture and
control/power structures)
Let me be clear, however, that I am an enthusiastic
advocate of this technology. In graduate school
(1978-1983, UCSF)
my
master's thesis
(and resulting publication) was an EHR
I programmed from scratch and that was briefly
used in live clinical practice (as proof of concept
only). I am convinced that well-designed
and well-implemented clinical data systems can and
already often do much to improve quality of care,
efficiency, accuracy and above all safety.
However, there is also a strong case to be made
that these systems sometimes have the opposite effect.
One thing that makes Patty's paper especially
valuable is that for each of the six burdens it
gives real-life examples,
most of which will be recognized
by nurses and other clinicians from their
experience of their professional environments.
On reading it, many will be tempted to say,
"Amen, amen!"
Go Patty! Go nurses!
top
|
| |

Innovate!
Perform!
September 12, 2020 --
Our Bay Area Nursing Informatics Association chapter (BANIA)
today delivered its summer educational event,
"Leading Innovation and Creating Cultures of High Performance"
taught by industry luminary
Dan Weberg RN PhD who works at Trusted Health
that provides tech-savvy nurse staffing services. (That is, the services are tech-savvy...
I hope the nurses are, too.)
He described several disruptive and innovative activities in health care.
(I've blogged about him before.)
One is a
healthcare focused division at Microsoft,
spearheaded by Molly McCarthy, pictured above.
Here is one of her podcasts,
on nursing, technology, and the key focus areas at Microsoft.
Her title is Chief Nursing Strategist (wow! where do I apply for a job like that?)
She builds cloud- and AI-based tools for clinicians.
Other innovators in healthcare mentioned by Dr. Weberg include
Amazon, Google, Apple, and Walmart. Big tech senses big dollars.
(He didn't say that, I did.) It was a great talk.
Go nurse technologists!
top
|
| |

Droplet? Airborne?
Aerosol? All of the above!
July 25, 2020 --
We used to think that the Covid-19 virus was transmitted
only by droplets in the air (and, less commonly, on surfaces we touch).
Droplets -- a term with a very specific meaning in nursing, and
clear protocols we must follow in caring for patients who require
droplet precautions -- can travel up to six feet before
falling out of the air and ceasing to pose a threat.
How Is SARS-COV-2 Transmitted?
published today by the nurses union, National Nurses United
(NNU), claims otherwise.
Recent studies show there are also aerosol and airborne components
in the transmission process. These travel much farther than six feet,
and remain airborne longer. The danger is worse than we'd feared.
Go nurses union! Educate us and keep us safe!
top
|
| |

Covid Screening
in Madison
July 14, 2020 --
Today I received on-line training to become
a volunteer nurse screener
of guests in a couple of shelters
(one for women, one for men) in Madison, WI.
The screening process, too, is conducted on-line.
Folks wishing admission to these shelters
(Porchlight and Salvation Army)
must first stop and talk with me or one of the other
volunteer RNs via an Internet-connected tablet.
We screen them for Covid symptoms, make sure they're
wearing their mask correctly, and if necessary,
triage them to a hotel (funded by Dane County, WI)
or to a nearby ED.
The brainchild of nurses
Tracy Zvenyach and Epic
veteran Bre Loughlin (pictured above),
this program is called Nurse Disrupted.
To date, four dozen people like me
have signed up, been trained, and staff it
seven days a week, one shift a day in each of the
two facilities.
Forty to fifty shelter guests are screened
in a typical shift.
There have been no outbreaks of
Covid in either. Evidently Nurse Disrupted is
working well.
Go Wisconsin nurses!
top
|
| |

Goodbye
Zakheim
June, 2020 --
Among my fond memories of studenthood at UCSF are the WPA-era murals by Bernard Zakheim
in UCSF's Toland Hall. One of my classes was in this hall and it was a joy to attend.
Toland Hall is in the handsome but obsolete UC Hospital building on the Parnassus campus.
UCSF plans to demolish the building and replace it with one that's up-to-date,
seismically safe and, alas, mural-less. Preserving them would cost millions
and the money is just not there.
Here are my photos of these
stupendous works. Go see them for yourself while you still can!
top
|
| |

Clinicians
and
computers
June, 2020 --
As I have blogged before, clinicians are ill-served by technology,
EHRs in particular. EHRs' primary purposes are:
- Data gathering (legal and regulatory), and
- Billing
...not supporting clinicians.
Here is my recent first-person essay on what this is
like for this nurse.
Cartoon by
Charles Keller (Dan's Dad)
top
|
| |

RN
=
IT
June, 2020 --
A new meaning for the term nursing informatics?
I have blogged at length here about nursing informatics.
Recent experience adds a whole new layer: tech support for patients.
This is a thing.
Requests from patients on a variety of units
where I have worked recently have been for things like,
"My phone's charger cable broke; can you find me another?" or
"How do I get a network connection so I can Skype with my family?"
Especially in these times of Covid-19 when inpatients are increasingly
isolated -- for infection control, visitors are no longer
permitted -- technology is essential for human contact.
And often the only way to get tech support is to ask a nurse.
A new challenge! Go nurses!
top
|
| |

What
SNFs
must
do
May 28, 2020 --
In an excellent article, Asymptomatic Transmission, the Achilles' Heel of Current Strategies
to Control Covid-19, the venerable New England Journal of Medicine (NEJM)
offers a strategy for SNFs to combat the Covid-19 pandemic that's killing their residents:
- Expand Covid-19 testing to include asymptomatic persons residing or working in SNFs.
- Isolate infected residents and care for them appropriately.
- Quarantine exposed residents to minimize the risk of spread.
- Cohort residents and resume some group activities in nonoutbreak settings.
- Do routine rRT-PCR testing
in addition to symptomatic screening of new residents before entry.
- Apply conservative guidelines for discontinuation of isolation.
- Periodically re-test long-term residents.
- Periodically rRT-PCR screen and surgically mask all staff.
- Extend these recommendations to all US-based SNFs.
These are excellent recommendations. What are the chances that they will be implemented as legislation?
I'm not holding my breath.
top
|
| |

Eating
my
own
dogfood
May, 2020 --
Among programmers, using the products you build is referred to as eating your own dogfood.
I've been doing that.
That is, on my nursing shifts, I've been using my new app,
NurseAssess

The verdict?
I love it! Of course, I am biased. Everyone thinks their own baby is beautiful.
Still, the app (entering vital signs and nursing assessments straight
into the smartphone) compared to the conventional method (jotting them on scraps of paper and
later typing them into the computer) is so much faster and more accurate.
Seems like a no-brainer!
Dogfood, anyone?
top
|
| |

In
defense
of
SNFs
May, 2020 --
SNFs (skilled nursing facilities, at one of which I work) have been getting a bad rap lately.
Their residents suffer a disproportionate share of Covid-19 deaths. The implication in a recent spate
of articles in the press is that these institutions have delivered substandard care or worse, driven
by rapacious administrators and capitalistic owners to cut corners and let patients sicken and die.
While such abuses have surely occurred, I maintain that these are a vanishingly small minority and that
very nearly all such institutions have performed well, even in the face of daunting odds. What are those
odds? They are two:
- SNF residents are by definition the most vulnerable demographic: elderly beset by numerous
comorbidities, often surviving by the merest thread sustained only by, well, skilled nursing.
Throw a deadly virus into this mix and the outcomes are inevitably poor.
- The designs of these places are commonly outmoded. If we were to redesign them today
(and many have, for example
the
New York Times: As Death Toll in Nursing Homes Climbs, Calls to Redesign Them Grow)
each resident would have a private room.
The HVAC/ventilation systems would exhaust to the outdoors instead of recirculating. Shared spaces
would support social distancing. The number of residents in a nursing unit ("pod")
would be perhaps a half dozen instead of the two or even three dozen common in today's
SNFs, most of which were designed many decades ago.
So today the odds are against us. What can we do? Bulldoze and rebuild? Where's the money for that?
In practical terms, let's do what's possible within the constraints of reality, and point
fingers only when the malfeasance is real. Which it rarely is. In defense of SNFs, please
understand the realities. And go (skilled) nurses!
top
|
| |

Big
babies
May, 2020 --
A recurring theme in right-wing screeds is the unuttered yet
essential assumption that they can do crazy stuff knowing
that responsible people will keep them safe and clean
up their messes.
An obvious example is the folks protesting
the coronavirus lockdown. They know perfectly well that if
everybody stopped sheltering-in-place as they demand,
the virus would run rampant and many more would sicken and
die. They don't say it out loud but they count on being
prevented and thus safe.
Another is the anti-vaxxers. Idiots!
And there's the environment. If the
regulations that keep our air, water, atmosphere, oceans,
fisheries, wetlands and forests functioning were withdrawn,
our planet would soon fail to support life, especially
human life. They know this, and count on the people
they attack to protect them.
This hypocrisy must be exposed and it must end. The
problems are too big and too fatal to play games.
Right-wingers,
stop counting on "the adults in the room" to change
your diaper. Grow up, you big babies!
Nurses, of course, are among the realists. We know the
real issues and what it takes to keep everybody healthy.
We are the adults in the room.
Go nurses!
top
|
| |

Nursing
in
Covid
times
April, 2020 --
In most ways, it's no different than nursing in normal times.
Except for two things:
One: wiping, wiping. I used to be able to take a set of vitals
in about four minutes. Now that is more than doubled by the time
it takes to wipe down the thermometer, pulse oxymeter, blood
pressure cuff/tube/gauge between patients. It's a real
hindrance and I must remind myself not to get sloppy. Lives are
at stake.
Two: PPE (personal protective equipment).
I wear (going from head to toe as nurses are taught)
hairnet, face shield, N95 mask, disposable gown, gloves
(sometimes doubled), booties. Communication with coworkers is
rendered difficult by the muffling of mask and face shield.
Most are immigrants with strong accents and this makes it worse.
We tire of having to repeat everything but what else can we do?
And there's a third thing: fear. Mine. When a
Covid+ patient coughs in my face as I'm affixing a blood pressure cuff
I wonder, was that it? The moment the virus nails me? I leap back
but of course those droplets travel faster than I can.
I wipe down doorknobs, faucet handles, handrails. Then someone says,
did you wipe your steering wheel? And I'm, OMG. There's always
something more. After a while these thoughts are exhausting and I
grow resigned. So far I've been lucky. How long will that last?
I do what's possible and that has to be good enough. What happens
will happen and we'll come out OK in the end.
top
|
| |

NEJM
on
SNFs
April 24, 2020 --
Here in the venerable NEJM is Presymptomatic SARS-CoV-2
Infections and Transmission in a Skilled
Nursing Facility. It posits:
"Infection-control strategies focused
solely on symptomatic residents were not
sufficient to prevent transmission after
SARS-CoV-2 introduction into this
facility."
This should frighten anyone
who goes or whose loved one goes into
such a facility.
The facts are
perhaps worse than the article
describes. In the SNF where I work, we
use infection-control strategies for all
our residents, not only the symptomatic
ones. Yet upwards of 70% in my unit
(my unit is the Covid unit; this is not
facility-wide) tested positive for the
virus last week. The previous week it
had been 10-20%.
When a worker has symptoms or tests
positive, he/she stops coming to work.
(So far, I am negative, thankfully.) But
when a resident tests positive, what can
we do? Sending them home is not an
option (as I have discussed in an
earlier blog posting, "sitting
ducks".) SNF residents with their
numerous comorbidities comprise by far
the most vulnerable demographic.
My facility is doing everything the NEJM
article recommends:
- Restricting
visitors and nonessential personnel from
entering the building
- Universal
use of face masks by all staff
- Strict screening of staff
Beyond these, we do frequent
hand-washing, use full PPE, and wipe
with bleach our instruments between
patients. Even so, nearly all the
residents of my unit have caught the
bug. In close quarters, it is
indomitable.
We are at the limit
of what's possible. Yet the near-term
outlook is poor.
top
|
| |


SNF
musings
April, 2020 --
I have had the good fortune to remain in contact with the best of my
teachers from the various levels of my education. In grad school, among my
most inspired and inspiring were Drs. Azad Bolour and Hyo Kim who, at UCSF,
taught, respectively, databases
(essential to my work to this day) and emergency medicine (that
informed my stints as an ER nurse).
They read my recent
blog about SNFs
and, unsurprisingly, had insightful (and, again, inspiring)
responses.
"I congratulate you for being so brave to volunteer
your services to the emergency situation.
You may want to describe more of your emotional response which maybe more compelling.
Many medical professionals are having debate as to how much to
sacrifice of yourself to help in this situation.
One small misstep can ruin your own life and end everything.
Let us keep updated as to your decision to proceed."
So I have been thinking about that: what are my feelings regarding
my SNF patients, an elderly population with numerous comorbid chronic
conditions? What are my feelings about SNFs? And what about
the risks I take in working in a Covid-19-ridden SNF? Read
my diary if you're interested.
top
|
| |

Sitting
ducks
April, 2020 --
I am volunteer-nursing on a unit in a local SNF (skilled nursing facility).
Nearly all our patients have tested postive for Covid-19.
We caregivers do all we can to prevent the spread of the virus. We:
- Get tested regularly and cease work if we're positive.
- Use PPE (N95 masks, disposable gloves, face shields, hair nets, bootees, disposable gowns).
- Wipe down our equipment (blood pressure cuffs, thermometers, etc.) after each use.
- Change gloves between patients.
- Wash hands at every opportunity.
- Put a mask on anyone who has tested positive and on others when possible.
Even so, the virus spreads. Like a fog it surrounds its carriers and settles everywhere.
Calling it a fog is not quite accurate since the virus is droplet-borne not dry, but
I find the mental image useful. A virus is DNA or RNA surrounded by a thin fatty shell that
is easily dissolved by soap or solvents thus destroying it. The problem is that the "fog"
settles everywhere. Washing and wiping cannot reach every place the virus lands.
The CDC is well aware of the risks and has published guidelines to reduce them.
Both patients and workers are at risk, me among them, and I worry.
Eliminating visits from outsiders and group events are
essential measures but they don't solve the underlying
problem, people in close proximity. Not much can be done about
that short of closing the facilities and sending everybody home. Even if that
were an option, it would merely displace not solve the problem. Alas, there is
no good solution. The best we can do is to continue to be careful and do what we're
already doing.
We'll be living with this virus for quite some time to come.
top
|
| |

Nursing
plans
dead
April, 2020 --
A positive side effect of the coronavirus pandemic is the forced
streamlining of healthcare procedures.
Nurses in acute care facilities are permitted to
omit the redundant and largely pointless step of creating
nursing care plans. It's about time!
These were largely duplicative of physician's orders.
No one ever reads them.
Nursing students are required to write them endlessly
though it is well understood that the exercise is a waste of time.
See, for example, Death to Nursing Care Plans!
in the American Journal of Nursing.
The entire industry needs to relinquish this obsolete practice.
Thank the virus for rubbing our noses in the obvious.
Go nurses. Go streamlined workflows!
top
|
| |

Informatics
for
pandemics
March, 2020 --
You thought electronic health records were a technical detail,
an obscure tool, an esoteric subspecialty
on the periphery of modern health care?
Think again.
As Rapid Response to COVID-19:Health Informatics Support for Outbreak Management
in an Academic Health System (get it here if that link is broken)
from UCSD Health demonstrates,
the EHR is central to confronting the COVID-19 pandemic.
It is an essential tool to:
- Support management of patients in a standardized way
- Enable immediate widespread distribution of information
- Track transmission in real-time
- Provide virtual venues for meetings and day-to-day operations
- Manage the inventory and distribution of essential supplies
- Offer telemedicine visits for patients
Go nurses. Go nursing informatics!
top
|
| |

Coronawisdom
March, 2020 --
Brilliant, recently-retired Kaiser intensivist Tricia Bell shares the following wisdom about our coronavirus miseries.
The number of reported cases vastly underestimates the true prevalence
in our population because the availability of testing is still far from adequate.
The danger, therefore, will almost certainly increase over the next few weeks.
Public health department recommendations tighten up significantly every 12-24 hours.
Following exactly what they do or don't recommend today looks insufficient tomorrow.
We should stay ahead of the curve to protect our entire community.
This article
explains the fallacy of the "it's not much worse than the flu" argument.
This persuasive article
is about the necessity of instituting social distancing ASAP.
This article
shows how the pattern of exponential spread has been virtually identical from country to country,
except in places like Taiwan where they instituted tight restrictions early.
 This video interview
with one of the intensive care specialists who is leading the efforts in Italy is both
fascinating and terrifying. The coordination between hospitals and ICUs in Lombardy has
been stunningly intelligent and rapid. We'd be lucky to do as well in the US.
The message for us is that he sees enforcement of maximal social distancing as the only hope
to avert total breakdown of the health care system. They have not been forced to ration ICU beds,
ventilators, or personal protective equipment yet, but at the rate cases are rising,
they could be in that position within a week. And Italy has more ICU beds per capita than we do.
This video interview
with one of the intensive care specialists who is leading the efforts in Italy is both
fascinating and terrifying. The coordination between hospitals and ICUs in Lombardy has
been stunningly intelligent and rapid. We'd be lucky to do as well in the US.
The message for us is that he sees enforcement of maximal social distancing as the only hope
to avert total breakdown of the health care system. They have not been forced to ration ICU beds,
ventilators, or personal protective equipment yet, but at the rate cases are rising,
they could be in that position within a week. And Italy has more ICU beds per capita than we do.
Wash your hands. Keep socially distant. Stay safe. We'll survive this one!
top
|
| |

Wrongheaded
graph
March, 2020 --
I have seen this graph copied and pasted into numerous web sites and emails
about the coronavirus.
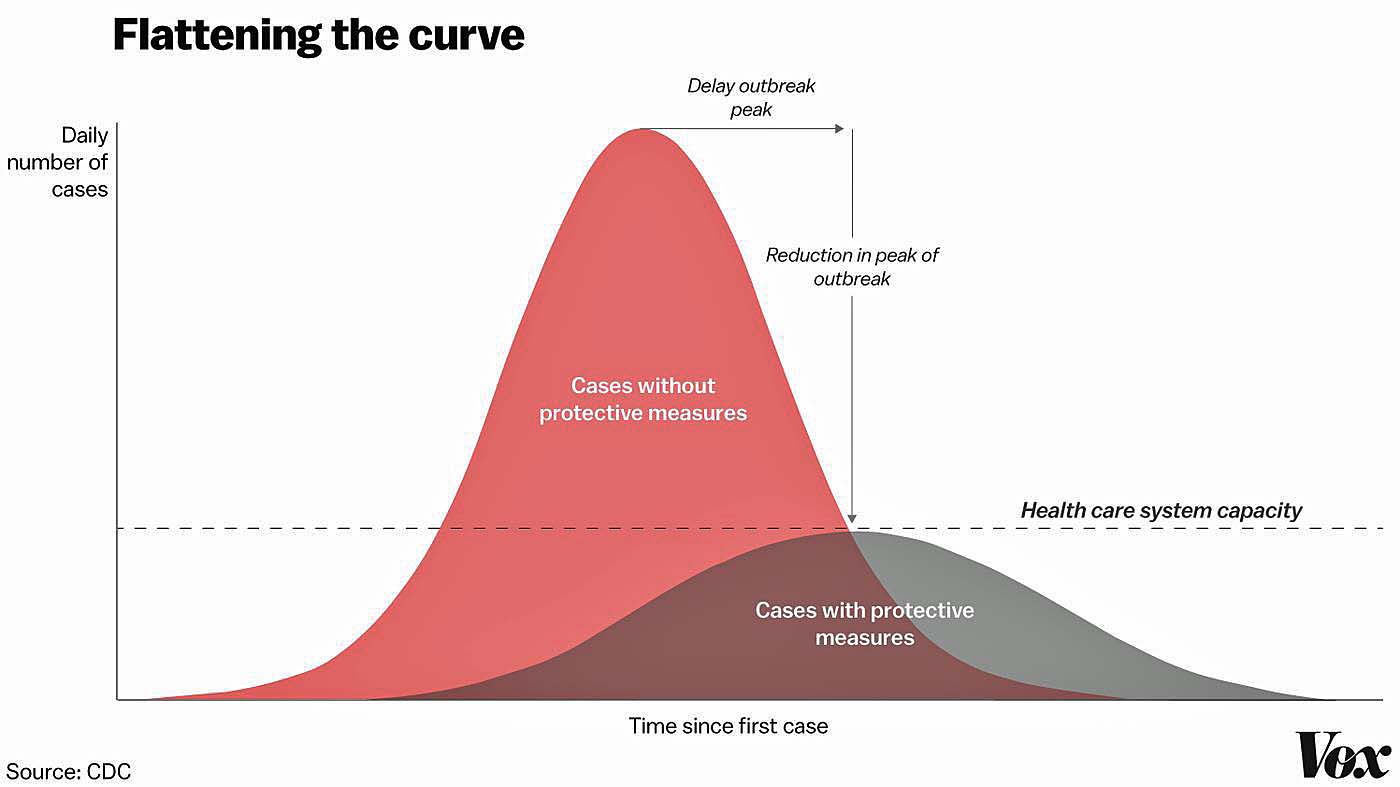
It comes from the
CDC. What is it attempting to tell us?
The obvious message is, use protection (social distancing, hand washing, etc.)
No one disagrees with that. But the graph itself is flawed and thus
serves as little more than propaganda for the unwary.
What are its flaws? Firstly, what are the axes? Time (horizontal) versus
number of infections (vertical). But what are the units? We are not told.
The time could be days or years; the graph is purposefully vague. This
makes it useless in telling us what to expect.
A deeper flaw is, with protection (the gray curve) we are supposed to see
that the pandemic lasts longer but infects fewer each day. Why would it last longer?
The implication is that the number of infections is somehow constant and,
if we protect ourselves, it is spread out over a longer period of time and
thus does not overwhelm our healthcare facilities, a worthy goal. But why
should the number of infections be a constant? Indeed, if fewer transmissions
occur, wouldn't that number be reduced? Isn't that the goal?
I conclude that this graph is -- though not intentionally -- misleading and
of little use. So stop copying and pasting it, folks!
top
|
| |

Corona
no
conference
March 6, 2020 --
Today, a conference I'd planned to attend
(LOINC at Regenstrief)
was canceled for fear of coronavirus propagation.
Is this a national -- worldwide! -- obsession?
Probably. Were the organizers wise to cancel?
Also, probably. The risk is tiny but if something
untoward had occurred, the consequences would have been
unacceptable. So I am disappointed but sympathetic.
Turns out medical conferences are being canceled everywhere:
Which Medical Conferences Are Being Canceled by Coronavirus?
We mustn't put our caregivers at risk.
top
|
| |

Cruel
bills
February 4, 2020 --
Medical bankruptcies are once again growing in America.
After brief respite under Obamacare, these
horrendous calamities are on the rise.
In Billing Quality Is Medical Quality, JAMA
today writes,
In a 2018 survey of 1513 patients with stage IV breast cancer,
50% reported that they had been contacted by debt collectors
regarding a medical bill, suggesting their medical bills were
significantly overdue.
Imagine this: you're dying of cancer and being dunned, garnished,
and sued, too.
Do we blame the hospitals and health care institutions for egregious
business practices? Not so fast. Some, says the article, are indeed
heartless and cutthroat:
At [some] institutions, some patients with private or no insurance
receive bills with prices that exceed Medicare allowable amounts,
and many patients who cannot pay may be subject to lawsuits to
garnish their wages.
However, it must be recognized that in our system, healthcare
is a business like any other and can't survive if it can't
collect payment. Indeed, many hospitals are themselves
struggling financially.
I place the blame elsewhere: on the duped public that does not
support reforms that would (and, briefly, did) end these cruel
practices, and on the cynical self-serving politicos who
promote them.
The current administration
is step by step dismantling the protections we all deserve.
If you vote for them, you'd better never get sick.
top
|
| |

Year
of the
nurse and midwife
January, 2020 --
The World Health Organization (WHO) has
declared 2020 the Year of the Nurse and the Midwife.

The world needs 9 million more nurses and midwives if it is to
achieve universal health coverage by 2030.
A lofty goal! But it's an important -- no, a lifesaving -- one.
Go nurses!
top
|
| |

Shopping
around
January 16, 2020 --
In Even With Hospital Price Lists, 'Shopping Around' Still Difficult,
Medscape observes that, "despite a federal mandate that hospitals publish price lists,
comparing prices among hospitals can be very confusing, and information remains limited".
It's a mess. You just can't figure out what your health care is going to cost you.
We have complained that this should be one of the functions of healthcare portals, and
their failure to provide this service is one of the reasons
portals suck.
Evidently we are not alone in this.
top
|
| |

Ber-
nie!
January, 2020 --
American nurses,
through our biggest union, National Nurses United (NNU), are
steadfast
in our endorsement of Bernie Sanders for the next President:
Bonnie Castillo, executive director of NNU, said, "Nurses are beyond
tired watching our patients suffer and die needlessly, simply due to
inability to pay, and we know Bernie Sanders is and has been leading
on Medicare for All through his advocacy and Senate legislation."
If you vote for anyone else, you better never get sick.
Go nurses! Go Bernie!
top
|
| |

The
checklist
is
ten
January 15, 2020 --
This year, we celebrate the tenth anniversary of the surgical checklist.
Pioneered by Dr. Pronovost and
by Dr. Gawande,
these checklists are, according to the New York Times in an article today
entitled
Where
Surgeons Don't Bother With Checklists,
"[in rich countries, the checklist is] used in 90 percent of surgeries...
studies showed the checklist reduced deaths by 24 percent and major
complications by 60 percent."
The article decries the relatively poor outcomes in poor countries in which
checklists are used less.
Even less-used in any country are nursing checklists. We have
contended for nearly a decade that the quality and outcomes of nursing care,
too, can and must be substantially improved through this simple technology.
Over ten thousand nurses have agreed with us and downloaded our app,
NurseMind.
It knows what we need to get done during our shifts and when each task is due.
It makes sure none are omitted and all are on time.
Another such app was recently released,
as announced on September 17, 2019 in Geneva, Switzerland --
UNITAR and partners launch new mobile application on WHO Surgical Safety Checklist.
But it's for surgeons, not nurses.
Are we nurses to remain the second-class citizens of health care technology?
Not according to Nurse Tech, Inc.!
We shall continue to advocate for the central role played by nurses in
every sphere of health care, and for the technology that supports us.
As we have said so many times before, go nurses!
top
|
| |

Portals
suck
December, 2019 --
In 2013, I blogged/griped about "patient portals".
In the years since then, they have gotten a little better... not a lot.
Why not? Because their design continues to be driven by financial not
quality-of-care motives.
It is not only me griping. See, for example,
Meaningful
Use of Health Information Is Meaningless For Patients (Chuck Dinerstein, 12/11/19, American
Council on Science and Health, "Promoting science and debunking junk since 1978"):
only 10% of patients use this access. Why so few?
Patient portals (of which Epic's MyChart is among the best),
serve the interests of the health care institution (HCI)
not of the patient. They do offer features that patients like,
such as:
- showing you your lab results which saves the HCI dealing with
paper and routing documents;
- making your appointments online which
saves the HCI man-hours, etc.
Yes, patients do like these
but they exist not for that reason but because they save money
for the institution.
There are plenty of other features that could be added to portals that patients would like.
But it doesn't matter what patients would like.
If a feature doesn't redound to the bottom line, it is not provided. Examples:
- I should be able to ask, what's this
procedure going to cost me out-of-pocket, in actual dollars?
- I should be able to view the video from my colonoscopy
(for example) online after the procedure is done.
- I should have access to the complete record of this (or any)
procedure including MD's notes, start and end time, and
the names of the providers involved and their roles. (This
information is in the EHR; it's just not available to patients.)
- I should be able to enter, review and correct data from out-of-network
sources, e.g. my childhood immunizations.
- I should be
given links to reputable web resources, not just to the
institution's rubber-stamp patient info brochures. But that
would be expensive to maintain and wouldn't
generate revenue so it's not provided.
We'll get these
things (if ever we do) only through legislation. Which
is today being weakened not strengthened. So I still contend
that portals suck.
top
|
| |

Nurses
assess
December, 2019 --
It is said that doctors diagnose and nurses assess.
Indeed they do -- time after time, all shift long --
even better with our new nursing assessment tool.
It's out! Following a two-year non-stop gestation,
the NurseAssess app
has been released.
This represents a major milestone for
Nurse Tech, Inc.
This is a "soft" release; the big one will happen in a
couple of months when integration with Epic is complete,
a feature requested by every reviewer.
Cerner and Meditech integration are not far behind.
Ready to give it a try?
Get it for your iOS/iPhone

Get it for your
Android phone 
And please let us know how it goes.
At feedback@nurseassess.com.
Was your experience with the app good?
Suggestions for improvements?
Here are answers to Frequently-Asked Questions (FAQ).
We are excited and proud!
top
|
| |

Another
behemoth
fails?
December2019 --
This review is two years late but still relevant.
Announced January 24, 2018, the
the Apple Health app (that
comes free with your iPhone) was given an
"...updated Health Records section [to bring]
together hospitals, clinics and the existing
Health app to make it easy for consumers to
see their available medical data from multiple
providers..."
The concept is good -- Apple
attempts what Google Health attempted (and
failed) -- to popularize a user-controlled repository for
1. locally- and 2. provider-generated health data.
Access to the platform (iPhone) gives them a big
advantage. They can collect things like sleep data
from other apps, number of steps walked from the
accelerometer, and so on. Google Health couldn't
do that.
The provider-generated part is a good idea but
doesn't yet work well. I was able to connect to
Labcorp and to Kaiser (where scraps of my medical
data reside) because evidently both of
them have invested the IT resources (not much but
not zero) to build the FHIR interface. The
list of providers that have done
this is long but I surmise
it's still a small minority of the providers
in the US. Google Health had the same problem
-- convincing third parties to make the investment.
Many didn't.
Perhaps it will take legislation --
the interoperability parts of ACA and HITECH,
perhaps? --
to make this happen. Alas, my primary
care provider, One Medical, has not done the
programming so their data about me remains
inaccessible. I have asked them to remedy
this... Stay tuned.
Does this demand fall within the mandate of the
Office of the National Coordinator for Health IT
(ONC) which is responsible for advancing
connectivity and interoperability of health
information technology (health IT)?
Section N (p.43) of Connecting Health and Care for the Nation, A Shared Nationwide Interoperability Roadmap calls for "Individuals [to]
Have Access to Longitudinal Electronic Health
Information, Can Contribute to that Information,
and Can Direct It to Any Electronic Location".
Might such locations include apps such
as Apple Health?

I think Apple is on the right track with this,
in the sense that it does something that I (but
not most others) find useful and interesting, and
it will fail for the same reason Google Health
did. That is, there is no compelling reason for
most health care consumers to take the time that
I took to enter demographics and to connect to
third parties. (Instructions)
It's only engaged, technophillic patients like me who
will do this. In other words, not a market
big enough for Apple.
top
|
| |

Rethinking
nutrition
December2019 --
The China Study, first published in 2005, is a bestseller and perhaps the most influential book about nutrition. It advocates a whole foods plant-based (WFPB) diet and the avoidance of animal-based foods for health and weight loss. This stance is based on the strongest dietary evidence to date: a 20-year research study with hundreds of thousands of subjects.
Disease rates in Chinese counties are correlated with diet (animal-based and not). The conclusions are indisputable. The authors, T. Colin Campbell and his son, Thomas M. Campbell II have rocked the world of nutritional science. Adherents (Bill Clinton among them) are legion and I, too, have joined their ranks.
Some side issues the Campbells raise:
- Modern science suffers from reductionism. In the case of nutritional science, the exclusive focus on micro-nutrients (e.g. are "carbs" good or bad? vitamins?) misses the point. They call it, "This mistake of characterizing whole foods by the health effects of specific nutrients... For example, the health effect of a hamburger cannot be simply attributed to... saturated fat... [that is] merely one ingredient. Even if you change the level of saturated fat, all of the other nutrients are still present and may have still have harmful effects on health." [p. 267] The way we study nutrition does not give us good guidance for how to eat.
- Studies by Western scientists have typically been based on groups that are too homogeneous to yield scientifically-valid results. There have been no control groups. For example, the Nurses Health Study (go nurses!), described by the Campbells as using the best experimental design (prospective cohort, i.e. following a group of people and recording diet information before disease events are diagnosed) is nonetheless fatally flawed, they say, by the homogeneity of the cohort -- all meat eaters. There is nothing to compare them to (no control group, i.e. plant eaters).
- Vegan and WFPB diets are not the same. "A vegan diet doesn't use foods of animal origin but can still include... processed foods, and is often high in fat, sugar, and salt, which compromise human health." [p. 240] Beware, fellow vegans!
- There is a political angle, too. The WFPB approach to health as opposed to traditional medicine's heroic procedures such as coronary bypasses and expensive medications "[threatens] the status quo by circumventing standard treatments... 'I'm making a freakin' fortune and you want to take it all away?'" [p. 324-325] Yes, we do want to take it away. For most chronic diseases (diet-caused), conventional medicine is a failure. The China Study demonstrates that there are better (and cheaper) ways to live, eat, and stay healthy.
We need, they say, to make a "...radical shift in [our] thinking about food." [p. 238] We must relearn a lifetime of habits -- shopping, cooking, eating, feeding our loved ones, and the culture that drives all this.
Read this book! Join the movement toward healthy eating!
Book cover image courtesy of Wikipedia fair use, link.
top
|
| |

RN,
healthineself
December, 2019 --
I am disheartened by the number of nurses who,
though competent, compassionate and even inspired on the job,
suffer from maladies and miseries from obesity and addiction
to depression and burnout. What is it about this job that takes
so much out of us? And what can we do about it?
One solution is work/life coaching.
I recently discovered (by chatting with her brother-in-law)
Abby Sanchez, an Oregon RN. She offers a podcast
(The
Thriving Nurse -- I'm an enthusiastic subscriber), a
web site (www.glowingnurse.com),
and coaching -- you can make appointments for phone calls that,
according to her testimonials, can be life-changing. I haven't
yet tried those, but I have seen so many nurses whose lives do
need change.
Nurses, heal thineselves!
top
|
| |

Still
volunteering
October 16, 2019 --
As I have dozens of times before (see earlier blog postings e.g. PHC 62),
today I worked a volunteer nursing shift
for Project Homeless Connect.

This was PHC's 75th such event -- quite a milestone! We continue to be proud of the good
work we do and horrified that it continues to be necessary. Indeed, San Francisco's
homeless population is growing.
Here are a few statistics about what was accomplished today:
- 1,100 participants were served.
- In Nursing, we saw 75 of these.
- I personally triaged 14.
And some stats (source: Applied Survey Research, 2019, SF Homeless Count and Survey) about SF's homeless population's self-reported health conditions:
- 42% alcohol and drug use
- 39% psychiatric/emotional conditions
- 37% post-traumatic stress disorder
- 31% chronic health problems
- 27% physical disability
- 15% traumatic brain injury
- HIV/AIDS related illness
As always, I am saddened by the severity of the afflictions I see (a bad
case of cellulitis, a bulging tumor, much drug addiction, HIV, scabies,
mouth abscesses, drug injection site infections, kidney failure,
psychoses, and much too much more) and heartened by the frequent cheerfulness
of the sufferers despite the adversity they confront. Peoples' resilience is amazing.
Governor Gavin Newsom is a big booster of this community service.
When it was first started around 15 years ago, his involvement was pivotal.
(Back then he was San Francisco's Mayor, one of the best we've had.)
Do-good volunteer organizations like PHC will continue to be necessary
as long as our country continues to be inhumane and exclusionary.
America's social safety net is inexcusably inadequate.
It's a sad state of affairs but we're doing what we can.
Join us at the next one!
top
|
| |

Vegan
works
September 20, 2019 --
An article in today's Medscape --
Vegan
Diet Alters Microbiome and Insulin Sensitivity, Drops Weight --
describes a study of vegan diet outcomes.
The diet called for low-fat, calorie-unrestricted, no-animal-products (vegan) eating.
The control group ate an everyday, non-vegan calorie-unrestricted diet.
The outcomes:
- Weight loss of a pound a week, on average
- Beneficial changes in the gut microbiome
- Increased insulin sensitivity (diabetes reduction/prevention)
The researchers write:
"Eating a plant-based diet with ample fiber changes the gut microbiome composition for
the better by feeding the right kind of bacteria... notably short-chain fatty acid
producing Faecalibacterium prausnitzii, [which] deliver many metabolic benefits
including weight loss, increased insulin sensitivity, and fat loss,
including visceral fat loss."
They caution (as they always do) that this evidence is not definitive and more study
is needed before specific dietary recommendations can be made.
But this is certainly support for
the diet choices I've made
(whole foods, plant based (WFPB))
and the outcomes I've observed in my own life (weight loss,
resolution of prediabetes).
Go vegans!
top
|
| |

Patient
engagement
September, 2019 --
"Patient engagement" is the buzzword du jour on
healthcare technologists' lips. I have even attended
conferences
of which this was the title. Yet, it's not happening.
It is disappointing that tools and resources
such as
Google Health
and
Microsoft Healthvault
didn't catch on with
the public. We consumers of health care products and services could not
be convinced to take charge of our health data and decisions. Why not?
In August 21, 2019 NEJM,
A Taxonomy to Engage Patients: Objectives, Design, and Patient
Activation
the writers (from Harvard's Kennedy School) suggest that
the poor quality of the tools constructed to date have prevented them from
engaging patients and consumers. "designs... are not user-centered...
and inattentive to users' needs." I have also blogged that
"patient portals" suck.
How can we fix this? The authors propose a three-part strategy:
- Give patients access to health information and data;
- Let patients produce and share their own health data; and
- Enable patients to connect with other patients, with their providers,
and with research groups.
On-line portals and communities do provide these
capabilities but no single provider or site offers them all
and none in a compelling way.
The authors survey on-line health resources
and describe how the successful ones succeed.
We need, the authors posit, to "[focus] on objectives and [understand]
patients' motivation to engage."
Notable successes are "peer-to-peer platforms
(e.g., MyHealth Teams and Breast Cancer Straight Talk Support
Facebook Community) [that] engage large numbers of patients...
[providing] information as well as emotional support."
They observe that "...moderation is key... conversations [must be]
carefully moderated to eliminate content that is inappropriate or not
backed by scientific evidence as well as to maintain respectful interactions."
Also essential is ease of access via popular platforms such as
Facebook with web and mobile (smartphone) apps.
What are the objectives of such sites and apps? The authors identify four:
- "Those that join patients... to health care providers;"
- "Those that connect patients to each other for support and peer advice;"
- "Those that make clinical information available to patients; and"
- "Those that [gather] data and ideas from patients... to advance research."
These are good objectives but can they be achieved? Will they engage patients?
For highly-motivated populations such as disease sufferers, this is
already happening. But what about the general public? When, will the majority
of consumers say, as
Dave DeBronkart famously said,
"Gimme my damn data!"?
Alas -- given what I've seen of a passive public too readily accepting
a paternalistic healthcare system and providers -- I remain skeptical.
top
|
| |

Linked
In
September, 2019 --
Social networking -- can't live with it, can't live without it.
Facebook, Twitter, Instagram, Pinterest, Tumblr, and more every day.
So what is the busy professional to do?
LinkedIn, of course! There, you're not bombarded by political screeds and worse.
It's where people look for jobs and recruits, so everyone is on their professional
best behavior.

It's also where projects and products are announced...
Ahem... Here is ours:
be a NurseAssess beta tester.
top
|
| |

Afib
July, 2019 --
A friend was recently diagnosed with atrial fibrillation.
Afib is serious but not usually fatal.
Here is what he needs to know,
in a paper I wrote for nursing school many years ago.
top
|
| |

Goodbye
Kaiser
June 19, 2019 --
Yesterday I had my final appointment in the Kaiser HMO
medical system. It was not serving my needs and, I argue, does not serve
the needs of many of its members. In our too-brief-as-always meeting,
my smart-but-doctrinaire MD Saruchi Tandon
acknowledged that Kaiser is "conservative and evidence-based."
She was half right. Kaiser is indeed conservative, in the sense that
the status quo is maintained, whether or not it means good care.
Medical decisions at Kaiser are decidedly not evidence-based.
Rather, they are made by habit and tradition.
For example, much could be done for sufferers of chronic conditions
-- notably hypertension and diabetes -- but Kaiser persists in simply
doling out pills (just like the rest of mainstream American healthcare) rather than curing.
The
evidence -- if only they would look at it -- shows that cures
are often possible.
I am living proof. Until a month ago, I had a diagnosis of
prediabetes. My fasting blood glucose was measured at 107 mg/dL,
exceeding the guideline of 99.
A medically-supervised fast
and lifestyle change to a
plant-based diet have brought my blood
glucose back down to a healthy level. (Today it is 84.)
However, in my decades
at Kaiser, I have never heard the words "plant-based" nor "fasting"
uttered.
Had I not taken matters into my own hands, Kaiser would have permitted
my diabetes to worsen to the point of no longer being "pre-" and
thus requiring a lifetime of Metformin and insulin and the
ugly sequelae of that awful disease.
Did Dr. Tandon ask me how I achieved my remarkable outcome?
Nope. Not interested. In our meeting, I attempted to describe it.
She changed the subject.
Another example, equally anecdotal but equally relevant to my life,
is my girlfriend, also a longtime Kaiser member. She has suffered
from hypertension for much of her adult life. Kaiser gives her a
handful of pills to take daily -- ACE inhibitors,
beta blockers, diuretics, etc. Kaiser was
guaranteeing that she would remain hypertensive for life.
They don't cure, they "manage".
Unbidden by Kaiser, she, too, has converted to a plant-based diet.
We are seeing her blood pressure numbers drop and she is weaning
herself off those pills. Like me, she has never heard anyone at
Kaiser utter the words "plant-based".
So I've decided -- after decades of Kaiser membership -- to ditch 'em.
My girlfriend still drinks the Kool-Aid and is not yet ready to
jump ship but soon she will see how much better medical care can be.
I am switching to
One Medical
where health care providers are not limited to
ten minutes, are not bound by tradition and habit,
and health care is not delivered by an assembly line.
Goodbye Kaiser! Hello health!
top
|
| |

HIMSS
hype
June 13, 2019 --
At the HIMSS Innovation Conference and Showcase in San Jose today,
one of the speakers was
Graham Grieve, called the father of FHIR (about which I
have written before).
Electronic Health Records are a young, immature technology. Often,
clinicians hate them; technology should reduce
workloads but has the opposite effect.
As the technology matures, this and other
problems will be solved. What will that solution look like?
It's been predicted that the EHRs will eventually be relegated to data stores.
They will evolve into backends that users won't experience directly. The parts that users will see
will be apps, GUIs, and fine-tuned solutions created by third parties such as
Nurse Tech.
What will it take to make this happen? At today's conference, we're told,
the answer is APIs. And the API of choice in healthcare is FHIR. Good
marketing, Mr. Grieve.
But not good talking. He emitted a stream of marketing
buzzwords and we're-smarter-than-everybody-else cheerleading.
Not much tech in the talk. This is what I'm
learning to expect at HIMSS events:
hype is the key to success. Thanks but no thanks.
top
|
| |

Not
interested
June, 2019 --
A few months ago, Microsoft announced that it would close its HealthVault service, effective
Nov. 20, 2019.
I have blogged about HealthVault before, e.g. here.
It will follow Google Health (blogged here)
down the ignominious path of project failure.
But why these failures? I had predicted that patients would want access to
(if not control of) their health data. Others had
made similar demands. Yet, consumers remained resoundingly uninterested.
A compelling case for us each to take charge (or at least acquire visibility)
could not be made. No business model emerged.
For me as a champion of empowered patients and the
information must be free movement,
this is a profound disappointment.
Hey, patients! Get with it!
top
|
| |

Numbers
June 5, 2019 --
Just a quick update on my progress here at
TrueNorth: my numbers.
Better than I could have hoped. And, after three weeks, I get to go home,
a week earlier than planned.
I love my flat belly! Weight down from 186 to 157 lbs. Woo hoo!
Fasting blood glucose (my primary objective achieved: no more
prediabetes!) from 107 mg/dL to 69 (above 99 is considered prediabetic.)
Systolic blood pressure down by 20 mm/Hg to 107 and diastolic
down by 15 to 73. Thrilled!
I was never on any meds for any of these conditions but most of
the others in attendance here were (and were sicker than I) and
all of them leave med-free and with numbers like mine.
This is no fad diet; it's the real deal.
A lifetime of change.
top
|
| |

Break
fast
May 31, 2019 --
If I haven't yet bored you with my incessant blogging about my TrueNorth fasting experience,
here's another one.
We get a couple of lectures every day, mostly on medical topics.
I've learned a lot and captured some of that here.
Today I broke my fast (as planned) after eighteen days of water only.
TrueNorth's protocol decrees a "refeeding" period of half the length of the fast so,
for me, that will last nine days.
They start us on light juices (breakfast: celery and raspberry -- yum!) and
gradually lead us to solid foods and a "normal" diet...
if you call SOS/vegan (vegan plus no salt, oil, or sugar) normal.
Which it shall be henceforth... my new normal!
How did it go? Evidently, my journey was easier than most people's.
Common symptoms are nausea, lightheadedness, headaches, and other miserable stuff.
I had none of those.
During the first week, I did endure some back pain -- I've occasionally had that
in daily life and fasting magnifies aches and pains temporarily.
By the second week, it was gone.
I've taken great joy in seeing
the number on the scale dwindle. I've lost thirty pounds!
I got my blood test results, too. I had been diagnosed with prediabetes.
The healthy blood glucose range is 65 to 99 mg/dL. Mine had been 106.
Today it's 69.
I feel great!
Want to overcome a chronic disease? Want to lose weight?
This regimen -- and TrueNorth -- is highly recommended.
top
|
| |

It
works!
May 25, 2019 --
It's Day 12 of my water-only fast here at TrueNorth in Santa Rosa, California, and it's
going so well that I have decided to extend it from the originally-planned 14 days to 18.
Despite the naysayers -- and they are legion -- this procedure (and the lifestyle changes
that follow) really work. I am already down more than 25 pounds, and I am certain that
my prediabetes is being vanquished. (These were my two goals.) I am thrilled.
And it's not just me. The woman in the room next
to mine came here to get off her blood pressure medications -- she had been taking
seven, including two diuretics -- and after only a week, she has achieved that.
She is now normotensive, and she feels great. She fully expects
never to take those pills again.
Her story is not unusual; indeed it's business as usual here.
The conversation we all have -- almost daily --
is, why is this not mainstream medical practice? The body's ability to heal itself
so vastly outstrips what conventional medicine can achieve with pills and procedures,
it's perhaps literally criminal that "modern" healthcare refuses to consider this modality.
They offer a couple of lectures every day, and I've been
learning a lot.
Think about it... Read the evidence... Don't drink the kool-aid... Drink water!
top
|
| |

Get
well
May 21, 2019 --
Today I finished reading The Pleasure Trap (2003)
by Doug Lisle and Alan Goldhamer, the "bible" of this place
-- TrueNorth Health Center -- where I am undergoing a
medically-supervised water-only fast with the intention
(which I'm certain will be fully realized) of overcoming
my pre-diabetes and losing 30 lbs.
This book describes the philosophy that underlies what is done here.
More than that, it offers a prescription for what ails
so many Americans and eaters of the "western" diet worldwide.
Here's the idea: Our bodies evolved for food that's
different from what we eat today.
We can process it but not well.
So we are often sick and fat.
The solution is to eat the right food (SOS/vegan).
And the process of healing can be jump-started
by water-only fasting.
The body has remarkable abilities to heal itself
-- far better than any medical care -- if only we let it.
Applying this strategy has achieved astonishing
-- almost unbelievable -- results.
Yet, they are true and well-documented.
So what is the "pleasure trap"?
The book's subtitle is,
"Mastering the Hidden Force that Undermines Health & Happiness."
That force is human motivational mechanisms that drive
us to seek food that, evolutionarily speaking,
was rare and precious: calorie-dense foods.
These foods are now abundant and we
eat them in great quantities.
Our bodies are equipped only for small amounts;
mostly, we are geared for low-calorie-dense
vegetables and fruits, not oils (a modern invention),
meat and fish (infrequent in prehistoric diets),
refined grains (another modern invention),
added salt and sugar (absent in food until recently),
and the like.
Thus, our instincts no longer drive us
to do what's best for us.
The book teaches us about this trap and how to avoid it.
Once we get the message, many chronic diseases --
increasingly endemic in modern life -- will be overcome.
The forces arrayed against this potential revolution
in health recovery are numerous and powerful.
It challenges the dogma in our culture that protein
from meat has the highest quality, essential for
nutrition; and that calcium for strong bones
comes from milk and dairy.
It threatens the makers of the food that makes us sick:
meat and dairy industries, food processors
(most processed foods are too calorie-dense
and laden with fat and salt).
Also threatened is the medical establishment
protecting its hegemony and coming from a mindset
that cures can result only from "doing something"
-- a pill or a procedure.
Fasting, by contrast, is essentially doing nothing;
get out of the way, let some time pass,
and watch what happens.
The results are nearly miraculous and should be standard practice.
Take heed, America! Take heed, world! You have only your health to regain!
top
|
| |

Allopaths
'rus
May, 2019 --
Practitioners of alternative medicine like to refer to
their conventional counterparts (MDs) as practitioners
of allopathic medicine. I've never seen this word used
in another context and believe it smacks of disdain.
There is also disdain for those who use this word.
Dr. Kimball Atwood IV writes in Medscape General Medicine
Naturopathy,
Pseudoscience, and Medicine: Myths and Fallacies vs Truth (2004):
There is no such thing as "allopathic" medicine,
a pejorative term coined by the founder of homeopathy, Samuel Hahnemann.
Those who use it to describe modern medicine only betray their ignorance.
[emphasis mine]
...Hahnemann meant by "allopathic medicine" -- the prescientific,
highly toxic practices of bloodletting, purging, scalding, etc.,
based on the "four humours".
So the naturopaths and osteopaths look down their noses
at the people they call allopaths. The MDs ("allopaths")
give little credence to the so-called sciences of
naturopathy, homeopathy, and other "complementary
and alternative medicines" (CAMs). Each defends their
turf.
I guess it's clear which side I'm on.
Practice must be substantiated by evidence.
In other words, science. Call that allopathy if
you like... It's just a word, a word that reveals
your bias, a bias I don't share.
top
|
| |

Goingfast
May 16, 2019 --
"How long are you in for?"
The question is like the one inmates ask each other.
Here at
True
North Health (TNH), though, it means, how long is your fast?
Mine is 14 days, followed by 7 days of "refeeding".
During the fast, I get only water. Refeeding (I wish
they'd come up with a better name) starts gently
with light fruit juices for a couple of days,
then stronger ones, then a little light solid food, and so on.
True North is a comfortable place.
The rooms are well-appointed.
Everyone is friendly. There are classes (yoga,
stretching, mind/body, meditation) and lectures (mostly medical
topics). Between these things, there is lots of free time.
I brought my laptop and plenty of work so I am keeping busy.
I am treating this as a working vacation.
It's a vacation with some benefits: health, weight
loss, education, and lifestyle change.
I am also participating in a research study. I am one of a few
dozen subjects selected per strict criteria. Blood test data is
collected, as well as body measurements. The exact goal of
inquiry is unknown to me, as it should be. It's a double-blind,
controlled, randomized clinical trial.
Of course, not eating for 14 days (or whatever duration you choose;
the upper limit is 40 days) is not easy. I am in my fourth day now
and so far have experienced no ill effects except hunger, that is
surprisingly mild and fleeting. I love getting on the scale each
morning and seeing another pound or two gone!
Our fasts are medically supervised. Blood is drawn and analyzed.
Urinalyses, too, are done. Twice a day our vital signs are checked
(pulse, blood pressure, temperature) and a physician checks on us
and reviews our progress. The process is remarkably pleasant.
And it has real science supporting it (more about that in a
future blog.)
Why fast? The health benefits are numerous and well-documented.
Some, like me, come here for a tune-up and weight loss. I was
recently diagnosed with prediabetes -- at 106 mg/dL I am just
over the recommended maximum of 100 -- as is half the adult
population of America. But just because it's normal doesn't
mean it's good. As a nurse, I have seen what diabetes does
and I intend to go nowhere near it!
Some come here with more serious diagnoses. One of the
most dire is lymphoma (cancer of the blood) and TNH has
actually resolved this. Another is multiple
sclerosis (MS). Along with rheumatoid arthritis and
many more auto-immune diseases, MS can be cured by
fasting and diet change. So can hypertension,
hyperlipidemia, and many more. People come to TNH for
all kinds of reasons. In its 35 years of operation,
20,000 people have fasted here. All have benefited
hugely. There has not been a single death. It's a
remarkable track record.
As a medical professional, I know that we're not supposed
to say something is cured; we must say (especially
regarding chronic diseases) that it's managed.
But that's the problem:
allopathic medicine (as these
alternative medicine folks like to call it) doesn't
cure. Well, that's not true; it has has had
tremendous successes with bacterial diseases,
genetics, immunization, surgery,
orthopedics, and many more. But still...
Given TNH's record of accomplishment, one can only wonder,
why is this not mainstream? Theories abound.
Their essence appears to be resistance
to change (by the medical establishment) and threats
to sales (by the pharmaceutical,
meat, dairy, and refined grains industries).
Indeed, one of my best buddies, an MD, became
enraged when I extolled the health benefits of fasting
and the vegan/SOS (no salt/oil/sugar)
diet. There's no science behind it, he said.
(There is; numerous studies support this.)
The people who sell this are quacks, he said.
(They're not; they have done substantial research
and publishing in peer-reviewed journals.)
And the best evidence: the thousands of folks who have
gotten off their meds and had their quality of
life -- if not their life itself -- restored
are proof to the contrary.
Fat and sick? This is the place for you.
top
|
| |

Freeradical
May 13, 2019 --
I am undergoing a two-week, medically-supervised,
water-only
fast
(about which I will blog soon) at True North Health Foundation's
residential treatment facility in Santa Rosa, California.
True North's founder is the remarkable Alan Goldhamer, DC.
I have attended his lectures, read one of his books,
watched his videos, and chatted with him over an SOS-vegan
dinner.
The work he does is radical and has hugely impacted
the lives of the 20,000 people who, like me, have
fasted at True North to
maximize and regain our health.
His institution runs smoothly, is remarkably affordable,
and achieves health results that are nothing short of miraculous.
Until you study the science...
Then it's obvious and inevitable.
About that, I'll blog later.
Goldhamer confronts (and often antagonizes) the
medical establishment and food industries,
both of whom are contributing to (or at
best not curing) growing
nation- and world-wide epidemics of
diabetes, hypertension, and
auto-immune diseases such as multiple sclerosis
and rheumatoid arthritis.
It is a battle that will be won
-- people want health! -- but the struggle is uphill
and we have a long way to go.
He has been waging this war for forty years.
During this journey -- which demands repeated
explaining and convincing -- he has come to repeat
certain phrases so often that he now utters them in a
hasty blur of syllables, almost as if they were a single word:
- Of typical Western food, he says,
"We must stop eating that greasy-fatty-slimy-diet
of dead-decaying-flesh."
- The rare physicians who,
instead of prescribing lifetimes of pills that "manage" not cure,
dare to promote fasting interventions and lifestyle changes
that actually help patients get well, he calls,
"Doctors who want to do something worthwhile
with their lives: heal their patients."
Goldhamer does not mince words.
top
|
| |

Nurse
informaticians'r us!
April 13, 2019 --
Today is the last day of yet another superb conference
(the 19th) of the
American
Nursing Informatics Association (ANIA).
I always learn so much and meet people who inspire!
The photo is a selfie with a
nurse hero, Diane Humbrecht DNP RN-BC, past president of ANIA
and now CNIO (wow!) at Virginia Mason Medical Center (double wow!)
in Buckley, Washington. Diane has done much to advance the
field of nursing informatics both professionally and academically.
One of those inspiring ones!
There is much to blog about. F'rinstance:
- Lots of work on alarm fatigue.
- Big data! Lots of talk... but who really "gets" it?
- Real-time, point-of-care documentation... Hey, this is
what I'm building with NurseAssess!
- How do we pave the way for the next generation of nurse informaticians?
Is it just me or do I observe that most of us at this conference
are in our 60s? Where is the fresh, new energy?
- Patient engagement... We know that involving patients
in their own care yields better outcomes. But why is it so
hard to do? Why don't they use the so-called portals the
provider organizations build and tout? Because portals suck!
But that's a topic for another screed... er, blog...
Stay tuned!
And join us at ANIA #20 next year in Chicago!
top
|
| |

EHR
reportcard
March 18, 2019 --
In this excellent article,
Death by 1,000 clicks: where the electronic health
records went wrong, Fred Schulte and Erika Fry of Fortune magazine
and Kaiser Health News (an editorially independent program of the Kaiser
Health Foundation) give us a thorough look at the status of EHRs today,
especially in light of the strong financial push they got from
Obama's stimulus package.
Most hospitals and many doctor's offices have them now.
How's it going? Were they a good idea?
Well, yes and no.
There is much we could have done better.
For example, George W. Bush's healthcare tech czar
David Brailer said,
"HITECH should have spent its $30 billion
on standards, interoperability, a "Geek Squad" to help
with training and implementation,
and creating a cloud-based 'medical Internet'."
He's right. We were naive. 20/20 hindsight!
Here are some of the main issues discussed in the article.
In some cases, EHRs have actually caused patient harm.
Software glitches, user errors, and system flaws have
caused orders to be lost, erroneous diagnoses and
prescriptions, and many more.
Deaths, serious injuries, and near misses have resulted.
EHRs facilitate "upcoding", the practice of overcharging
by changing billing codes to more expensive ones.
This is, of course, fraud. Settling such allegations
has costed vendors more than $200 million.
Interoperability -- the ability to exchange data among
EHRs so patient records could be shared with doctors and hospitals
anywhere in the country -- is a promise that remains largely unmet.
Doctors (and nurses!) are burning out. Now they must
spend so much of their time clicking menus and typing --
up to half of their working hours, by some estimates --
that the frustration from not instead spending this time with
patients has caused many to quit. This is termed by some
to be a healthcare crisis.
The EHR vendors routinely contractually obligate their
customers to withhold information about
product and system failures. These "gag clauses"
hinder public scrutiny of safety issues
and failed software installations.
My opinion: EHRs are harder to do than we thought, and our
early efforts are more painful than we expected. It's a
new technology, still in its infancy. It will be decades
before it's seamless. But let's not give up!
top
|
| |

Paying
forMedicare for All
March, 2019 --
Medicare for All (M4A) -- great idea, right? But how do we pay for it?
Here is an Economic
Analysis of Medicare for All by an authoritative group including
Don Berwick, former head of CMS.
It has plenty of opponents.
At the heart of every right-wing position is opposition to taxes.
That's why they hated the ACA; it had new taxes for the wealthy
(though they pretended to have other reasons; the greed
exposed by the truth would have been too obvious). They
hate M4A because it includes a net worth tax. That will hit
rich people hardest. It also proposes to abolish capital gains
taxes, taxing them as ordinary income. It's the right
thing to do. But they'll fight it as they always have.
One thing I would change is continuing to tie health coverage
to employment. I think people should buy their own healthcare
(even if that means paying into M4A) instead of getting it from
their jobs. What employers spend on healthcare should instead
go into paychecks. I also oppose funding M4A with a sales tax;
such taxes are regressive.
Read it yourself. See whether you agree.
top
|
| |

Bad
behaviorpoints
February 20, 2019 --
Should we forgive the Virginia Governor's youthful bad behavior?
The answer is spelled out in
this article in Medscape by Dr. Arthur Caplan.
It boils down to, "No!"
It's especially serious given the special faith placed in medical people,
says Caplan. (Governor Northam is also a pediatrician and neurosurgeon.)
I am troubled by the inflexibility of this zero-tolerance approach.
I remain convinced that Al Franken's treatment was too harsh.
So I propose a more nuanced method for dealing with bad behavior by public figures.
It's a point system. Get 20 points and you're out.
Rape is 30 points. Off-color jokes (in settings other than bars and such)
get 5 points. Overt racism, 10. Unwanted touching, 8.
Your points are diminished by 1 for every 3 years that have
elapsed since the act in question.
We could debate what the right numbers are, and the list of
transgressive acts, but the concept seems useful.
Could we get it added to the code of conduct of the US Congress?
The political parties?
top
|
| |

No vax?
Die!
February 5, 2019 --
"Measles: Will It Take a Death to Get Kids Vaccinated?" Dr. Paul Offit asks in this article.
He writes, "Invariably it's children who suffer our ignorance, and it is unconscionable."
Nurse hero Terri Olson writes:
This is a perfect example of what happens
when people fail to listen to FACTS.
You cannot make health decisions by listening to anecdotes on the internet.
This happens primarily in the more affluent communities where parents spend more time on the internet
and think they have more leverage to make decisions they are not equipped to make about their children's health.
My experience was that most of the immigrant moms raced their kids into the clinic to have them properly
vaccinated and viewed it as almost a luxury.
Sadly, with the loss of regard for FACTS, we will have more issues such as this.
top
|
| |

Still
turkeys
December 29, 2018 --
In an earlier blog the joke was that folks opposing
the ACA were like British turkeys voting for Christmas.
(In the UK, the traditional Christmas dinner is turkey.)
They're still turkeys! In an op-ed
(Everyone Gets Sick)
in today's NYT, California Senator Kamala Harris (whom I hope to help elect president in 2020)
lists the folks who will suffer as a result of a partisan Texas judge striking down Obama's landmark legislation:
- People with "pre-existing conditions" could once again be denied coverage.
- Insurance companies would once again be allowed to discriminate based on age and gender.
- People in their mid-20s would get kicked off their parents' plans.
- Lifetime coverage caps could come back.
- Out-of-pocket costs would no longer be capped.
- The expansion of Medicaid in dozens of states could be reversed.
- More than 50 million Americans could be rejected for coverage by health insurers.
- 20,000 to 100,000 people could die each year due to decreased healthcare coverage.
Surely an awful lot of these folks vote Republican. When will the turkeys stop voting for Christmas?
top
|
| |

Nursing
orders
October, 2018 --
Doctors order things all the time -- diagnostics, medications, treatments -- and so do nurses,
within their scope of practice, of course. But we don't call them nurses' orders,
observes nationally recognized Electronic Health Records expert and industry thought leader Ann Farrell, BSN.
Instead, we call them care plans.
This is a problem. For one thing, hospitals cannot charge for them, weakening
nursing's political and organizational influence.
Also, nursing care plans are not tracked well -- though nursing care is essential to
value based pricing (VBP) which ties revenue and penalties to outcomes.
And of course outcomes are dependent on, more than anything else, nursing care.
Ms. Farrell writes [personal communication]:
Do we REALLY know which are key OBSERVATIONS (we forget this when replacing RNs with
lesser educated and experienced staff) and interventions RNS do that impacts outcomes?
Hospitals want the cheapest staff possible which makes nursing vulnerable.
A set of MD's orders is an "order set", and a set of RN (and therapist) orders is a
"care plan". Together, they provide an "integrated plan of care" which brings together
the entire care team, and should increase stature of nursing role.
Alas, nurses are considered "task masters" -- following MD orders.
People don't understand the role nursing has in CREATING part of the plan of care.
People think of RNs "passing meds" as if there were not a critical thinking process.
The MD order may be perfect when it's written but patient status changes from moment to moment.
EVERY TIME an RN administers a med they evaluate its appropriateness.
People think it's just an assembly line from drug cart to patient, RN role "transport".
NO ONE has been able to explain what nurses DO!
[We also] lack a common "framework" or terminology to guide profession and industry...
it's painful to reflect on the damage to nursing due to lack of data (and leadership)
to support what value [we] bring.
The words we use to describe nursing's contribution denigrate it.
By continuing to undervalue the role of nursing, we deliver health care that's not as good
as it could be.
What's needed, says Farrell, is deeper thinking by our nurse leaders
and less simplification of complex issues.
Nurses must participate more fully in technology design and deployment decisions.
We nurses have largely abdicated those responsibilities. For our jobs and our patients, this must change.
In a time of tremendous economic pressures and disruptive technologies, Farrell's is a rare voice of reason.
top
|
| |

Sugar
=
poison
Aug. 21, 2018 --
We've known for decades that sweets are bad for us.
The evidence continues to mount and today Medscape has published
The Case Against Sugar:
It took more than 40 years from the publication of studies that pointed to the dangers
of smoking cigarettes to begin to rein in the tobacco industry and reduce cigarette smoking among the public.
Now, we are seeing similarities with the sugar industry, which is wreaking havoc on
public health by influencing both science and public opinion.
Here is what we must do:
- Educate the public.
- Ban sugar promotion at sporting events.
- Ban sugar product promotion in grocery stores.
- Tax sugar-sweetened products.
- Ban sugar product advertising.
- End food subsidies.
- Ensure that dietary advice is independent of bias.
- Separate diet and exercise goals.
It will take time, but the payoff will be better health for Americans.
top
|
| |

Another
nurse
hero
June, 2018 --
I first met Suzanne Bakken when she was on the faculty at my alma mater UCSF,
perhaps fifteen years ago. She taught the only informatics course in the School of Nursing,
and there hasn't been another one since she left. As
I have blogged before, this is a grievous omission.
A few years ago, I reached out to the Dean (who shall remain nameless) and
proposed a modest informatics curriculum. No interest. Su, we need you back!
But we surely won't get her back, and for good reason.
She went to Columbia in New York City where she is now a full professor and
publishing mightily as always. I applied to Columbia (MSN program) a decade ago,
was accepted, and almost followed her there... but I decided not to abandon
my family in the Bay Area.
Meanwhile, Su has been super-productive, most recently becoming Editor-in-Chief
of JAMIA, AMIA�s flagship informatics journal (read
the press release).
It's great to see nurses breaking through that glass ceiling. Go Su!
top
|
| |

EHR
market
shares
June, 2018 --
I have blogged about Epic
before -- the 800-pound gorilla in the EHR marketplace -- but there
are a couple of others -- Cerner and Meditech -- snapping at its heels.
top
|
| |

Reboot
education
June 2, 2018 --
Attending my alma mater UCSF's annual Alumni Weekend today,
I heard a fascinating talk by the acclaimed Dr. Eric Topol,
named the most influential physician executive in the United States.
In his wide-ranging talk, Dr. Topol touted some amazing new devices
available (or soon to be available) to consumers including a
continuous blood pressure monitoring wristwatch, a non-invasive
blood glucose monitor, an EKG watch with more accurate readings
than most cardiologists, and so on.
The technology of health care is changing fast, he told us, and
the role of the clinician is changing from that of data gatherer
to that of data interpreter. Thanks to artificial intelligence,
it will soon be more important for doctors to be good communicators
than "brainiacs" (expert diagnosticians).
How do we get there? "Reboot education," he says. Among other
radical changes, this means teaching more about technology.
My own nursing school experience -- not so long ago -- confirms this.
We had not a single lecture on, for example, the topic of the
electronic health record (EHR) let alone an entire class...
Despite the fact that nurses quite literally spend more time in
front of the computer than in front of the patient.
Reboot education indeed!
top
|
| |

Gun
research
April 10, 2018 --
Gun violence is a public health issue.
It should be studied.
Perhaps research can suggest solutions.
The Dickey Amendment prevents the federal government from doing this...
scoring a bullseye for the gun lobby.
Why suppress research? The reason is obvious:
the gun industry knows it would reveal what they don't want revealed.
But today Kaiser has stepped in, with
an ambitious plan to research gun violence (Washington Post).
Thousands of Kaiser patients must be treated each year for gunshot wounds.
"We should be thinking about this problem and studying interventions
for it in the same way we study heart disease or diabetes
or any other leading cause of death."
Go Kaiser!
top
|
| |

Epic
Mecca
December 28, 2017 --
Today I went to Mecca. (Click
image
for full size.)
Well, not exactly Mecca, but certainly the center of
universe of EHRs (electronic health records) -- the opulent
corporate headquarters of
Epic
in Verona, Wisconsin. (I have
blogged about Epic before.)
It is by far the leading vendor of these systems,
with the largest market share and growing.
The EHR (formerly EMR, electronic medical record) is a passion of mine.
I built one back in 1980-1983 as my Master's thesis when I was in graduate
school at UCSF. It was a real one and was even briefly in live service in
UCSF's outpatient dermatology clinic. (I had this access because my thesis
advisor, the reverently-remembered
Dr. Marsden Scott Blois,
was a practicing physician in that clinic... And HIPAA did not yet exist.)
Its name was Encounter Data System (EDS)
because its function was to capture and report information about patient
encounters: demographics, diagnoses, procedures performed. It was written
in C, ran on a Digital Equipment Corp. VAX computer running Berkeley
Software Distribution (BSD) Unix,
with a UC Berkeley-developed database named Ingres (that
"spoke" not SQL but Quel, a predecessor) as its backend (data storage and retrieval).
It really worked.
I suppose I could have made a career of it; Judith Faulkner (the sole owner of
privately-held Epic and now one of the richest women in the world) certainly did.
Alas, being too early is just as fatal as being too late.
I mean no sour grapes to Ms. Faulkner nor to her company; their product is in
many ways brilliant and their success is well-earned. And -- as I saw today --
the offices that success can build are spectacular indeed.
Click the thumbnail image to see it full size: yours
truly at the head of an Epic Boardroom table.
top
|
| |

Not
Documented
Not
Done
January, 2018 --
"If it wasn't documented, it wasn't done."
We nurses have had this drummed into us.
Seems logical, right?
Our coworkers need to know what care has been delivered
(or not delivered) and the lawyers do, too. Or do they?
It's counterproductive!
We waste so much time in front of the computer.
For example, why document hand-washing?
There are only three reasons to document in healthcare, and CYA isn't one of them. The three reasons are:
- It is meaningful for patient care.
- It is necessary for regulatory requirements.
- It is needed for billing.
As EHRs mature and begin to support -- not impede -- nursing workflow,
dogmas such as this one are at last being abandoned.
Cartoon by
Charles Keller (Dan's Dad)
top
|
| |

Healthcare
Econ
101
January, 2018 --
It is well understood that our health care system is expensive and dysfunctional.
We pay too much and, in terms of outcomes, get too little, especially by comparison to other countries.
Why? Here are a few of the basic economic principles at work in our health care system.
Principle #1: Follow the money.
Financial rewards are the primary motivator -- indeed the raison d'être -- of every business,
and in the United States health care is a business.
But here is the problem, as stated in the Journal of the American Medical Association (JAMA) in 2003:
"The United States alone [among wealthy countries] treats health care as a commodity to be distributed
according to the ability to pay rather than a social service to be distributed according to medical need."
Principle #2: Regulate.
I am as much a capitalist as the next guy and am clear that business is what makes our high standard of living,
but it must be regulated. Well regulated.
Such regulation must enforce basic human rights including the right to health care.
Leaving people without health care, medical bankruptcies, exclusion for
pre-existing conditions and so on, are travesties
and should not be permitted.
Principle #3: Payment models matter.
In an ideal system, providers are rewarded for outcomes.
There are some incentives for this in the Affordable Care Act (ACA)
and in Medicare including patient satisfaction surveys that have been made
a factor in hospital reimbursement by government.
However, the predominant models are driven neither by outcomes nor by quality.
Principle #4: What is rewarded increases.
-
A traditional model is fee-for-service. The result is, of course, more service.
(This was discussed in my blog post Doctors as Businessmen.)
-
Another common model is capitation -- a provider network is reimbursed a fixed amount for each patient.
So the result is more patients. In capitation models, the scramble is for market share.
In any model, the physician says, when the patient is in front of me, he is the most important person.
After he leaves, the most important person is the payer.
The intersection of healthcare and economics, alas, will always be an uneasy one.
Cartoon by
Charles Keller (Dan's Dad)
top
|
| |

Nursing
the
system
November, 2017 --
There is a new role for nurses: the Clinical Nurse Leader (CNL). Well, relatively new; certification for this job role began only ten years ago.
It comes with some new vocabulary. For example, a microsystem is a hospital unit.
Here are a couple of fascinating Medscape articles by Linda Borns:
The Clinical Nurse Leader Role,
and
A Day in the Life of a Clinical Nurse Leader.
Ms Borns' microsystem is a 24-bed medical telemetry/oncology unit.
Her work there demonstrably improves outcomes and reduces costs.
Wikipedia defines the CNL
as a healthcare systems specialist.
The idea of applying systems approaches to healthcare delivery is a good one, and timely.
top
|
| |

Choke
it
down
June, 2017 --
Call something a conspiracy theory and you stack the deck.
But with Big Pharma, the conspiracy is real.
To nurses, the evidence is stark.
We see that our primary function often
is merely the administration of "meds".
This is how we manage chronic diseases,
which for many of us comprise the bulk of our patients' conditions.
Very little of our work is prevention.
Rather, we dole out pills and drive a trillion-dollar industry.
It is also driven by a powerful lobby. Notably, Big Pharma wooed
the Bush administration who gave us Medicare Part D that both bolstered
pharmaceutical sales with tax dollars and outlawed discounting to the federal government,
Big Pharma's biggest customer. This made a gaggle of these
lobbyists rich
and a profitable industry more profitable than ever.
My opinion of Trump is low but I do agree with his statement that
drug
prices must come down. Let's see whether he delivers.
Let's take things a step further and redesign our healthcare system
to be more than a drug-selling machine.
We nurses need to be more than pill-dispensing servants.
Hey nurses, remember
that oath we swore the day we got pinned?
Our work is to benefit our patients, not to enrich an industry.
top
|
| |

Kaiser
Ed
May 2, 2017 --
I am a Kaiser patient (a "member").
Recently diagnosed with pre-diabetes, I signed up for a class on this topic.
Presumably, Kaiser's goal in offering such classes is lifestyle modification.
The benefits would be enormous, both for Kaiser's bottom line and,
even more importantly, for the health and quality of life of its patients --
people like me.
Yesterday, I attended the class.
What I learned is that health education at Kaiser is merely a formality,
and is unlikely to achieve any positive outcomes.
This is clearly a missed opportunity.
In this essay, I propose some remedial actions that could be taken at Kaiser,
and suggest that the payoff -- both to the organization and to its patient members -- would be immense.
Cartoon by
Charles Keller (Dan's Dad)
top
|
| |

Never
events
April, 2017 --
What's a "never event"? It's one that should never happen, a failure by a caregiver or organization, technically termed a serious reportable event.
The National Quality Forum calls itself "...a not-for-profit, nonpartisan, membership-based organization that works to catalyze improvements in healthcare"
and it identifies 29 never events.
Of particular interest to med-surg nurses -- considered important measures of quality (or lack thereof) -- are falls (4E in the above-linked document) and bedsores (4F).
Fascinating reading!
top
|
| |

Reconciling
April 10, 2017 --
Reconciling the meds (that is, answering the question, what is the patient taking?) is one of the maddening, time-consuming, excessively-repeated tasks nurses must do and rarely get right. My friend Claire writes:
I have been an inpatient in 4 institutions in the last 6 months, and the quality of care varies wildly.
I take several meds in the morning and several in the evening. I take pain meds PRN 3-4 times per day. But I also have two glaucoma drops, a shot for bone density, and inhaler, and a few OTC meds, and they started me on vitamins and iron because I was anemic.
I always bring my own meds because I know that they will not have them all for at least 3 days. I surrender my meds to the pharmacy and then they dole them out to me. In hospitals it's a giant pain in the ass to dispense even an aspirin. The problem there was always just getting the meds at all. At the rehab place, where I was an inpatient a much longer time, I had to insist that they put each med in a separate cup, labeled. They still left out half the meds and/or gave me the wrong dose most of the time. I was able to insist that they do it right even if it took 3 trips back and forth.
Now just imagine I was one of the typical elderly patients there. If they are members of our parents' generation, they ask no questions, and many people don't know what meds they take or what they are for. It won't happen to me because I am on the ball. But most inpatients aren't! They trust that they will be given the right meds at the right time, the right dose. My experience was that only by the third week did they finally deliver the right thing. It took two weeks of doing it wrong before they learned. I was also there for 5 weeks in Oct/Nov, and in order to get cooperation on giving me the right drugs, I had to email upper management.
Shame on us!
top
|
| |

High
reliability
April, 2017 --
Another fascinating talk at ANIA 2017 was Amy Edmondson, �Managing the Risk of Learning: Psychological Safety in Work Teams�. She, too, offered an interesting metaphor: when you get on a plane, you don�t do it saying, �This will be a good flight because Jane Smith is at the controls.� Yet, we do that in health care. Unlike when we fly, we don�t assume that the care team is thoroughly trained and expert in delivering the best-researched and best-engineered standard of care.
Aviation has known for decades that it is a team � not a heroic individual � that makes it safe. In healthcare, by contrast, we often say things like, �I had the world�s expert in [disease X � my disease] treating me.� The implication is that another provider would have delivered inferior care, and that there are not standards for consistently delivering best practices.
This is changing. We are starting to talk about making health care organizations be HROs: High Reliability Organizations. One standards body addressing this is the Joint Commission on the Accreditation of Healthcare Organizations (JCAHO) that is working on, among other things, the five components of safety culture (see p.477).
One such component is psychological safety: no penalties for errors nor for asking for help nor for providing feedback. These are essential for an O to be an HRO. It is more emotionally satisfying to praise (or blame) people than systems. This is one of many habits we in healthcare must overcome.
top
|
| |

Comms
metaphor
April, 2017 --
At last week�s ANIA 2017 conference in New Orleans, one of many fascinating presentations I attended was �Scalable Communication Strategy� by Rhonda Collins, CNO of Vocera and a colleague of my friend Kathy English (VP of Global Marketing).
Ms. Collins offered an interesting metaphor for the structure of communications systems: the mobile device is UPS or the postal service; it just delivers. The EHR and other HISs are Amazon; they supply the full spectrum of �products� users consume. Connecting these two is the �fulfillment company� (such as Vocera) that packages and ships what�s been �ordered�. Useful metaphor!
Another interesting observation she made: NO technology is inherently HIPAA-compliant. No matter how water-tight a system has been engineered, misuse can create security leaks. Ultimately, it�s the users who are responsible.
She also said, �Just say no to Big Bang. Instead, use rolling adoption. For example, start in the ED and then roll it out unit by unit to the rest of the hospital. Each must commit to change, maintenance, upgrades, education and support.� She recommends a shared governance strategy. �Plan and implement your communications strategy as carefully as you do your EHR strategy.�
Words for the wise.
top
|
| |

Pleading
the
fifth
February 28, 2017 --
How do you know your patient is in pain?
"He/she says so."
How much pain?
"He/she tells you a number from zero to ten."
This is what we are taught in nursing school -- the "fifth vital sign" -- and it is an article of faith. However, it is fraught with issues, not the least of them that it has legal repercussions, providing the foundation for lawsuits and in some cases substantial penalties. But is it a reliable indicator?
Not much, says Diane M. Goodman in The Pitfalls of Pain Scales in this month's Medscape.
This is a fascinating read, and an important issue for nursing and quality of care.
top
|
| |

Synapse
firing
October, 2014 --
Whoops! I forgot to toot my own horn!
Here is a link to an interview from three years ago.
The publication is UCSF's Synapse.
The topic is NurseMind and Nurse Tech, Inc.
Better late than never? NurseMind App Keeps Busy Nurses On Target.
top
|
| |

Gold
standard
January, 2017 --
When doing medical research online,
professionals do not use Google and Yahoo.
Anybody can write anything on the Web. Much of that is bunk.
Instead, base medical decisions on the gold standard:
controlled, randomized, double-blind clinical trials.
Official sources: Cinahl, PubMed, and Medline.
These are vast databases.
In them resides the most authoritative medical and nursing data.
To search in them, use MeSH (Medical Subject Headings),
a system maintained by the National Library of Medicine,
a limb of the National Institutes of Health and (ahem)
the source of some funding for my advanced degree.
Do your search using MeSH terms.
Here is an
example of MeSH terms
from my own specialty, medical informatics.
One way to select MeSH terms is with the
MeSH Browser
and with the
MeSH
on Demand service.
Best of success to you in your search!
top
|
| |

Data
for
sale
January 20, 2017 --
Our medical data is valuable and is bought and sold without our permission or even our knowledge.
Many people are worried.
About this, Adam Tanner has written Our Bodies, Our Data.
He says (in an interview with Reveal) that people would be "creeped out" if they knew.
My own feelings on the topic are mixed.
It is true that certain types of medical information -- substance abuse history,
sexual history, psych history, HIV status
-- are very private and should indeed be protected.
Other kinds of information, e.g. info that might influence an insurance carrier's decision,
should also be protected, at least from that kind of user.
However, some data mining, e.g. population health and epidemiological studies, are beneficial and should be permitted.
Most of my own medical data I don't care who sees.
You want to look at an x-ray of my broken arm?
Go for it.
You want to know when I had a flu shot?
Knock yourself out.
We are excessively protective of much of this data, and it creates obstacles to care that are unnecessary.
With a little education, the knee-jerk instinct to hide it unconditionally could be relaxed.
On the other hand, I do think that the uses of this data should be more transparent.
Some of the uses, e.g. marketing data for drug manufacturers and retailers,
should be tightly regulated and consumers should be able to find out about it if they want to.
top
|
| |

Quandary solved
January, 2017 --
RoseAnn DeMoro bills herself (on Twitter)
as Social Change and Activist for Life and
is the Executive Director of National Nurses United, the largest American organization of nurses.
She offers the Republicans a solution to the quandary in which they find themselves, having
vowed to repeal the Affordable Care Act but having nothing with which to replace it.
"Medicare for all," she proposes,
following in the footsteps of would-be presidential candidate Bernie Sanders who was himself not the first to propose this.
Whatever its provenance, it is an excellent idea. In effect, it would eliminate the insurance company middlemen
(parasites, I call them, as they add to the cost but not to the value of health care) and
would move us to a single-payer system.
This would yield numerous benefits, including the bargaining power to hold costs down
and to establish enforceable standards of care.
Is this not that what Mr. Trump promised (in words with fewer syllables)?
Even so, it is not a quick fix, requiring much careful planning and considerable complex language.
How would it be paid for?
What should businesses do with the money they would no longer need to spend on health insurance for their employees?
Numerous questions arise, all of which can be solved.
Radical though this proposal may be, the Repugs should embrace it
as it enables them to keep the absurd promise they made.
Everybody wins! Go nurses!
top
|
| |

Nurse, Advocate
January, 2017 --
Nurses are not known for being articulate. Other skills are more relevant to the job.
In nursing school, my writing skills were not recognized nor, indeed, of much use in nursing work.
Instead, what is respected is competence and, most of all, expertise.
The downside is that competent and expert nurses sometimes do not express themselves well.
Nurses are wonderful advocates for patients but poor ones for themselves.
The following brief treatise in defense of nurses
(especially in light of strikes and other conflicts with management)
is the words nurses might not find to speak or write but nonetheless feel in their hearts.
Here is an attempt to say what often is not said.
�I have a lifetime of experience doing this work, and every day on the job I give it all to my patients. They get everything I�ve got and that�s a lot.�
�The hospital wants to haggle over things like PTO (paid time off) and other benefits. No amount of PTO is equal to the genuine caring and � let�s say it! � life and health my patients get from me. It�s not something money can buy.�
�Given how much my extraordinary hard work and commitment contributes to (and sometimes saves) the lives of others, my own life outside of work should be trouble-free, to the extent that a paycheck and benefits package can provide. To haggle over compensation for something that is so precious and given so limitlessly demeans us all. It denigrates the priceless thing our patients seek when they come to us.�
It has been said, "Physician, heal thine self." To this we add, "Nurse, advocate for thine self!"
top
|
| |

Escaping the spotlight
December, 2016 --
The new President has promised to repeal the Affordable Care Act (ACA/Obamacare).
Fortunately, there are other important health care legislations that -- escaping the spotlight
of campaign rhetoric -- are evading his attack.
That's good because they, too, do things that are good for the American people. Here are a couple of them.
On October 14, Medicare payment reform legislation (Medicare Access and CHIP Reauthorization Act, MACRA) was finalized.
In essence, this law creates new, better ways for providers (mainly doctors) to be paid.
Of these, perhaps the most radical is termed the Merit-Based Incentive Payment System.
It creates incentives for quality (make more money when you give better care)
and -- dear to the hearts of us informaticians -- substantial incentives for the use of electronic health records (EHRs).
This latter initiative -- that has propelled our health care system toward electronic in place of paper record-keeping
-- has been driven by a program termed Meaningful Use.
It is part of the Health Information Technology for Economic and Clinical Health (HITECH) Act,
a component of Obama's economic stimulus package, crafted early in his
first term, a year or so before the Affordable Care Act (Obamacare) was passed.
Meaningful Use offered strong financial incentives to hospitals and to
physician practices and has been effective indeed.
In the seven years since HITECH was passed,
adoption of EHRs by hospitals has gone from near zero to 96%.
Having escaped the spotlight, HITECH and MACRA are likely to survive the new President's push to
"repeal and replace". And that's a good thing!
top
|
| |

TrumpCare?
December 5, 2016 --
Ann Farrell forwarded to me a copy of
the letter
Pam Cipriano, President of the American Nurses Association (ANA),
wrote today to president-elect Donald Trump.
Ms. Cipriano's heart is in the right place but in my view -- especially
given the misogynistic and obstruct-Obama-at-any-cost attitude of the
incoming Administration -- her plea for reason is rather anemic.
Most of what she requests is already granted by the Affordable Care Act (ACA).
Thus, this letter serves as a thinly-veiled intercession for its preservation.
Alas, there's not much hope for that.
What the letter doesn't say is that nurses had little input into
the writing of the ACA in the first place
and should -- no, must -- be involved in
the drafting of any such legislation as we go forward.
Pam, stop pulling your punches!
top
|
| |

Nursonomics
November, 2016 --
The economics of nursing is complex and important.
Typically, the cost of nursing service in a hospital is bundled into the room rate and not billed separately.
It is not a revenue center; it does not generate income.
Thus, nursing -- in most hospitals the single largest payroll category -- is treated as a cost center.
So -- as with any expense -- the conventional strategy is to minimize it.
This means hiring as few nurses as possible.
That's different from, say, the expense of a new CAT scanner machine.
The CAT scanner generates revenue each time it's used.
Nurses don't. Yet without them hospitals are useless.
With too few of them, patients die.
As reported in Medscape, The More RNs, the Higher the Patient Survival:
...each additional patient per nurse on a medical-surgical unit was associated with a 5% lower odds of survival
...below-target RN staffing patterns and high patient turnover increased the risk for patient death.
So what's good for patients is bad for hospitals' bottom lines.
With new mandates that tie reimbursements to outcomes, however, this is changing.
The time is ripe for new economic models for nursing.
top
|
| |

Trumbers
October 11, 2016 --
If you are the Donald, Obamacare is a disaster.
You cherry-pick your numbers to construct the worst possible picture.
But for plenty of folks, Obamacare is a success:
Trump�s Debate Claim On Health Care Costs: It Depends What You Mean By 'Cost':
"...when it comes to health care, there are many different types of costs: those for governments, employers and individuals.
And those costs don�t always go up and down at the same time...
Health care spending overall (as measured by the federal government) continues [to grow] at a historically slow rate."
There are plenty of numbers to paint whatever picture you want.
top
|
| |

Nurses,
learn
informatics!
August, 2016 --
Why learn informatics?
Nurses use computers every day.
They need to be good at it!
And nurses need to be more involved in decision-making about technology tools
We must advocate knowledgeably for what nursing needs.
When we are ineffective with technology,
we are held back as professionals and as industry strategists.
How should we learn informatics? Read my brief article, Nurses,
Learn Informatics!
top
|
| |

Balancing
act
August, 2016 --
You�d think that everybody in health care would want the same thing: health.
More formally, we call that outcomes;
the goal of doctors, nurses, and of course, patients should be
the achievement of the best possible outcome in the situation,
even if that is, say, a death with pain minimized, or a chronic disease managed.
But it�s not so.
However, the wants of each player are surprisingly different.
Here I�ll discuss the situation that is most familiar to me, the acute care hospital.
When he is there, the patient wants meals, to be warm,
to receive timely responses to his call bell, and to be helped to the bathroom ASAP.
The nurse, on the other hand, has quite a different list of wants.
She wants to know clinical data such as WBC (white blood cell count, a measure
of response to infection) as part of her mental model
of her patient�s health status,
to be able to deliver meds on time because that is an important measure of her performance,
to prevent falls and bedsores because these are indicators of quality of nursing care,
to be confident of the appropriateness of meds orders since she,
ultimately, is the one administering them,
and that pain meds are adequate because she is the one
witnessing suffering and managing it within parameters determined by others.
Sometimes these differing goals are in conflict.
For example, going to the bathroom might risk a fall.
Letting a patient sleep undisturbed might risk a pressure ulcer (bedsore).
In summary, health care processes are complex and the motivations of its participants are surprisingly divergent.
Managing all this so that all needs are met is a remarkable balancing act that nurses do every day.
top
|
| |

It's
the
workflow,
stupid
August, 2016 --
When nurses complain that the technology-based tools (especially EHRs)
that they are tasked to use slow them down, usually what they mean
is that these tools don�t model their workflow.
We talk about workflow a lot! But what is it? Why is it so important?
And why is it so hard to model with computerized/electronic/mobile tools?
Please see my
August 2016 NurseMind blog entry for the full story.
top
|
| |

RN
+
Rx?
July, 2016 --
Should RNs prescribe pain meds?
Our scope of practice denies us this important function, perhaps appropriately so.
We don�t want this responsibility but we often want more participation in the decision.
Often, the order is insufficient and the patient is suffering
(perhaps due to the prescriber's addiction phobia),
or it is excessive and the patient is being snowed.
The RN is more in touch with the patient from moment to moment and, at least in terms of pain,
often has a better sense than the MD of what�s really going on.
We do have a professional certification
for pain management and even the
American Society for Pain
Management Nursing but even the best-equipped nurse can be no more
than a "caring advocate" and an advisory (not decision-making) member
of the professional team.
Is it time to enlarge our scope of practice?
top
|
| |

More
war
stories
June, 2016 --
Here are some more war stories, focused on issues with the EMR. My friend Pat works in a peri-op unit, so her stories relate to peri-op workflow. Here are four.
War story 1: The patient's chart says NKA (no known allergies), and that it's been reviewed by another RN.
However, at admission, the patient says yes, they do have allergies to several meds.
So Pat asked the RN who had left the allergies field blank why.
That RN said, allergies weren't relevant at the time;
"I was working on something else and had to click through that screen to get to the part where I could do what I needed to do."
In other words, the EMR did not model that nurse's workflow. A serious medical error was narrowly averted.
War story 2: When you scan a document, a stripchart, or an image into the EMR, you must name it. What name should you use? Into which folder should you store it? There is no standard. Different departments use different conventions. Thus, it is often difficult to find a document or image scanned by someone in another department. You must call and ask them what it is called and where to find it in the EMR.
War story 3: HIPAA rules create obstacles. For example, a patient recently had an EKG at another site and didn't sign a release. The RN at our site needs to see the EKG in preparing the patient for the OR (operating room). So she gets another (redundant, expensive) EKG. This is quicker than attempting to obtain access to the existing one and enables Pat to get the patient to the OR on time.
War story 4: Reconciling a patient's meds must be done in preparation for an OR procedure. It takes an hour to do. Shortly thereafter, the doctor or the patient decides to delay the procedure by a week. A week later, when the RN re-does the admission process, she cannot find the existing medication list and must repeat the one-hour reconciliation process though nothing has changed. The information is in the system somewhere but the RN can't find it.
It's a war out there... but with whom are we fighting? Often, it's our own tools and processes.
top
|
| |

Nurses
are
underserved
June, 2016 --
Nurses are surprisingly underserved by technology. Paradoxically, much of what they do involves computers and complex electronics such as pumps and monitors. In particular, nurses spend a lot of time working with electronic medical records. However, these tools are patient-centric, not nurse-centric. In other words, using these tools, nurses contribute substantially to the quality of patient record-keeping, care delivery, and billing, but the tools do little to support the work of nurses themselves. There is a large gap in the spectrum of nursing knowledge- and process-based tools.
The reasons are twofold. First is economics: nursing is a cost center rather than a revenue center. Unlike medical procedures and supplies, most of what nurses do is not directly billable. For example, an appendectomy or a pill generates a charge on a bill for which a medical institution is paid, whereas most of the expense of nursing is, from the financial standpoint of the institution, overhead. The cost of most nursing care does not appear as line items on medical bills; it is bundled into hospital room rates and into the charges for procedures. As with all bundled expenses, the incentive is to reduce them. Whenever possible, spend less on nursing. This makes tools for nurses hard to sell and thus industry rarely develops them.
The second reason is the complexity of nursing work and its workflow. At Nurse Tech, Inc., we have given this much thought and propose that a good starting place is, as Drs. Gawande and Pronovost have done for surgeons, the creation of checklists for nurses (NurseMind). Unlike surgeries that are discrete units of work, usually comprising a clearly-defined set of goals and predictable branching paths through the course of procedures, nursing work encompasses entire work shifts and are more varied and fluid in how their content evolves. They would be impossible to capture in static printed checklists. Rather, they require the more complex support that can be provided by algorithms (such as the one we have patented) on mobile devices such as smartphones.
In this environment, an app can build nursing task lists by drawing on a variety of sources: nursing units' descriptions of how they provide care (e.g. who takes vital signs? who manages physical resources such as carts and trays?), what diagnoses patients have that demand additional nursing tasks (e.g. diabetes care, central and intravenous lines, catheters), new orders that are received during the course of the shift, changes in patient status, and follow-ups (e.g. lab results, communications with colleagues, requests from families) that must be remembered. The context and its demands are fluid and rapidly changing, and the checklist tool must reflect that without slowing the nurse down. We believe that in the app we have built we have largely satisfied these demanding and complex goals.
No app can replace the nurses' clinical judgment and critical thinking. In early versions, we attempted to build algorithms for assigning priorities to tasks but soon concluded that there is no way to automate this. However, it is appropriate for nurses to have tools that support them in the routine parts of their work. This enables them to make fewer omissions and consistently deliver top-quality care. Most importantly, by relieving the cognitive burdens of the routine work, mental space is freed for the higher level thought processes.
It is time for nursing to receive the technology support that it needs and deserves.
top
|
| |

War
story
June, 2016 --
I love the war stories recounted by nurse heroes. Here is one by my friend Terri Olson. She recounts:
In 1984, I went to Eagle Pass, Texas for a travel nurse assignment. There I saw some things I will never forget.
The hospital had a splendid view of the Rio Grande.
From the windows, we could see people wading over from Mexico to deliver their babies.
Thankfully, in recent years the quality of care in Mexico has mostly caught up with ours.
I was assigned to a med/surg unit, which was where they put patients of every description.
Med/surg served as the catch-all unit, providing services that should have had specialized units such as peri-op.
We received patients directly from the OR on monitors and requiring constant surveillance.
However, the monitors were in the patient rooms not at the nursing station, so we were unable to watch them.
So I literally ran from room to room in constant panic hoping I wouldn't walk in and find a dead patient.
None of the other hospital staff thought that was a big deal.
I had a hissy fit and quit after six weeks.
Thankfully, the design of hospital nursing units has gotten a lot better since then.
top
|
| |

Bundling
and
engagement
April 5, 2016 --
Today I attended Northern California HIMSS's 4th Annual Patient Engagement Summit
at Stanford University. A majority of the attendees were, like me,
vendors of healthcare technology. The experience was most worthwhile.
We all learned a lot.
Perhaps the most interesting session was entitled Payer Challenges.
Payers include insurance companies, health plans, and the data analysts
who work for them. It was eye-opening to hear their side of the
healthcare story.
We learned that this month, under a provision
of the ACA, bundled payments have gone into effect.
This replaces -- on a voluntary basis -- the more traditional and likely
less effective (from a cost-savings and quality-of-outcomes viewpoint)
fee-for-service payments.
At the CMS web site, the concept of bundled payments is described:
Traditionally, Medicare makes separate payments to providers for each of the
individual services they furnish to beneficiaries for a single illness or course of treatment.
This approach can result in fragmented care with minimal coordination across
providers and health care settings.
Payment rewards the quantity of services offered by providers rather than
the quality of care furnished.
Research has shown that bundled payments can align incentives for providers
� hospitals, post-acute care providers, physicians, and other practitioners
� allowing them to work closely together across all specialties and settings.
A bundled payment is for a single episode of care (e.g. a hip replacement)
and is made to a hospital that then pays the various caregivers such as the
surgeon, the physical therapist, the pharmacist, etc.
The amount of the
payment remains fixed even when the patient must
be readmitted to the hospital within 90 days.
If that happens, the hospital will likely lose money.
Thus, the incentive
is strong to coordinate caregivers to work as a team,
focusing above all on outcomes thus avoiding that readmission. Indeed, research has
shown that the incentive works -- costs go down and quality of care goes up.
Here
is a brief tutorial and video about bundled payments.
Not by accident, an effect of bundling payments is the incentive for patient engagement,
the topic of today's conference. Involving the patient in their own care is essential
for good outcomes. Also, the provider becomes motivated to pay attention
to patient-reported outcomes. Now the financial rewards are aligned with these
care-improving behaviors.
I have written about this concept of patient engagement in a different context,
that of healthcare's shifting paradigms.
The old paradigm was discharge planning.
Now we strive for lifestyle change.
Today's conference was timely indeed.
top
|
| |

PHC
62
March 23, 2016 --
Another amazing day
(#62) with Project Homeless Connect.
I saw sixteen patients. Yes, we're supposed to call them clients,
but their medical needs were so great. I saw meth users, a
MRSA victim with an active infection, lots of lice, a paranoid schizophrenic,
and a guy who had been awake two days straight, walking around the city,
because he has no place to lie down.
PHC provides an amazing array of services, everything from
banking to foot washing.
Society at large does little for these folks.
It falls to volunteers like me and the heroes who run PHC.
Is that any way to run a country?
top
|
| |

Little
guys
March 18, 2016 --
Sometimes it's not the big guys who are at the top of the nursing education game.
Unlike the major nursing schools of the Bay Area,
little Holy Name U. has Nursing Informatics course offerings in its curriculum.
Not only do the bigger players (I won't name names, but you know them!)
have no such courses, they are not interested.
Given that today's nurses spend more time in front of the computer
than in front of the patient, why don't all the schools do
what HNU is doing?
Today I attended HNU's annual nursing symposium.
Though the essential purpose of events such as this one is recruitment,
I did learn a lot and found the majority of the presentations
valuable and even eye-opening. Go little guys!
top
|
| |

Financial
incentives
March, 2016 --
I believe that people who call for abolition of the
ACA would not do so if they knew what's in it.
So here's another little bit of ACA 101.
We all want better, cheaper healthcare.
The ACA drives improvements in quality and decreases in the cost of healthcare.
One of the mechanisms for accomplishing this is financial incentive.
The ACA has three specific financial incentive programs:
- Value based purchasing (VBP) � outcomes, satisfaction, quality, safety � metrics that
drive "booster" payments.
- Readmission reduction program (RRP) � reduce 30-day all-cause readmissions for patients with
CHF, pneumonia, and other conditions that can best be treated at home.
This can be accomplished through coordination of care providers, patient education, and more.
- Hospital-acquired conditions (HAC) � Medicare and various ACA programs no longer reimburse for
the curing of falls, air embolisms, urinary tract infections, central line-associated blood stream
infections, surgical site infections, and various others including MRSA,
CDI (Clostridium Difficile infxn).
These are all common sense, evidence-based measures to help change
healthcare in directions we all support.
top
|
| |

Big
Data
March, 2016 --
Can machines discover medical knowledge?
In a frank interview with Dana Ludwig, MD, this notion and many more are discussed.
Medical data is huge and complex.
The Epic electronic health record alone has 13,000 tables, and there are many more databases to mine.
Ludwig says,
Machine learning algorithms might find associations that I don't know about by crawling through the massive tables.
Given the 100,000 variables that we have on line, have the machines crawl through and see which ones are predictive
of [some] diagnosis code.
I don't know whether the algorithms can do a better job than the experts can do, but I'd like to find out.
The goal of the neural networks is to let the algorithm discover the attributes that are predictive rather
than presupposing that the experts can name them.
Can machines make discoveries that human experts cannot?
Read the interview here.
top
|
| |

Vaccinations
Revisited
March, 2016 --
Remember back in 2009 when I listed all the vaccinations?
Here's the real list, the
CDC's Code Set CVX -- Vaccines Administered.
top
|
| |

Healthcare
Econ 101
February, 2016 --
With ours being the most expensive healthcare system ever, its economics are increasingly topics of debate.
Here are a few basic principles that drive our dysfunctional system.
Financial reward motivates every business, healthcare among them.
What is rewarded increases.
In an ideal system, providers are rewarded for good outcomes.
There are some incentives for this in the ACA and in Medicare
including patient satisfaction surveys that have been made a
factor in hospital reimbursement by government.
However, in healthcare's predominant economic models, the rewards are neither for outcomes nor for quality.
One such traditional model is fee-for-service.
The result is, of course, more service.
(This was discussed in my blog post Doctors as Businessmen.)
Another common model is capitation.
A provider network is reimbursed a fixed amount for each patient.
So the result is more patients. In capitation models, the scramble is for market share.
In any model, the physician says, when the patient is in front of me, he is the most important person.
After he leaves, the most important person is the payer.
The conclusion: healthcare and economics will always be an uneasy mix.
top
|
| |

Obstacle?
Opportunity!
February, 2016 --
The first obstacle a new grad nurse encounters is
the dearth of jobs for new grads. It's easy
to get into nursing school. Afterward, it's
hard to get that first job. The schools don't tell us this.
Reluctance to hire new grads is understandable from
the hospitals' point of view; a new nurse
is a big investment. It can be months before
she (almost always a she; my graduating class
was 85% female) reaches full productivity.
Something that is also not discussed is the content
of nursing education. The schools are obsolete!
What I saw in nursing school: a bunch of grizzled
old farts who couldn't cut it as actual nurses ("those
who can't, teach") and who haven't kept up with
the rapidly-changing world of healthcare.
Case in
point: today's nurse spends quite literally more
time in front of computers than in front of patients
(proven by numerous studies). Yet
informatics courses in nursing school curricula
are rare.
Even at national leader UCSF, my alma mater,
Dean Vlahov declined my request to meet
to talk about this.
The result? Nurses helpless and
frustrated by technology, decreased productivity
and reduced safety, defying nursing's #1 mandate.
The upside? This is an opportunity. My software
projects will enable technology to
be a help rather than an obstacle for nursing.
top
|
| |

Get
real
February, 2016 --
In today's climate of presidential campaigns, right-wingers are
still calling for
repeal of the ACA?
Get real!
Deep down, those echo chambers know how badly that would backfire.
Insurance companies -- huge campaign donors -- would see a steep drop in profits.
Lots of ordinary folk would suddenly lose healthcare coverage.
People with "prior conditions" would be back out in the cold.
Medical bankruptcies would resume.
Hospital and provider revenue streams would be disrupted.
A lot of people would be very angry.
I think what's happening is -- as they do with environmental and other regulation
-- the right-wingers clamor in public but in private they count on cooler heads to keep them safe.
top
|
| |

Cool
gig
January, 2016 --
Here is Dr. Dan Weberg RN speaking at a medical technology conference.
He works for Kaiser.
His title is Director of Nursing Innovation.
Doesn't that sound like the coolest gig in the world?
top
|
| |

Work
to
do
 November 18, 2015 --
Today at the AMIA conference, Dr. Bob Wachter, faculty member of my alma mater UCSF and author of the thought-provoking The Digital Doctor: Hope, Hype, and Harm at the Dawn of Medicine's Computer Age, gave a great talk on that theme.
November 18, 2015 --
Today at the AMIA conference, Dr. Bob Wachter, faculty member of my alma mater UCSF and author of the thought-provoking The Digital Doctor: Hope, Hype, and Harm at the Dawn of Medicine's Computer Age, gave a great talk on that theme.
As is unmistakeable in this wonderful image he showed -- "A 7-year old girl's depiction of her MD visit" -- in which the MD is completely focused on his computer not on the patient (click to see it full-size) we in medical technology have a lot of work to do.
top
|
| |

General
Zuckerberg
November 21, 2015 --
Today I attended the ribbon-cutting dedication of the new
Priscilla and Mark Zuckerberg San Francisco General Hospital (SFGH) and Trauma Center building.
Present at the occasion were Zuckerberg (in his trademark tee-shirt and jeans,
chatting with California Lieutenant Governor Gavin Newsom in my photo),
Congresswomen Nancy Pelosi and Jackie Speier, San Francisco Mayor Ed Lee (wielding the giant scissors),
venerable news anchor Belva Davis, and many more.
The building itself ($880 million) was paid for by a City bond. Zuckerberg's gift of $75 million
paid for the equipment and technology inside it.
We toured the new facility. It is the most efficient, high-tech and
well-designed emergency department I've seen. Having volunteered in
its predecessor (across the courtyard, still running) I have seen the
superb medical care that is delivered here. When the new facility opens
in March, 2016, it will be even better.
top
|
| |

Coding
Nursing
November 18, 2015 --
Here is another reflection following the
American
Medical Informatics Association's 2015 meeting (AMIA) that
ended today. It regards data coding standards for nursing and
is woefully neglected, even here at AMIA. The topic is important
for nursing because without a good coding scheme, we cannot capture
data about what we do. Without that data, we cannot make the
important case for the value that we create for healthcare.
As I have discussed here,
there are several encoding schemes for nursing data. The best one for
the purposes of nursing and data processing is Virgina Saba's (about whom I blogged
briefly here)
Clinical Care Classification System
but alas it hasn't received the wide uptake it deserves.
Dr. Saba herself attended the conference (we lunched) and -- as
one of the grand dames of nursing informatics -- presented the
Virginia K. Saba Informatics Award.
At AMIA, the only nursing coding scheme I saw discussed was
International
Classification for Nursing Practice (ICNP), an international standard
and nursing-centered but not as well suited for computerization.
Perhaps this is an area for discussion at a future AMIA.
top
|
| |

AMIA
2015
November 18, 2015 --
Today was the closing day of the American
Medical Informatics Association's 2015 meeting (AMIA). As always, I learned a lot
from the technical
talks and came up to date on issues and trends in this busy, burgeoning industry.
The closing keynote speech was by Dr. Bob Wachter (here is his blog,
Wachter's World)
in which he gave us an impassioned
exhortation to remedy the numerous ills of healthcare IT. The audience clapped
frequently, sharing his enthusiasm for the as-yet-to-be-realized potential (and
numerous humorously-described flaws) of the immature technology we're all working on.
For example, he observed that it is not enough to write good software; we must also
reimagine the work itself.
Wachter's talk largely paraphrased his recent book, The Digital Doctor that I
have mentioned here and of which I promise
a review soon. The book was a terrific read and the speech today was equally heartening.
Go Bob! Go AMIA!
top
|
| |

Innovate!
November 12, 2015 --
Today I toured Kaiser's
Garfield Innovation Center where they simulate hospital and home environments for testing
new technologies and refining caregiver workflows.
As with the military, Kaiser's processes for evaluating, selecting, testing and rolling out new
tools and technologies are ponderous and lengthy. Often, by the time all the maintenance
and support procedures are implemented, impacted work processes are updated, and staff are
trained, the tool or tech is old news. But there are no short cuts. When you are steering
a battleship, you must turn the wheel five miles before the ship responds.
One such innovative change touted at Garfield that is already old hat to
us nurses is the don't-interrupt-me-while-I give-meds yellow sash.
Simple as it is, it does work. Uninterrupted, the nurse is less likely to make a medication
administration error. Yet it had to be tested in a safe environment, and
the Garfield Center served this purpose well. Today, most nurses in hospitals use
these sashes (or something similar) and error rates have gone down.
Another new technology -- this one dear to me as a proponent of mobile
solutions for nurses (such as my NurseMind app) --
is smartphones. Kaiser is evaluating various ruggedized versions and deploying them
for a variety of purposes such as secure messaging. I hope they will also consider
checklists such as the nursing one I have built... And deploy it at the Garfield Center!
top
|
| |

Boot
camp
September, 2015 --
Nursing Informatics Boot Camp was this week.
Organized by the Northern California chapter of HIMSS (thanks!)
The instructor was my friend Susan Newbold. She knows her stuff. Glad I went!
top
|
| |

Yes vault!
September, 2015 --
Success! Kaiser and Epic came through after all. And so did HealthVault.
If you're a Kaiser member, you can download the last five years or so of your
electronic health record in CCR format. Here is how:
- Login to Kaiser's web site.
- Find the medical record page and click the download link. You'll get a zipfile.
- In the zipfile, find the file named DOC0001.XML
- Upload it to your HealthVault account. Bingo!
And thank Obamacare Meaningful Use Stage 2.
We can all have our data in our PHRs now.
Hurray!
top
|
| |

No vault
September, 2015 --
Here's the main part of the letter Microsoft HealthVault
provided for me to send to my health care provider (Kaiser):
Please send my medical information from your medical
records system directly to my personal HealthVault
record using my Direct address.
I'm taking an active role in my health and wellness
by keeping a personal health record in HealthVault.
If you are using an electronic health record (EHR)
system that is certified for Meaningful Use Stage 2,
then your software may be able to generate a CCDA
and send it to me using the Direct protocol.
(As you may know, Direct is a security-enhanced
health messaging protocol designed to help protect
health information when it is sent from one
computer system to another.) Your EHR software
vendor should be able to provide instructions.
[Kaiser uses Epic... Amazingly, it's not
retrofitted for MU2! See below.]
Please read How healthcare providers
can benefit from HealthVault (fascinating!)
for more information about HealthVault and
how it supports Meaningful Use Stage 2 (MU2).
I sent that letter to my Kaiser doctor.
Here's what my doctor wrote back:
Daniel S Keller
From: [Nameless MD]
Received: 8/27/2015 4:26 PM PDT
Hi Dan - Sorry I am unable to do that directly.
All our Epic secure messages must go through our system.
You will always need to log into KP.org to retrieve them,
though you will get a notice to your regular email saying
you have a message. I have nothing to do with the system
or contacting the vendor. You can get your medical record
on a thumb drive. You can go to member services for that.
The phone number for Member Services is 1-800-464-4000.
They may be able to help with your questions about
HealthVault, too.
Hope that helps.
Best,
[Nameless MD]
Turns out you can only get a CD, and it contains only PDFs
of your medical record. In other words, Epic (with Kaiser's collusion?)
is making sure you cannot do what HealthVault and I are trying to do.
Discussions with Kaiser's medical records department member support
people were pointless. They had never heard of CCD nor even MU.
So Epic sucks again. I hope their customers (ahem, Kaiser?) find a vendor who
actually delivers on MU2. Go HealthVault!
top
|
| |

Good vault?
August, 2015 --
Here are some things I like about a PHR (personal health record) such as Microsoft HealthVault:
- It could free me from those sucky "patient portals" such as Kaiser's HealthConnect, one of Epic's
"features" that primarily serves the institution and only secondarily the patient (as I've blogged
here and here).
- It gives me a little more access to my data, and a little more control over it.
I can actually enter and update my medical data myself and, to a limited degree, grant access to it to others.
- The Continuity
of Care Document (CCD) protocol/format is a long-overdue advance from lame old HL7.
It is a good thing and should be universal.
- Another good thing in Obamacare is MU2's requirement that health care providers exchange data including patient demographics,
problems, test results, immunizations, allergies, care plans, and more. Here are some of its objectives:
- Use secure electronic messaging to communicate with patients on relevant health information.
- Automatically track medications from order to administration using assistive technologies in conjunction with an electronic medication administration record (eMAR) (for hospitals).
- Provide patients the ability to view online, download and transmit their health information within four business days of the information being available to the eligible provider (EP).
- Provide patients the ability to view online, download and transmit their health information within 36 hours after discharge from the hospital (for hospitals).
Go HealthVault!
top
|
| |

How
sick?
August, 2015 --
An issue of perpetual contention in nursing is staffing.
How many nurses do we need on staff right now, for the present patient load?
Management wants fewer (to save money) and nurses want more (to get all the work done).
Where's the science?
One way to make staffing decisions is based on acuity -- how sick are your patients?
Today, staffing decisions are based on crude estimates drawn from patient diagnoses.
If they're very sick, hire more nurses.
But there is a better way. Degree of sickness is not the best indicator of nursing workload.
Instead, I propose a measure of acuity that is the number of minutes of nursing work remaining
to be done for each patient. Nurse managers would, in real-time, use a tool
that adds up all the durations of
the outstanding tasks for each of the patients currently on the unit. A lot of minutes means
you need more nurses. How many? Divide the minutes into the duration of a shift. Voila!
Accurate nurse staffing!
This measure was developed working with seasoned veteran emergency/charge RN Mark Wandro.
We propose a study to confirm that
this new measurement of acuity (and the tools that support it) can improve nursing
outcomes.
Is your hospital interested? Can you sponsor this study? Please get in touch!
Let's make nursing better!
top
|
| |

Nurses
more
than
ever
August, 2015 --
In this videoed
interview with Pam Cipriano entitled Why Nurses Matter More than Ever, Ms Cipriano --
an old guard union booster -- makes an important point. But it's based on nursing's traditional
battle about staffing levels. This pits us directly against management that seeks to hold down costs.
Recall, payroll is a hospital's single largest expense. Nurses are often its largest component.
Ms Cipriano is right but for reasons other than what she states. Now reimbursements --
thanks to the ACA -- are partly based on quality measures and, most importantly, on outcomes.
In its central role, the quality of nursing care has risen to what is perhaps the most
essential factor in determining outcomes.
Our union does an important job in enabling us to work well but we need to move beyond
those tired formulae and focus on how we deliver the high quality health care that America demands.
What we nurses need to enable us to deliver these ever-better results should be the goal for
which our union contends. Ms Cipriano fights a good fight but could do better by enlarging her goals.
Adequate staffing is necessary but not sufficient.
We also need tools (especially mobile ones such as
NurseMind), participation in decision-making,
representation in the C-suite (every substantial health care organization should
have a CNIO), evidence-based protocols, and much more.
In Nursing: Essential to Healthcare Value in Nurse Leader,
a model begins to emerge. Authors Pappas and Welton propose to "...define nursing value
as the function of outcomes divided by costs." The model is rudimentary but it's a good start.
What you can't measure you can't manage. The model begins to tell us what to measure.
The point is that, with reimbursements tied more than ever to outcomes and perceptions of
quality, nurses are essential to health care revenue.
Hospitals, make sure your nurses have what they need to deliver the results you need.
When we do our work well, you are reimbursed well and -- most importantly -- patients get good care.
top
|
| |

Numbers
August, 2015 --
The numbers are in. The homeless have been counted. I was one of 400 volunteer counters on
Jan. 30th as I recounted then.
But first, how exactly is homelessness defined?
The federal government's definition excludes many whom we in SF consider homeless.
They exclude:
...individuals who are "doubled-up" in the homes of family or friends, staying in jails,
hospitals, and rehabilitation facilities, families living in Single Room Occupancy (SRO) units,
and in substandard or inadequate living conditions including overcrowded spaces.
In accordance with the federal rules, we did not report the numbers of these people, but we
hope that eventually they, too, will be included and eligible to receive the services they, too, need.
Here is a summary of what we found in the 49 square miles that comprise San Francisco:
- 6686 homeless adults, 250 more than were counted in 2013
- 853 homeless youth, 61 fewer than in 2013.
For the details, please see the full report.
top
|
| |

Yes, patients
August 12, 2015 --
Fascinating meeting today with Dr. Howard Landa, CMIO of Alameda Health System. He is
implementing
EHRs in their five-hospital system.
Though his job is technology, his thinking is all about the patient.
In describing the systems his team builds, he regularly refers back to what patients need,
what they experience, and the quality of what's delivered to them.
When we do our jobs right, this is how we do them. Thank you, Howard. You are a great role model!
top
|
| |

Go Bernie!
Go nurses!
August 10, 2015 --
National Nurses United (NNU), our Washington advocacy group, has officially announced our endorsement
of the candidacy of Bernie Sanders for President. Here in Oakland, no less.
(I have extolled his principled positions on prior occasions.)
In this picture he is with Executive Director RoseAnn DeMoro who says,
"His issues align with nurses from top to bottom."
Please read the press release for details.
Once again, we nurses are on the right side of history!
top
|
| |

ACA
for
whom?
August, 2015 --
The ACA has delivered substantial benefits for many Americans but the citizenry is not its primary beneficiary.
In an excellent July, 2015 article entitled "Wrong Prescription?
The failed promise of the Affordable Care Act", Trudy Lieberman in Harpers Magazine reviews
what we've learned in the five years since its passage.
"[It] was a canny restructuring of the American health-care marketplace, one that delivered millions of new
customers to insurance companies, created new payment mechanisms for hospitals, steered more business to pharmaceutical companies,
and dictated expensive, high-tech solutions for a wide range of problems."
Though medical bankruptcies seem likely to diminish, 17 million more (woefully far from all)
Americans have health care coverage, no one can now be excluded due to a pre-existing condition,
the growth in health-care costs has slowed and, on balance, we seem to be a little better off than without ACA,
it is clear that insurers and big pharma -- not health care "consumers" -- are the winners.
All that lobbying paid off.
"Because of a failure of nerve and the immense power of health-care
stakeholders, the A.C.A. has reinforced and accelerated many of the system�s most toxic features."
We still need single-payer.
top
|
| |

Cool
clear
Brooke
July 31, 2015 --
My favorite podcast, On the Media,
yesterday delivered an incisive and scathing look at the way
health and diet news is reported in popular media,
popping many bubbles of
conventional wisdom.
Its anchor
Brooke Gladstone
(this week without her equally brilliant and wry co-anchor Bob Garfield) subtitles this piece,
"High colonics, vampire facials, and the magical thinking that fuels an industry."
Ms Gladstone righteously and accurately excoriates,
as an example of the irresponsible and sensationalist writing that passes for journalism,
an article that proclaims that kale is actually bad for us, describing it as "stunningly unsubstantiated."
This is just one article in an endless parade, she tells us, that trumpet the newest food "breakthrough" or
"medical miracle" or "first of its kind" or "game changer" or "new standard of care" that will kill us or save us.
Other examples are omega-3s, dark chocolate, red wine, cell phone radiation, yo-yo dieting, and don't get her started on gluten.
She cites a genuine expert regarding gluten and the diet craze that now surrounds it.
For people who don't have a diagnosed case of celiac disease (i.e. more than 99% of us),
clinical trials have found no benefit in avoiding these foods.
The popular frenzy that now surrounds supposed gluten-sensitivities is just the latest example of the effectiveness of the pop science press.
She further reports that there is no such thing as a "simple screening test."
If a story claims this, run for the hills!
Screening test decisions should actually be among the most complex that we face in all of our health care decision-making.
What will we do with the results?
It is very difficult to ignore a positive, even when the treatment decision that seems inevitable does more harm than good.
She warns us not to confuse -- as many such articles would have us do -- risk factors with actual diseases.
The classic example is LDL cholesterol and heart disease.
The public has fixated on their serum cholesterol numbers instead of on the numbers that really matter:
the rates of death from heart disease. Beware, she further exhorts us, of the representation of normal
conditions such as baldness by the "disease-mongerers" as pathologies.
In all these cases, the objective is, of course, to drive spending with fear.
Of the numerous myths she debunks, my favorite is the one about drinking eight glasses of water a day.
It's just not true. There is no evidence that all this water, as Jennifer Anniston has claimed
(in an example of what is termed marketing by celebrity culture) will make your skin glow.
Drink water when you're thirsty. That's all you need.
How do these stories come to be? Ms Gladstone interviewed John Bohannon of Science magazine who describes their typical trajectory:
launch a study of some popular food or behavior, "...do a bad job with the statistics and the design of the experiment, get a bad paper published,
and then build a global multimedia campaign around it... There are diet fads that come like tsunamis every few months.
Why have journalists missed this?" Well, Ms Gladstone hasn't and I am grateful for her rare, honest voice.
Here is her Skeptic's Guide to Health News and Diet Fads.
top
|
| |

Interopera-
wha?
June, 2015 --
My friend and former classmate, the highly accomplished Dr. George Krucik laments the ACA's failure to
demand interoperability among healthcare data software vendors and systems. You got that right, George!
Indeed, Meaningful Use fails to call for EHR interoperability -- a serious omission.
However, it does call for specific types of data to be exchanged between specific types of providers.
For example, deservedly-maligned patient portals (that I've blogged about) will
be required to share certain data such as lab results with patients and with the ordering providers.
Medication reconciliations will be required to be shared among providers.
Hospital discharge information is to be reported to third parties (payers, mainly).
And there are a few more dribs and drabs of data that must be captured and shared.
These are baby steps but that's as fast as our industry can go. Keep pushing, George!
top
|
| |

Defending
their
turf
June, 2015 --
So it's data silos not missile silos but both provide formidable defense.
For the EHR vendors, one way to defend their turf is to not share their data.
In other words, with data silos.
Bad news for the FHIR folks.
No EHR vendor will expose all their data fields to any public API
(Application Programming Interface).
This will make it hard for people like me to build useful medical apps.
It's a deadly blow to any notion of medical data access and sharing, and
ought to have been forbidden by the ACA...
Oops, bad oversight!
top
|
| |

Dentist
regent
May 22, 2015 --
As a member of the committee that chose him, I am proud to announce
the selection of Harvey Brody, DDS, our next alumni regent.
He is the first dentist to serve as a regent of the University of California.
The announcement is here.
The last alumni regent from UCSF (2007-2009) was
Dave Shewmake.
Like me, Dave was a graduate of the Medical Information Science Section of UCSF's Graduate Division.
Serving as a regent was one of Dave's peak experiences, as it will no doubt be for Harvey.
Congratulations, Harvey!
top
|
| |

Woulda shoulda
May 2015 --
In his brand new (May 2015) book, The Digital Doctor, Chair of UCSF's Department of Medicine
Dr. Robert Wachter reports
David Brailer's (G. W. Bush's healthcare technology czar) comments
on the ambitious Health Information Technology for Economic and Clinical Health (HITECH) program.
I think Brailer nailed it.
He told Wachter that "HITECH locked in an existing set of clunky products
and led the computer vendors to focus on meeting federal requirements [Meaningful Use]
rather than innovating" (p. 18).
Existing vendor hegemonies (especially Epic) were thus strengthened by the financial pressure on provider
organizations (especially hospitals) to hurry up and computerize, regardless of quality.
Instead, Brailer says, HITECH should have spent its $30 billion (yes, with a B) on:
- standards,
- interoperability,
- a "Geek Squad" to help with training and implementation, and
- creating a cloud-based "medical Internet".
Perhaps Wachter, Brailer, and other visionaries can guide us in a more productive direction.
top
|
| |

Nursing volunteer
May 18, 2015 --
Considering volunteer nursing in a distant disaster zone?
Fellow UCSF grad Joe Niemczura is doing this in earthquake-stricken Nepal and writes an
excellent blog. Squat toilets, "water discipline", modest dress, and cultural sensitivity are just the beginning.
Kudos to you, Joe, a volunteer nurse sharing "your gift to the world."
top
|
| |

Military nurses
May 13, 2015 --
A new hero! This (unnamed) nurse at Guantanamo Bay, Cuba, refused to force-feed detainees.
As is plainly visible to everyone but the willfully blind, doing so would have violated the
code of ethics we nurses swear to.
Read
about it in Military Times.
This sheds new light on the world's most powerful military, regulated at least a little by
ethics and humanity. If you are looking at nursing career options, consider What's
Inside a Military Nurse's Toolkit? and take hope from our new nurse hero.
top
|
| |

Overkill
May 11, 2015 --
In today's New Yorker, Dr. Atul Gawande hits yet another home run:
"Overkill --
An avalanche of unnecessary medical care is harming patients physically and financially. What can we do about it?"
He writes:
[We have] a new, unanticipated problem: ...the correct diagnosis of a disease that is never going to bother you in your lifetime.
We�ve long assumed that if we screen a healthy population for diseases like cancer or coronary-artery disease, and catch those diseases early,
we�ll be able to treat them before they get dangerously advanced, and save lives in large numbers. But it hasn�t turned out that way.
For instance, cancer screening with mammography, ultrasound, and blood testing has dramatically increased the detection of breast, thyroid,
and prostate cancer during the past quarter century.
We�re treating hundreds of thousands more people each year for these diseases than we ever have.
Yet only a tiny reduction in death, if any, has resulted... [emphasis mine]
The medical system [does] what it so often does: tests, unnecessarily, to reveal problems that
aren�t quite problems to then be fixed, unnecessarily, at great expense and no little risk.
Meanwhile, we avoid taking adequate care of the biggest problems that people face -- problems like diabetes, high blood pressure,
or any number of less technologically intensive conditions. An entire health-care system has been devoted to this game.
Yet [with the ACA and new standards of practice] we�re finally seeing evidence that the system can change.
He also follows up on a shocker he wrote five years ago, discussed here.
He described the skewed incentives and thus excessive costs caused by our fee-for-service payment model,
gradually being phased out thanks largely to an outcomes-and-quality-based model mandated by Obamacare.
Thanks, Dr. Gawande, for giving us new hope!
top
|
| |

BANIA
April, 2015 --
Here is the actual survey referenced by my earlier blog, HIMSS and HERSS. Entitled 2015 HIMSS Impact of the Informatics Nurse Survey, it concludes that informatics nurses are useful.
We are also organized! Here in the San Francisco Bay Area, we are starting up the Bay Area Nursing Informatics Association (BANIA), our local chapter of the national American Nursing Informatics Association (ANIA).
Join us!
top
|
| |
|
World domination

April, 2015 --
At HIMSS15 I saw
world domination and this is what it looks like: the biggest trade show booth
you ever saw! Seemed like acres! Why is that scary?
top
|
| |

HIMSS and HERSS
April 15, 2015 --
My newest nurse hero: Patricia Sengstack DNP, RN-BC, CPHIMS. At HIMSS15 in a presentation
(like me, Patty was in the audience) about Continuity of Care, we were shown a diagram of the organizational structure that implements it.
The box labeled Management Team contained only CMO/CMIO. That�s code for "doctors run the show." Oh my!
Patty leapt in: "Excuse me, please attend Informatics 101: you need CNO/CNIO in that box, too!"
There is no excuse for omitting RNs from the IT implementation teams for EMRs and other tech that impacts our work.
It is indeed Informatics 101... And so many have yet to learn it.
There�s plenty of supporting evidence, for example regarding a hot topic today, population health:
a survey
showed that some people think that nurses are actually useful when implementing HIT.
"60 percent of respondents feel that informatics nurses play a key role..." Nurses are useful? Who knew?
But what about those other 40%? What are those folks thinking? Have they ever met a nurse? How about a nurse informaticist?
We in this job role must be from Mars. Can we trust this report? After all, nobody uses EMRs more than do nurses... Not even close.
Do you suppose heavy usage entitles us to claim some expertise? Might we possibly be what these C-level folks
call stakeholders?
Hello, world? Listen to Patty!
top
|
| |

HIMSS15
April 14, 2015 --
I spent a fascinating week in Chicago attending HIMSS15, a healthcare technology show.
There were 38,000 of us; the scale was immense. And so are the dollars in this industry.
Each day ended with a parade of black Escalades ferrying the assorted C-level types from the convention center to their hotel suites.
Is this what -- in healthcare -- we have become? Is it what we want to be?
Among the Armani suits were health insurance executives.
Bruce Broussard, CEO of Humana was one of the keynote speakers.
He talked about "responding to consumers� wants and needs."
Evidently, insurance people must create the illusion that they add value.
The first fallacy is that their relationship with patients is -- by definition -- anything but adversarial.
They do their job "best" when they deny care, because the constituency they serve is not actually patients.
Humana is a corporation; its primary purpose is to serve -- again, by definition -- its stockholders.
There is nothing wrong with that; it�s how capitalism works. Why pretend otherwise?
The second fallacy is that patients are the consumers.
The definition of a consumer is one who makes a purchasing decision; one who is the target of advertising and sales.
In health care, that�s mostly doctors. The doctor chooses the drugs, the treatments, the procedures.
It�s mostly the doctors who are wooed by pharma and device manufacturers.
A tiny portion of those advertisements are patient-directed (and some would argue that this shouldn�t be permitted) e.g. sleeping pill ads on TV.
Let's not pretend that patients are more than pawns in a high-stakes game played between medical vendors, payers, and the real consumers.
Broussard arrived by private jet.
He describes Humana as "one of the nation�s largest health and well-being companies."
He is a master of euphemism. Indeed, his entire industry is. Do they add value? Quite the opposite!
But I guess this doublethink enables them to sleep at night.
He showed us some slick, highly-produced videos of happy Humana customers, and recited drivel -- larded with folksy homilies --
about making consumers happy and healthy, some self-serving statistics about excess care delivery (we overspend on all our lucky customers),
the ineptitude of Federal programs (only private companies like ours are capable of delivering decent care),
and litanies -- now de rigeur -- about the need for change. All delivered with conviction and stage management, supremely polished.
No mention of his bloated paycheck. Despite lots of brave talk about embracing
change, that is surely the thing he wants least.
More than ever, it�s clear to me that these parasites must go. They add no value.
They are blood suckers, singing love songs while we bleed. Single payer is the only way forward.
top
|
| |

Patient-centric?
April, 2015 --
We speak of being patient-centric and of patient engagement but still fail to give the patient control of their data. The provider institutions remain in control and responsible for stewardship of the data. Incentives for silo-ing remain in place.
Meaningful use mandates some data sharing but vendors and providers do this only begrudgingly. The value to patients of "portals" could be much better but the incentives are not there for those in our community who create them. For example, as a patient I have not seen even a single provider portal that would tell me what some service would cost. Nor has any patient portal ever asked me whom I might want to withhold any of my data from or disclose it to. We are a long way from being patient-centric.
To be fair, these shortcomings are not the fault of the system developers nor even of the health care providers.
Rather, it is the financial incentives here in the USA that force them to be counterproductive.
The Meaningful Use features of the Affordable Care Act will soon require providers and developers to share some small portions of their data with each other and with patients but we are a long way from giving patients control.
All this talk of being patient-centric is hot air. Only Meaningful Use Stage 3 will cause that to change. Money is the driver in every system but few channel it as perversely as we do. Big pharma, insurance companies, doctors, hospitals, labs and other ancillary service providers make money by selling products and services -- the more and the more complex the better. Our health care system does not exist primarily to serve patients, and the new legislation does only slightly more than nothing to improve that. Too bad for America!
top
|
| |

We've
come
a
long
way...
April, 2015 --
Check out the "Aristocrat of Uniforms" (what the well-dressed nurse wore in the 1920s) at UCSF's archive.
Very elegant but I'll stick with my scrubs, thank you!

top
|
| |

Pepsi Apples
April, 2015 --
"Dean Mozaffarian," writes pundit Jason Clark, "is a well known nutritionist and Dean of the Friedman School at Tufts.
He proposes taxes on unhealthful foods and drink and subsidies on the healthful ones: Should we tax unhealthy foods?"
Jason continues,
Trouble is, I don't think he goes far enough in his analysis. I have no problem with 5 cent apples (though that would require planting a lot more apple trees, which would cut into grain production),
but I think 25 cent salmon filets would be detrimental to the environment. Fish is not a sustainable major protein source for 7 billion people, and there are problems with farmed salmon (e.g. dioxin).
While salmon is no doubt more healthful than red meat, there is probably contamination, and it is environmentally a non-starter.
Why can't the 'big thinkers' truly consider the big picture? A world of 7 billion needs to subsist on unrefined grain, vegetables, and smaller amounts of fruit,
beans, nuts, seeds, etc. Animal products should not be subsidized and should be eaten much less or not at all. Clearly, Mozaffarian feels he needs to appeal to the 'flesh lobby', even if it's fish.
He doesn't answer the question of why apples often cost more than hamburgers in America. Clearly, meat is subsidized, while generating tremendous external costs borne by the environment and healthcare.
We wholeheartedly agree.
top
|
| |

Counting
January 30, 2015 --
Last night from 7 pm until almost midnight, with one of several dozen teams of three
volunteers, I traveled every block in a prescribed area of the Mission District
for San Francisco's annual
point-in-time homeless count.
We need a census of these folks not only to grasp the magnitude of
that population but also for federal funding for programs that
provide assistance allocated on a per-capita basis.
Most major American cities conduct these studies but San Francisco is
one of few that does so almost entirely by volunteer workers.
I am proud of my City and how we care about and for all our residents,
even those who sleep on streets and in parks.
In the approximately 30-block area our team covered, we spotted fifteen
people in sleeping bags or blankets on sidewalks, under staircases,
or in makeshift shelters in parking lots. That's fifteen too many,
but it's a start.
top
|
| |

New
Guy
January 15, 2015 --
In the 70s and 80s, UCSF was a leader in Medical Informatics. My department there, called Section on Medical Information Science, did groundbreaking work.
For example, my master's thesis was an electronic medical record -- one of the first -- that I developed from the ground up, and deployed and tested in a live setting, UCSF's Dermatology Clinic.
It worked fine!
Perhaps the most important work being done in our Section at that time was the development of medical terminologies, lead by our Chairman, Dr. Marsden Scott Blois. With his passing in 1988, our Section lost its funding that had come primarily from the National Library of Medicine. Many of our faculty and graduates defected to Stanford where a growing bioinformatics department picked up the leadership ball.
Today's news signals new hope for retaking our rightful leadership position. With the hiring of Dr. Butte (pronounced "beaut" as in "beautiful") and the reconstitution of our Section under the name "Institute for Computational Health Sciences," UCSF stands to resume its premier position in this area.
My concern is that amid the flurry of buzzwords -- "big data", "bioinformatics", "genomics", "precision medicine" -- we not lose sight of the central part of our mandate, clinical care.
An essential tool for clinical care is the electronic medical record.
Though in the last few years (driven especially by the incentives of Obamacare's Meaningful Use) this technology has become widely deployed, we are still not very good it.
It is not mature. There is much work that remains to be done, and it is my fervent hope that much of it will be done at UCSF.
I mentioned this when I recently met with Dr. Butte. He agreed. This could be the "re-dawning" of an important era at UCSF. Welcome Dr. Butte!
top
|
| |

Project
Homeless
Connect
57
December 17, 2014 --
Our 57th Project Homeless Connect event.
As always, we provided an amazing range of services.
I was part of the nursing team, taking vital signs, triaging, interviewing and diagnosing.
A lot of suffering. Some very, very sick people. Sometimes shocking, always sobering.
My photo is of Gavin Newsom rallying the "troops".
top
|
| |

Supes
vs
soda
December 10, 2014 --
Tonight we celebrated our near-victory in San Francisco over Big Soda.
(I have blogged about the battle
here,
here,
here,
here and
here.)
Spending $3 for each yes vote, we actually got a majority -- 56% -- versus the $100 that Big Soda spent for each no vote.
Alas, because it was to have been a targeted tax (a quirk in our City's electoral system) 66% was required.
I do believe that it is an appropriate role for government to protect citizens from threats both external (national security) and internal (e.g. high-risk behaviors).
Libertarians would likely agree with the former but not the latter... until it regards something they need, e.g. clean air and water, safe products, etc.
Sweetened drinks are not a safe product.
So how does government do this?
- Laws (e.g. seat belts -- thoroughly proven to save lives)
- Education (e.g. sex ed in schools -- thoroughly proven to reduce risky behaviors)
- Taxation (e.g. tobacco taxes reduce smoking thus saves lives)
I do have some intelligent friends who nonetheless opposed Prop. E calling it an overreach of the nanny state.
I disagree.
Taxing sweetened drinks would function as do tobacco taxes and tobacco education in schools.
It is the right thing to do!
Present at our celebration and spearheading the effort to pass this innovative legislation were
(L to R in my photo) Supervisors Malia Cohen, Eric Mar, and Scott Wiener. How often can we say we are
truly proud of our leadership?
top
|
| |

23
and
Anne
December 9, 2014 --
I have lots of heroes. My newest is Anne Wojcicki, one of the panelists at the
Technology Advisory Group meeting I attended today.
She is the co-founder and CEO of 23andMe,
the company that, for $99, will sequence your DNA from a saliva sample
and would (if it were permitted) tell you a lot about your genetics,
your ancestry, and predispositions for a variety of traits and conditions.
Alas, the FDA shut them down citing the potential for inaccurate results.
The main problem is a regulatory system that cannot keep pace with innovation.
By definition, regulators are a step behind and in cases like this one it is to our detriment.
We do need regulation to keep us safe from snake oil but the delicate balance between that and
new technology sometimes eludes us. As Ms. Wojcicki explained it, each of the genes for
which her company tests is considered by FDA rules to be a distinct diagnostic product.
23andMe would have had to apply for literally millions of product licenses.
Instead they went belly-up.
When it was still in business, 23andMe sold a commoditized version of the precision medicine
Sam Hawgood (see below) talked about. Indeed, Ms. Wojcicki's vision was to liberate genetics from the
research lab and create a consumer revolution. "Who owns the data?" she asked.
This would have enabled us each to possess our own.
Another obstacle was the all too familiar one of reimbursements.
Though genetic information has the potential to make health care more effective, insurers will not
reimburse for tests like these. Like the regulators, they are behind the times and the quality
of our health outcomes suffers as a result. Ms. Wojcicki quoted an MD at a conference: "The
biggest problem with 23andMe is you generate non-billable questions."
How do we get regulation and reimbursement to catch up with technology and with the public good?
Perhaps nobody knows the complete answer but some good people are working on it. Go Anne!
top
|
| |

Pride
and
precision
December 9, 2014 --
Today I attended a UCSF event named Technology Advisory Group.
It was chaired by Sam Hawgood, our new Chancellor.
He touted precision medicine,
an area of research (and eventually a strategy for delivering healthcare) that is genomics-based.
UCSF is a leader in this research.
What is precision medicine?
My simplistic understanding is that the effectiveness of certain treatments -- especially in oncology --
is in large part determined by our genetics.
Precision medicine would take a patient's genetic predispositions into account, for example, when planning a course of chemotherapy.
I'm proud of the industry-leading research at my alma mater!
top
|
| |

Playing
with FHIR
November 2014 --
One of the things I learned at AMIA's 2014 conference is that a thing named
FHIR will change the way we do computing in healthcare.
Much of the communication that is done between the numerous and disparate software systems that run our hospitals, labs, clinics, payers, etc., etc.
is via an antique and under-powered standard named Health Level 7 (HL7).
Standardized communication protocols were a breakthrough in their day but that day was decades ago.
FHIR is HL7's effort to remain relevant. It just may work.
Today's massive, monolithic, and preposterously expensive EMRs and EHRs will, they claim, with time become relegated to commodity products serving as backend
servers of medical and financial data, living in server farms in basements or even in the cloud.
The front ends (the part users see) will be small, cheap, easily-deployed (and replaced) apps.
Everybody is talking about apps.
Modularity in healthcare software has been predicted for many years yet no one has been able to make it work.
The contrarian view -- and it is thus far proven by practice -- is that the data and the workflows are just too complex, and
that's why our only choice is the fabulously complex and expensive software monstrosities of today.
Who is right? Only time will tell.
By the way, one of HL7's inventors back in the 1970s and 1980s was my UCSF grad school professor
Dr. Don Simborg. Go Don! Go FHIR!
top
|
| |

AMIA!
November 19, 2014 --
Today was the last day of the American Medical Informatics Association's 2014 conference in Washington, DC.
I learned a lot, grew professionally, enjoyed seeing what everybody else is working on and talking about what I'm working on,
and shook a lot of hands.

Among them were legends in the field of Nursing Informatics Drs. Virginia Saba and Kathleen McCormick.
Here are their autographs.
top
|
| |

Et tu,
RNs?
November 8, 2014 --
Usually the level-headed ones, now it seems even we nurses are infected by Ebola frenzy. Unlike the ignoramuses of fearmongering Fox News and its ilk, we should know better. Kaiser nurses are actually planning a strike! Nov. 12. Are Sutter nurses, too, planning anything like this?
If we really want to do what's right for our patients we wouldn't waste nursing resources on a crisis that doesn't exist. We'd wash our hands more. Things like MRSA and C-diff are real and they kill lots of people. And tens of thousands die of the flu every year. Let's urge our patients to get their shots. Half of America can't be bothered. Yet they obsess about Ebola.
Et tu, RNs? Say it isn't so!
top
|
| |

Wise
Cutting
October, 2014 --
I recently read and thoroughly enjoyed Dr. Abraham Verghese's 2009 bestseller Cutting for Stone. "Cutting", of course, is the slang surgeons use to describe their work.
Ethiopian-born and today practising at Stanford, Verghese shares much wisdom.
For example, he recites surgery's Eleventh Commandment:
Thou shalt not operate on the day of a patient's death.
Much to think about. Much that's profound.
top
|
| |

Talking
Sense
October 23, 2014 --
A rare voice of reason on Ebola is that of Dr. Paul Farmer,
a physician from Massachusetts, recently returned from Liberia.
Here
he's interviewed by Audie Cornish on NPR.
And here is his diary in the London Review of Books.
Both are highly recommended.
The main takeaway is that Ebola needn't be nearly as deadly as it's been thus far;
inadequate health systems are to blame.
As with cholera and other hemorrhagic infectious diseases, many or even most deaths could
be prevented by access to ORT (oral rehydration therapy).
Of course, the story is not that simple, but it's an important one.
Thank you, Dr. Farmer, for telling it, and for talking sense amidst the babble.
top
|
| |

Lava
Mae
October 23, 2014 --
Today I volunteered with the
Lava Mae
team and their shower bus.
The name is a play on the Spanish words for "wash me".
San Francisco donated an obsolete-but-serviceable city bus and
Lava Mae fundraised the $75,000 it cost to convert it to a pair of showers on wheels.
Three days a week, the bus is parked in places where homeless people congregate.
For many, it provides a rare opportunity to get cleaned up and feel human again.
During the course of a five-hour shift, 40 or 50 people shower -- privacy,
lots of hot water, castille soap, fresh towels, and friendly folks.
Sometimes the streets of San Francisco are not so harsh after all.
top
|
| |

Hey
Obama
October 10, 2014 --
President Obama came to San Francisco today on one of his fund-raising tours.
We let him know
what we want. In no uncertain terms!
top
|
| |

Schmebola
October 3, 2014 --
Laurie Garrett is not the only one drumming up Ebola hysteria.
Even less rational is the drumbeat from the right-wing fear-mongers.
Stephen Colbert has collected clips of insane "reporting" by Fox.
Fortunately, there are a few voices of sanity.
Here is an article in which Liz Szabo sums up America�s overreaction to Ebola.
top
|
| |

New
Vectors
September 29, 2014 --
My friend Jason Clark observes that corporate profits continue to trump human health and wellbeing.
He writes:
Poor diet is now responsible for a greater burden of disease than smoking, at least in America.
Food companies must be controlled much as tobacco companies have been.
See Collaboration with the New Vectors of Disease
that points out that the food industry "...may require tobacco industry-style regulation."
Banks must be controlled as well, so that we don't get a repeat of 2008 -- but I think Obama missed his chance to regulate the banks in 2009,
and another financial calamity is in the cards.
The last five years have been a gigantic lesson in moral hazard,
whether in the USA or in Europe Union, the UK, or Japan. Central banks covered up the mistakes and fraud.
Energy use and extraction must be controlled if we are to prevent catastrophic global warming (+6℃) by the year 2100.
Yet we have been moving in the wrong direction, and public skepticism in the US has actually been growing
(probably due to the efforts of right wing think tanks and spending by Koch Bros. and their ilk).
So while we won the war against the tobacco companies (mostly because we didn't need to smoke),
the fight against Big Food, Big Banks, and Big Energy is harder because these are less discretionary.
Tobacco may be addicting for its users, but food, money, and energy are primary to any civilization.
Good luck with the soda tax.
top
|
| |

Teachers
September, 2014 --
Dying, my friend Heather taught me so much. I am a nurse, trained, licensed, and full of technical knowledge. I have accompanied patients toward the next world, and supported their failing, disfigured bodies en route. I know something about the inevitable sequence of events, the takeaways, the suffering.
About her cancer, Heather asked, "Is it serious?" What she wanted to hear was, "No, you'll get over it. You'll be fine." Being truthful, I said, "Yes." I wanted to add, "But there are things we can do to improve the situation." But she had already hung up the phone.
What did she teach me? The power of denial. When it's you, I can talk about it all day long. But when it's me, change the subject. I'm not going there. You can't make me. No one can make me.
The death spiral can be handled like so many others -- addiction, alcohol, violence -- spinning downward with eyes shut tight. I can be swallowed by it yet refuse to look at it. Of course, denial is one of Kubler-Ross's famous phases: "F* you, f* you all, f* the world, this isn't happening."
My father's passing in 2006 taught me a lot, too. He made it to the anger phase, or perhaps it was bargaining... Kubler-Ross is helpful but not the whole story. On his last day he said, "But I have so many projects yet to do." He was good at so many things; so much skill, wisdom, and passion for art, politics and people. All that is gone now.
My best buddy Mike on his own death bed got fully down the Kubler-Ross trajectory, all the way to the acceptance phase. He supported us around him who were falling apart, filled with grief at his impending departure. "It is what it is," he taught us.
Each died in their own way. Each taught a lesson I'll never forget.
top
|
| |

Ebola
Gates
September 10, 2014 --
The Bill and Melinda Gates Foundation today announced its commitment of $50 million to support the emergency response to Ebola. At last, we are starting to see the resources this crisis demands.
Obama sought $88 million but yesterday House Republicans slashed Obama's requested Ebola funding by more than half.
What is needed for an appropriate response? In an article today entitled Ebola Then and Now, Drs. Breman and Johnson in the NEJM say,
...the main priorities should be adequate staff for rigorous identification, surveillance, and care of patients and primary contacts; strict isolation of patients; good clinical care; and rapid, culturally sensitive disposal of infectious cadavers... We also await key virologic, clinical, epidemiologic, and anthropologic descriptions of the epidemic.
We hope that this money from Gates and whatever slips past the Washington partisans will make these things happen.
top
|
| |

Ebola
death
September 3, 2014 --
We have seen another tragic death of a healthcare worker in Liberia, Dr. Sam Brisbane, the Emergency Department chief in the only Monrovia hospital that accepts Ebola patients.
The doctors and nurses are paying the ultimate price.
In another heart-wrenching NEJM article, A Good Death -- Ebola and Sacrifice
the authors debate the limits of their "duty of care toward their patients."
And here (Sept. 5) is another story, A
Diplomat Infects A Doctor As Ebola Spreads In Nigeria.
The diplomat violated a quarantine order and now "[authorities are] not optimistic about the Nigerians' ability to contain Ebola as it spreads beyond Lagos."
You can track the spread of this and other diseases on Healthmap,
a global disease-tracking service directed by epidemiologist John Brownstein of Harvard University.
Here is their tracking of ebola.
Press the Play button to see how the disease has progressed numerically and geographically over recent months.
top
|
| |

Corporate
genetics
August 29, 2014 --
If you're not already a vegetarian, you've probably at least considered it.
One of many reasons is ethical, both for the animal treatment and for the industrial genetics, controlled by just a few corporate giants.
Here's a way to eat eggs and chicken (and help propel a movement) that's more friendly to the environment, to the animals, and to our
bodies. It's described in today's National Geographic:
Open-Sourcing Chicken: Breaking Free from Corporate Genetics by Maryn McKenna.
It's part of community-supported agriculture.
My family has enjoyed Eatwell Farm's weekly food basket for years.
Pictured above is Eatwell's proprietor, Nigel Walker.
Consider his basket (delivered in San Francisco) for your own household, and
the crowdfunding campaign for the planet.
top
|
| |

A
nurse
hero
August 29, 2014 --
The Ebola crisis worsens. Hopes for at least one vaccine (from a San Diego company) are dwindling.
The number of reported cases exceeds 3,500.
More than 1,900 have died in Guinea, Liberia, Nigeria and Sierra Leone.
Senegal reported its first confirmed case today.
"The current outbreak is in both the anglophone and francophone countries,
with associated transmission risk implications," writes epidemiologist Pat Olson MD.
"This is the only disease I'm aware of historically where the caregivers are specifically
identified as those at highest risk."
HuffPo: "Deaths Of Ebola Researchers Underscore Urgency Of Their Mission".
One of the heroes is RN Anja Wolz, author of Face to Face with Ebola -- An Emergency Care Center in Sierra Leone in NEJM.
She volunteers as a nurse and emergency coordinator for the M�decins sans Fronti�res (MSF -- Doctors Without Borders).
She writes,
Everyone working in the isolation area must follow the protocols and procedures to the letter... one mistake could be deadly.
She continues, The new patients sometimes arrive eight to an ambulance...
We've given the ambulance drivers basic PPE (personal protective equipment) to distribute to patients, but they're afraid to get close enough to hand it out...
The global health community has taken a long time to react... We need to be one step ahead of this outbreak, but right now we are five steps behind.
top
|
| |

Talking
soda
tax
August, 2014 --
Last weekend I helped staff a sidewalk table at a farmer's market.
We harangued the passersby. Some brushed us off.
Most were polite and surprisingly well-informed on nutrition.
For those who weren't, here were our talking points.
Health Issues
- Soda is the largest source of sugar in the American diet.
- Liquid sweeteners disrupt bodily metabolism. The liver processes them differently than it does solid sugars. Eventually this leads to diabetes.
- We have an epidemic of diabetes.
Legislative Issues
- Purposes of the tax:
1. Reduce consumption,
2. Raise $31M (est.)
- Use of funds (earmarks):
25% public health
40% school district
25% parks and rec
10% special projects related to nutrition education, PE classes, etc.
- Only drinks with added sweeteners are taxed. Not fruit juices.
- The tax will be collected at distribution, not at retail sales, so grocery stores will be unaffected.
Election Issues
- It's a "special" tax -- earmarked, not for the general fund. We know exactly how it will be spent.
- Special taxes require 66% of the vote, not just 50%+1
- Our opponent, the Coalition for an Affordable City, is funded entirely by the
American Beverage Association. Their canvassers and operatives are paid. Ours are volunteers.
- The argument that this is a regressive tax ignores the fact that diabetes is a regressive disease.
Both soda advertising and sales and diabetes are concentrated in low-income neighborhoods.
top
|
| |

Ebola
hysteria
August 14, 2014 -- (an open letter) --
I'm disappointed, Laurie Garrett! As a Pulitzer prizewinning journalist and one I have heard and respected on NPR (and a fellow UCSC alumna, too) you appear now to resort to crass sensationalism.
In an article entitled You Are Not Nearly Scared Enough About Ebola
in Foreign Policy's online magazine, you write things like, "Wake up, fools."
That is inflammatory language and does not befit serious journalism.
Worse, you appear to conflate (surely on purpose; you are too smart not to know the difference) the severity with the communicability of a disease.
Even Fox News takes a more reasoned approach to this topic (Gutfield: Stop the Ebola Hysteria).
Here's what the experts say about Ebola:
While it's true that the majority of those who catch Ebola die, it's also true that it's hard to catch.
The period during which the disease is communicable is
while the patient is actively symptomatic and postmortem (the big problem with funerary rites).
These are not times during which the patient is likely to travel or even get out of bed.
It doesn't have a long, silent incubation like, say, AIDS; recent evidence shows it to be three weeks.
It's not airborne. It's communicated only by direct contact with body fluids.
Reading your article carefully, I see that it doesn't actually contradict these facts.
However, its tone is sensationalist or worse. Is your intent to frighten?
I am surprised to see you stoop so, and the same for Foreign Policy,
though evidently its mission is to "question commonplace views"
(see Wikipedia)
and, I guess, provoke debate. But this is irresponsible.
Please cool the rhetoric. Stick to the facts.
The crisis is real but creating panic does no one any good.
top
|
| |

A garden
to tend
August 2014 --
I recently read Dr. Victoria Sweet's 2012 recounting of her twenty years at San Francisco's venerable
Laguna Honda rehabilitation center,
recently transformed from almshouse (the last one in America) to hospital.
Her book is entitled God's
Hotel, and subtitled, "A Doctor, a Hospital, and a Pilgrimage to the Heart of Medicine".
The New York Times entitled its review, A Hospital That Gave Its Patients Time to Heal.
It's a fascinating concept, rare in today's healthcare system in which the body is an engine to repair...
As quickly as possible, and at the lowest cost.
Dr. Sweet suggests that -- just as an almshouse is an old and alas discredited model -- an old metaphor,
similarly worthy of revival, is of the body as a garden to tend.
She calls it slow medicine.
Almshouses and gardens lovingly and patiently tended... Dr. Sweet gives us pause.
top
|
| |

Medicare
for
all
July 2014 --
Another hero! Michigan's Congressman John Conyers has reintroduced
House of Representatives Bill HR 676, known as Medicare for All.
It would establish a long-overdue single-payer healthcare system in this country, along with several more much-needed reforms.
Its chances of passage? Zero. But it is the right thing to do. We mustn't give up. Go Rep. Conyers!
top
|
| |

Back
in
the
saddle
July 2014 --
For three days in mid-July, I shadowed an RN in Kaiser's Richmond, CA Emergency Department (ED).
Having done my RN preceptorship in another Kaiser ED (South San Francisco), it was good to be back in the saddle.
Emergency Departments serve a variety of unique purposes in our complex healthcare system.
Here are a couple of observations about that.
-
The ED is an essential portal to the hospital, admitting more than half of its inpatients.
Thus, its diagnostic and triage functions must be finely honed.
It serves as a gatekeeper for services that are often hugely expensive.
Decisions are made here that are both medically and economically impactful.
-
It is the only place in our healthcare system that is obliged to deliver care without regard to a patient's ability to pay.
This is mandated by the Federal 1986 Emergency Medical Treatment & Labor Act (EMTALA) Act.
As a result, the ED often serves as the sole provider of primary care for the medically indigent.
These are onerous demands yet at Richmond Kaiser they are skillfully performed day after day.
Thank you, Kaiser, for another excellent experience!
top
|
| |

Astro
Truth
July 2014 --
We are grateful to our San Francisco Supervisor Scott Wiener for District 8, where I live.
He is a staunch supporter of the proposed "soda tax" about which I have written
here, here and here.
Thanks to his support, this proposal will be on November's ballot in our enlightened City.
 Meanwhile, our opponent -- Big Soda -- is mounting a deceptive yet well-funded "astroturf" (pseudo-grassroots) campaign decrying the high cost of living here.
Taxing sweetened drinks, they say, makes our City even more expensive.
Their brochure's headline is about high housing costs, a real problem, but has nothing to do with the poisons they sell to our children.
Meanwhile, our opponent -- Big Soda -- is mounting a deceptive yet well-funded "astroturf" (pseudo-grassroots) campaign decrying the high cost of living here.
Taxing sweetened drinks, they say, makes our City even more expensive.
Their brochure's headline is about high housing costs, a real problem, but has nothing to do with the poisons they sell to our children.
More than half of the metabolism-disrupting sugars ingested by children come from sweetened drinks.
Regarding the high cost of the lifetimes of diabetes these products cause they are deathly silent.
Thank you, Supervisor Wiener, for telling the truth despite the astroturf.
top
|
| |
Health news
July 15, 2014 --
Today I attended a tour of the newsroom of our local paper, the
San Francisco Chronicle.
 It was wonderful to see -- live and in person -- the celebrity columnists we've been reading for all these years.
(If only we could resurrect Herb Caen.)
We also saw the news team decide what would be in tomorrow's paper... and tomorrow there it will be!
It was wonderful to see -- live and in person -- the celebrity columnists we've been reading for all these years.
(If only we could resurrect Herb Caen.)
We also saw the news team decide what would be in tomorrow's paper... and tomorrow there it will be!
For the purposes of this blog, I'd like to point out the Chronicle's excellent, weekly
Health section --
"exclusive, comprehensive coverage of health and medicine news, medical developments and studies,
biotechnology, genetics, diet, fitness, and exercise trends."
Go Chron!
top
|
| |

Meaningful Use
Phase 2
July 2014 --
As the second phase of the Meaningful Use (MU) section of the Affordable Care Act (ACA) kicks in,
we may at last be bringing under control one of the major culprits for the high cost of health care.
MU Phase 2 is doing this by shifting from fee-for-service to pay-for-quality reimbursement models.
Background:
- Meaningful Use is described here.
- The skewed incentives (and thus excessive costs) caused by fee-for-service are described here.
- The effect of these problems is described in a beautifully-written New Yorker story by Dr. Atul Gawande,
The Cost Conundrum.
One of ACA's promises is to control health care costs. That promise is starting to bear fruit now. We are watching!
top
|
| |

Save
VistA
July 2, 2014 --
I have written about VistA before, and it's time to revisit it,
prompted by Paul Berlin's The
VA Waitlist Fiasco: VistA should not be thrown out with the bathwater.
See also Mr.
Longman's testimony before Congress (linked in Mr. Berlin's article) that faults not the quality of the
health care provided by the VA but rather the barriers to access to it.
Similarly, the VA's VistA EHR deserves none of the blame game being played by opportunistic media and cynical politicians.
On the contrary, the rest of the Health Information Technology (HIT) industry would do well
-- indeed should be obliged by legislation and thoughtfully-crafted financial incentives -- to follow VistA's example.
This would include respecting and implementing data-sharing standards
(rather than the silos created and defended by self-serving vendors) and the
software quality and longevity that can happen when computer code is open-sourced.
VistA has done these things and should be held up as a model for the rest of the industry,
not, as Mr. Berlin quips, "thrown out with the bathwater."
This is an important message and I hope the buyers and decision-makers don't just
blindly make the "safe" choices as, decades ago, it was said that,
"You won't get fired for buying IBM." Where did that get us?
top
|
| |

Apple
Health
July 1, 2014 --
Last month Apple announced its inevitable foray into the healthcare arena.
It's a market too big to ignore.
The first product is Healthkit.
The visible part of Apple's strategy is on the consumer side.
This side is perplexing; a few years ago I thought that Google Health would be a winner
but it fizzled.
Will Apple succeed where Google, Microsoft, and others haven�t?
Joseph Kvedar of Connected Health offers an interesting perspective,
My Wish List for Apple�s HealthKit Initiative.
He says that Apple's strength is design and its weakness is analytics.
Both are necessary to thrive in this market; Apple's success is not guaranteed.
Another question regards the provider side.
Most of the doctors and nurses I know use iOS not Android (but this is anecdotal only -- no flames, please!)
What I�d like to know is, what are Apple�s plans for this audience?
I have worked on a product for the provider side, gambling on iOS as the platform of choice, and have built
NurseMind, an iOS-based checklist app for nurses.
It is a standalone but would benefit from integration with Epic, Cerner, GE, etc.
Apple could become the user-friendly front-end for us all with a larger ecosystem that supports health data of all types.
My prediction? They�re already working on it.
top
|
| |

Vocabulary 101:
HIT and ACA
June, 2014 --
The Affordable Care Act (ACA) has much to say about healthcare information technology (HIT).
It has spawned a new vocabulary.
Few would dispute the goals of the ACA: quality improvement,
cost reduction, wider inclusion, data sharing, and more.
The buzzwords are patient-centered and value-based.
The ACA also mandates:
- Reduction of hospital readmissions
- Improved access to critical care
- Community and population health
- Patient education and engagement
- Chronic disease management
- Preventive care
- Payment reform
Worthy goals! But how do we get there?
Here is how:
- Meaningful Use -- incentive payments to healthcare organizations (HCOs) to acquire certified electronic health record (EHR) technology, and to implement it in three stages over a period of years with measurable goals including effective patient data capture and sharing
- Rural healthcare -- through loans and grants for facilities and technology especially telemedicine, ACA addresses some needs of a long-neglected population
- Behavioral health -- community mental health centers, psychiatric hospitals, clinical social workers, and others who treat substance and alcohol abuse, suicide and psychological distress, can benefit from EHRs and HIT
- Strategic planning -- especially coordination of public and private efforts to implement HIT
- Federal and state coordination -- focusing primarily on consistent implementation of privacy and security that at present vary widely among the states
- Clinical decision support (CDS) -- HIT can help clinicians be more effective (though it cannot replace them) through alerts, reminders, guidelines, condition-specific order sets and eventually evidence-based practice (that ACA calls contextually relevant reference information).
- Data sharing (Health Information Exchange, HIE) -- today's data silos -- clinicians, labs, hospitals, pharmacies, health plans, payers and patients -- must have standards, mechanisms and incentives to communicate, and governance to enable and regulate this across geographic and organizational boundaries so that information can safely follow patients to wherever it is needed
- Consumer eHealth -- provide access to data by patients themselves, empowerment to take action and gain control over their health
- Patient safety -- HIT has risks as well as benefits; mitigate them and prevent patient harm
- Long-term and post-acute care -- the care of patients in these settings, especially elders, is often complicated by co-morbidities and multiple caregivers; policy can support development and implementation of HIT to support such care.
For any practitioner of HIT, this is essential vocabulary.
top
|
| |

End employer-provided
May 1, 2014 --
Why is your health insurance provided by your job?
Why not just buy it yourself?
The usual claim is that it's a perk that employees appreciate.
But the real reason is that companies can deduct it from pre-tax income and individuals cannot.
Why do we have this crazy system?
It is the outcome of some terrible compromises made 60 years ago, especially the 1954 decision to make employment-based health coverage tax deductible for businesses.
(See e.g. this Health Policy Brief).
Today's New York Times article, Envisioning the End of Employer-Provided Health Plans by Neil Irwin asks, "Why should quitting a job also mean you have to get a new health insurance plan? Why should your boss get to decide what options you have and negotiate the cost of them? Employers don't get to select our auto insurance or mortgage company, so why should health insurance be any different?"
Indeed. Now that the ACA has given us health insurance exchanges from which no one can be turned away,
and subsidies for those who could not otherwise afford it, there remains only one reason to continue the present system: that tax deduction.
My opinion? Rescind this. Instead, make health insurance premiums deductible by individuals rather than by businesses.
Make people buy their own insurance rather than tying it to their jobs.
This would be popular. Paychecks could be increased by the amount of the employers' healthcare savings.
So I offer a modest proposal: let companies pay their employees what they would have spent on health insurance
(fatter paychecks!) and let every American deduct from their pre-tax income whatever they spend on health care.
The net change in revenue to the government will be zero.
The net change in costs to companies will be zero.
Employee mobility and choice will be enhanced.
Problem solved.
top
|
| |

ACA
in real life
April 16, 2014 --
This ACA thing is tricky.
For many people, signing up is not so simple.
Here is a fascinating account of the issues as experienced in real life:
In Their Own Words: Consumers� and Enrollment Counselors� Experiences with Covered California, a survey released today by the California Healthcare Foundation.
Here in San Francisco we are having an interesting time with the ACA in real life, too.
My friend M. ran a couple of sign-up sessions.
She says,
[We] signed up J. [who] worked at [employer X] for 30+ years and was laid off. She had Cobra then her ex-husband insured her for awhile then she was a self pay. Once the ACA came into being, J. met with [us and we] signed her up!
[We] also signed up our bartender L. and her husband. L.'s husband is a taxi driver and neither of them had insurance. And now they do!
Of herself, M. writes,
I have insurance through the ACA.
I was not eligible for "regular" insurance because of a pre-existing condition
and had to get my insurance through MRMIP (Major Risk Medical Insurance Plan)
and paid almost $800 per month.
When the ACA became available, I might have been the first in line!
My insurance now has no limits and while I am paying $666 per month,
it is less than $800 so I am happy!
The successes speak for themselves.
Let's hope the voters are listening!
top
|
| |

Go
San Francisco
April 16, 2014 --
Today I attended a hearing at the Board of Supervisors of the City and County of San Francisco, my home town.
The topic of the hearing was
a proposed new tax of $0.02/oz of sweetened beverages.
As one of several dozen who expressed their viewpoints on this proposal, I spoke as a nurse, parent, and San Franciscan.
Regarding each of those roles, I said what you'd expect:
that health care workers are seeing more diabetes and obesity than ever and sweetened foods are largely to blame;
that we must protect the health of our children;
and how proud I am to be from San Francisco where we lead the nation in forward-thinking public policy.
What shocked me was the number of red-T-shirted proponents of
the opposing side.
Their T-shirts called for "fairness" and their wearers packed the room.
Clearly they had been drilled by "Big Soda", the corporate interests that would be harmed by reduced junk food sales.
I doubt that a single one of these well-indoctrinated flunkies would have been there without some incentive
(to which not one would admit).
The fairness claim speaks volumes to the fact that the science of nutrition is to them a cause that's already lost.
Nonetheless, they have the big dollars to confuse the voters with a barrage of advertisements.
Without that, our inspired legislation would sail through.
But there's still hope.
My fellow San Franciscans are a smart and principled bunch.
I hope they are enough so to not be tricked when the November ballot rolls around.
top
|
| |

New
Model
March 25, 2014 -- A New Financial Model for Nursing
I am a nurse and an informaticist.
Combining these disciplines, my mission is to equip myself and my fellow nurses with the best tools available and also with some that are yet to be created.
However, the existing financial model for nursing presents a large obstacle.
That must change.
The dearth of nurse-centric (my term) tools is discussed in a paper published today, mHealth's great untapped potential: Nurses.
In the context of hospital finance, nurses are seen as a cost center.
Compare this with doctors who "...are considered the revenue-generators and the face of the healthcare institution."
Indeed, most of what nurses do -- administer medications, deliver hygiene, nutrition, education, progress assessments, and regular activities such as charting, health status and vital signs monitoring, ambulations and surveillance -- is not directly billed.
Rather, these services are bundled into the hospital's room rate. From the point of view of accounting, nursing is a cost and rarely a revenue generator.
Thus, there is little incentive to equip us with the tools that would make us more effective.
Instead, workflow improvements focus on making us more efficient.
In other words, the "successful" hospital gets nursing done for as little money as possible.
Yet nursing is essential to health care and, done well, contributes immeasurably to the quality of outcomes.
It's time for the model to change.
Starving us while pushing us to get more done and to work faster can be detrimental to quality.
Hence, I offer a modest proposal.
To drive health care economics to perceive nursing as worthy of investment and redesign, we must become a revenue center.
Here is one way we could do that.
Much as outpatient doctor visits are billed according to a scale of simple, medium, or complex (with fees charged accordingly), the various services that nurses provide should be un-bundled and billed on a similar scale.
For example, some patients require in-bed hygiene care.
They (or their insurance companies) should be charged for it, on a scale of quick, medium, or lengthy.
An obese patient who requires a second nurse or an assistant to position them for a bed bath would incur a higher fee for hygiene service; it is more expensive to deliver.
Nursing activities are usually charted at least briefly in the medical record; this new approach would add a charge generation to an existing recorded item much like, say, a CT scan generates both medical and financial data.
Like airlines that have been able to reduce ticket prices by unbundling (charging extra for) baggage handling, hospitals could reduce room rates by unbundling the nursing services that come with them.
The article states that nurses are "underappreciated... [they] are looked upon as the single largest line item on the balance sheet... hospital IT departments are focused on those and other concerns and leaving nurses to their own devices.
They don't have the time or resources to deal with nurses."
In other words, we nurses often don't get the tools we need because the investment would not repay itself.
It would just add to our cost that is already perceived as high.
This could change.
The quality of nursing -- given incentives to equip us well -- could make a huge leap forward.
It's time for a new financial model for nursing.
top
|
| |

Too
HIPAA
March 24, 2014 --
Why should I care whether anyone knows my immunizations or can see the x-ray image of my broken foot?
I don't care -- help yourself. The truth is that for me and most people, most health care data needn't be kept private.
There's nothing secret or even interesting about it... Except to researchers and to my care givers.
These people should have unfettered access.
Well-intentioned HIPAA safeguards create obstacles that are not justified.
In practice, HIPAA reinforces data silos -- provider institutions that keep my data to themselves
-- that inhibit sharing.
Also, HIPAA grows the mountains of paperwork that they and I must scale whenever care is given.
Certain types of data -- psychological health and substance abuse history,
for example, listed in detail here --
should indeed be protected, with access controlled solely by the patient, but this is a small fraction of health data.
The benefits of sharing data are numerous.
These include the ability to conduct population-wide and epidemiological research.
Famously promoting such access to and uses of this data is
Google co-founder Larry Page who in this TechCrunch piece
proposes that we make all health data public. Go Larry!
top
|
| |

Big soda spending
March 20, 2014 --
Big Soda is fighting back and spending big.
It seeks to defeat San Francisco's pioneering effort
to discourage consumption of sweetened drinks -- conclusively
proven to have bad health effects -- with a tax.
What is it about jobs and faceless corporations that encourages
the suspension of morality? How do the people who work there
feel about defending products that hurt people? There's
something that just switches off in their brains. Remember
Big Tobacco? And the lies they told and evidence they covered up?
Big Soda is following them down the same path, and
spending big to defeat us.
They're buying direct mail, live calls, organizers, consultants, and even
ads on Facebook (some "friends"!)
They have the money; they can confuse voters.
But this is just a skirmish.
Ultimately the truth will be known.
The war is ours to win.
top
|
| |

Who
was
first?
March, 2014 --
I have touted Dr. Atul Gawande and his medical checklists in this blog. But he would be the first to point out that he wasn't the first to apply them to healthcare. That was Dr. Peter Pronovost at Johns Hopkins in 2001. The concept is summarized nicely in this 2009 New York Times article by Robin Henig, A Hospital How-To Guide that Mother Would Love.
However, it was Gawande who applied this method on an international scale, and proved that it works. Henig writes, and quotes from Gawande's Checklist Manfesto:
The study began in the spring of 2008, and the results were startling. Without adding a single piece of equipment or spending an extra dollar, all eight hospitals saw the rate of major postsurgical complications drop by 36 percent in the six months after the checklist was introduced; deaths fell by 47 percent. "In every site, introduction of the checklist had been accompanied by a substantial reduction in complications," he writes. "In seven out of eight, it was a double-digit percentage drop. This thing was real."
The point is that anyone with a complex technical job -- including nurses -- can benefit from this simple intervention. Henig writes:
...the complexities of technology in the 21st century may be best handled by the simplest solution. "We may admit that errors and oversights occur -- even devastating ones," he writes, referring here primarily to his fellow surgeons, a group not known for modesty. "But we believe our jobs are too complicated to reduce to a checklist."
We do so at our own peril or, rather, at the peril of our patients. She concludes:
What a powerful insight this is: In an age of unremitting technological complexity, where the most basic steps are too easy to overlook and where overlooking even one step can have irremediable consequences, something as primitive as... a to-do list to "get the stupid stuff right" can make a profound difference.
Are nurses victims of the same hubris? I am working to prove otherwise.
top
|
| |

How
we
die
March 3, 2014 --
"What is the experience of going though a heart attack? What is that like?" asks Dr. Atul Gawande in
this NPR interview
about Dr. Sherwin Nuland, author of the ground-breaking
How We Die that de-mythologized death.
Nuland died today of prostate cancer at age 83.
Gawande observes that, until recently, medical students weren't taught about death.
"It was a revelation," he says.
"You could be direct with people. You could tell them the truth about what happens while being humane...
what it means to be a good doctor."
Read the book. And applaud these doctors who are making a real difference in how we handle that final phase.
top
|
| |

Big
soda
February 1, 2014 --
Today I attended a rally organized by San Francisco District 10 Supervisor Cohen to urge
a tax on sweetened drinks here in our enlightened City.
Overcoming opposition from a huge and well-heeled industry (billions of dollars worldwide each year)
we're working to pass a $0.02/oz city surcharge on sweetened drinks (sodas, juices, sports drinks, etc.)
As usual, we're ahead of the curve!
We have an epidemic of obesity and diabetes.
Sweetened foods are a direct cause.
Especially for kids, increasing the prices of sweetened drinks would discourage their consumption.
Part of the reason why these foods and drinks are cheap is the Federal subsidy of corn farming.
The sweeteners in sodas and processed foods are made from corn.
If we can't stop the subsidy, let's neutralize it with a tax.
And if we can't do it nationally, let's do it locally.
This can generate $30 million annually to fund physical education and nutrition programs for San Francisco children.
Stop Big Soda! Go San Francisco!
top
|
| |

Politics or health?
January 2014 --
It's hard to believe that some politicians could be so driven by partisan politics that they would deny health care to their citizens rather than collaborate with the opposing party. Yet it's true.
In an unrelenting effort to undermine Obamacare, 25 states have refused expanded Medicaid funding -- funding that would have made health insurance affordable for literally millions more Americans
(here's who's left behind) -- to spite Obama and his health care reform. All 25 have Republican governors. Where are the calls for impeachment? Where is the outrage?
top
|
| |

Disaster
not
January 2014 --
Stop calling the Obamacare technology rollout a disaster! Even Obama parrots that conventional wisdom. If you're a practitioner of technology, you know that it's never like the movies, where everything new and complex works perfectly from the moment it's switched on.
The second meme, also unquestioningly accepted, is that government -- unlike private industry -- just can't seem to "do" technology (unless it's the NSA, I guess.) In fact, complex projects are complex no matter who does them, and buggy software happens in every big project, private or public.
Compounding the technical complexity was a litany of political issues that made www.healthcare.gov's specification a moving target. A difficult project becomes near-impossible when:
- Politics dictates an unrealistic schedule, with not enough time for testing.
- The target was moving -- they didn't even know how many (or which)
states their system had to support (34, as it turned out) until quite late in
the timeline.
- The number and diversity of systems to be integrated was large -- insurance companies, state and federal databases, even the IRS -- and without standards for data exchange.
- There were deliberate sabotage attempts by deep-pocket special interest groups whose tactics included bogus web sites to confuse and frustrate people who sought to sign up.
- Amazingly, the project had no official budget. In an excellent article entitled How political fear was pitted against technical needs, The Washington Post says, the "...most basic reason was financial: Although the statute provided plenty of money to help states build their own insurance exchanges, it included no money for the development of a federal exchange -- and Republicans would block any funding attempts. According to one former administration official, Sebelius simply could not scrounge together enough money."
It's remarkable that it worked at all. Now, with time for testing and debugging, system performance is improving. This is actually a pretty normal technology development and release lifecycle.
This blame game is like somebody letting the air out of your tires and then calling you names because you're having trouble giving them a ride.
Stop using technology as a political football, and -- ahem, Mr. Obama and everyone else -- stop calling it a disaster!
top
PS -- The cartoon is by my Dad. Click it to see it full-size.
|
| |

Wing
nuts
December 18, 2013 --
The right-wing nut jobs at Fox just don't give up.
The drumbeats about Obamacare seem endless.
Yes, Obama's promise that if we like our health insurance policies we could keep them was ill-considered.
He should have added, "...if they satisfy certain minimum requirements."
The surprise was that many didn't.
They were junk and should never have been allowed to be sold;
canceling and replacing them with honest policies is actually
one of the benefits of the Obamacare legislation.
Yes, there are bad parts of this legislation, too, e.g. that it leaves in place the cash-sucking fee-for-service providers and the yet-more-cash-sucking insurance middlemen.
These are discussed in other blog entries here.
It's all in how you spin it, and Fox outspins the White House.
The amazing part is that people fall for it.
But then, they can't spell, either.
top
|
| |

Heroic
senator
December 2013 --
One Senator slogs on in the campaign for single-payer health care: Bernie Sanders (D, VT).
It's inevitable because we cannot continue as we are.
Under this bill we'd have health care for all, reduced costs, and more.
Want the details? Read his American Health Security Act of 2013.
And don't give up hope... Go Bernie!
top
|
| |

More
homeless
December 11, 2013 --
My fifth 8-hour volunteer nursing shift for Project Homeless Connect (see previous one.)
| PHC 52 Results |
|---|
Client visits: 1,950 |
Volunteers: 887 |
| 65 | Acupuncture Treatments |
| 115 | Behavioral Health (Mental Health & Substance Abuse) |
| 394 | Benefits (CAAP, SSI, CalFresh, HealthySF/SF PATH) |
| 124 | California State IDs |
| 109 | Dental Procedures |
| 252 | Employment Visits |
| 175 | Eye Exams |
| 16,622 | Groceries from Food Bank (in lbs) |
| 70 | Flu Shots |
| 115 | Haircuts |
| 32 | Hearing Tests |
| 15, 80 | HIV & STI Testing, Safer Sex Education & Supplies |
| 31 | Homeward Bound |
| 1593 | Lunches Served |
| 73 | Massage Therapy |
| 145 | Medical Appointments (including us nurses) |
| 130 | Needle Exchange |
| 127 | Photo Portraits |
| 131, 706 | Prescription Glasses, Reading Glasses |
| 373 | Shelter & Housing Applications |
| 220 | Sprint Phone Calls |
| 21 | Wheelchair & Walker Repairs |
top
|
| |

Nurses
next
December 7, 2013 --
Click on this tweet to see a fascinating interview with a brilliant man, Dr. Atul Gawande.
He's one of my heroes, cited often on this page.
His checklists have made huge improvements in surgical outcomes,
and his writings have enlightened Americans about some of the most
bedeviling issues in our crazed health care system.
He describes the career he expected, centering on policy, and his subsequent unexpected fascination with surgery.
My own trajectory bears small similarities, with my nursing degree and license obtained with the intention of bolstering my health IT credentials.
For me the surprise was the astonishing satisfactions -- privilege! -- of working at the bedside, making differences in lives.
That people are even more interesting than technology is, in retrospect, not so surprising.
 In my own vastly smaller way, I hope to emulate him on the nursing side of the hospital bed.
Nurses, too, can benefit from checklists (though, surprisingly, it's a harder problem for nurses than it is for surgeons
because our checklists describe entire shifts with many patients with widely varied problems, rather than single
procedures) and offer a solution named NurseMind.
In my own vastly smaller way, I hope to emulate him on the nursing side of the hospital bed.
Nurses, too, can benefit from checklists (though, surprisingly, it's a harder problem for nurses than it is for surgeons
because our checklists describe entire shifts with many patients with widely varied problems, rather than single
procedures) and offer a solution named NurseMind.
And this blog -- in which I have a lot to say about nursing and health care -- is the writing side of
my hoped-for Gawande-ness.
Imitation, it's said, is the highest form of flattery.
Dr. Gawande, please consider yourself flattered!
top
|
| |

Empire
emerging
December 4, 2013 --
I used to work at Mills-Peninsula Health Services (San Mateo and Burlingame) when they were independent hospitals. Alas, this is but a fond memory. I remember Alta Bates in Berkeley before it, too, was swallowed, and Children's and Saint Luke's in San Francisco likewise. The gobbling behemoth is Sutter Health, and the evidence is mounting that consolidation drives up costs.
The article linked above mentions, for example, "$20 for a codeine pill, compared with 50 cents at a pharmacy" which is not entirely evil capitalism at work, as I have expounded recently. However, Insurance Commissioner Dave Jones (discussed here) has fined Sutter an astonishing $46 million (Sutter Health hospitals agree to pay record payment in Department of Insurance lawsuit) for fraudulent anesthesia billing practices.
Besides costing us more, the consolidation trend reduces transparency of pricing. (This, too, has been the topic of one of my rants.) What do things actually cost? You're going in for your colonoscopy, say, and want to know the price tag? Good luck!
When I had mine a few years ago and phoned three different hospitals for price quotes, only one gave me a straight answer, and that was only after repeated calls, getting handed off from one person to the next, etc.
With all this consolidation and emerging empires, it will only get worse.
top
|
| |

Obamacare
and
me
October, 2013 --
I am in that much-discussed 10% of Americans who buy their own health care insurance. (The others get it from their employers (55%), from the government (31%), or don't have it at all (4%) [source: Wikipedia].)
A letter last week from Kaiser informed me that my health care insurance policy premium would, starting January 1st, 2014, increase by 113%. That's not a typo. It will more than double from $261/mo to $556/mo.
This raises some questions. Can I afford that? Also, I wonder whether my old policy was what Consumer Reports called junk health insurance and Mother Jones called lousy health plans. Kaiser didn't mention the Affordable Care Act ("Obamacare") but it's clear that my old plan didn't satisfy the new law's minimum standards. Kaiser had been selling me junk.
Having always regarded Kaiser as ethical and high quality, frankly, I'm surprised. The good news is that at last they are required to be so.
Nonetheless, I now find myself in a quandary. I have not yet decided how to proceed. Stick with Kaiser? Shop around? Perhaps even on the much-maligned www.healthcare.gov web site? Fortunately for us in California, we have www.coveredca.com. What to buy? How much to pay? I'm working on it. Stay tuned.
top
|
| |

Future
now
September 11, 2013 --
Today I shadowed the charge nurse at an eldercare clinic. I saw the future of eldercare and it is named
On Lok.
It is based on common sense. First, for both quality of life and for cost control, let's "age in place", that is, stay at home. Nobody wants grim institutional corridors, lousy processed food in dining halls full of strangers, and over-sedation by sullen, underpaid flunkies.
Second, center the care around the patient. On Lok calls them participants. Nurses there nurse but they also coordinate care, much like case managers in traditional hospitals but with long-term relationships. Participants and staff get to know each other as they work together week after week, with vans bringing them to and from the clinic, home care nurses coordinating with families for medication administration and safety monitoring. A full staff of medical professionals -- a couple of doctors, three or four nurses, an occupational therapist, a physical therapist, a psychologist, a psychiatrist, and several more -- organize their schedules around the participants at the clinic rather than for their own convenience (the opposite of most health care).
And third -- perhaps this is really first -- is humanity. Staff and participants build real relationships, getting to know each other's foibles and preferences. In nursing school we were taught not to display affection for patients. At On Lok they hug.
When I'm old and near helpless, perhaps demented or otherwise reduced in function, I hope I'm fortunate enough to be cared for by such an organization. On Lok has it right.
top
|
| |

Get
social
September, 2013 --
Dr. Russ Cucina, who led the implementation of Apex (Epic) at UCSF says social media are here (in healthcare) to stay, and he's right! I've written about this before and here is his slide show about social networking for doctors... and why they need to get on board.
Especially good is his taxonomy of levels of participation:
- Minimum: write, communicate, enforce a social policy
- Intermediate: engage reactively
- Advanced: engage proactively
- Master: promote health and your practice
However, I have one peeve, expressed earlier: the patient portals I've seen -- and UCSF's is no exception -- have as their primary objective the goals of the institution; any benefit to the patient is almost a side effect. There is much they could do that would serve patients -- e.g. posting price lists -- but they don't, because it would not serve the institution.
Nonetheless, I applaud Dr. Cucina's technology proselytizing -- go Russ!
top
|
| |

Bedside
blogger
August, 2013 --
My newest hero is Pennsylvania oncology nurse and New York Times blogger Theresa Brown, RN, PhD.
Her blog is named Bedside and is in the Opinionator section of the NYT. In it she wisely opines:
- Nurse staffing ratios are clearly correlated with outcomes.
"...people died... because they were in hospitals with overworked nurses."
- Mutual respect among the members of medical care teams is essential for the safety of patients. "...the silencing of nurses inevitably creates more opportunities for error."
- Like Dr. Atul Gawande,
she decries -- in the final stages of terminal illness -- aggressive care that reduces the quality of life in the small amount of time that remains.
"We need our caregivers to talk to us, ...to understand the treatment trade-offs ...about quality of life over quantity."
- Regardless of where you stand on the importance of Constitutional rights, do not overlook the very real suffering of patients
-- victims, and their families -- due to gun violence. "The talk we hear from the gun lobby is about freedom and rights, not life and death...
So I have a request for proponents of unlimited access to guns.
Spend some time in a trauma center and see the victims of gun violence -- the lucky survivors -- as they come in bloody and terrified.
Understand that our country's blind embrace of gun rights made this violent tableau possible, and that it's playing out each day in hospitals and morgues all over the country."
When you see these things with your own eyes, theory and ideology fall away and humanity emerges. The best nurses practice a profound humanity, and Theresa Brown demonstrates this superbly.
top
|
| |

Homeless connect
August 14, 2013 --
This was my fourth time nurse-volunteering for this worthy cause. We make a big difference for our 5,000 homeless here in San Francisco.
The work is fascinating. It's a peek into a world much bigger than panhandlers and sleepers in doorways. Most of its denizens are invisible to us home-full (non-homeless?) folk. A surprising number of them have jobs. In their world, there is not as much misery as you might expect but of course lots of mental and physical illness. As volunteers and nurses we do what we can but the problems are deep.
Interested? Some hashtags: #phcsf #phc50
And the official website: www.projecthomelessconnect.com
top
|
| |

Mere apps
August, 2013 --
I recently did a demo of my NurseMind nursing checklist app for some technically-savvy people. They were not impressed.
I think the disconnect was based on the assumption -- indeed most people appear to assume this: apps should always be simple and obvious.
Certainly, there is no excuse for a poor user interface, but it is also true that serious professional tools are necessarily complex. For example, NurseMind has a "Remind Me" feature that adds a task to a checklist. It takes three screens to do this because it needs to know: 1. what task to remind about, 2. which patient it's for, and 3. what time it's due. Simple in concept, complex in implementation. The result? With all those screens, the app looks hairy, over-engineered. Yet there is no way to dumb it down without reducing its usefulness.
A corollary of the simplicity assumption: smartphones are not suitable platforms for serious professional tools. That is the obstacle I'm encountering. People expect something trivial and are put off when it isn't. Could this be an effect of McLuhan's dictum, "the medium is the message"? You wouldn't publish the Constitution on fishwrap. And perhaps you wouldn't build serious professional tools on smartphones.
My prediction? This conventional wisdom will evolve. It will become clear that smartphones are real computers and run full-powered professional application software.
Today, we are still in the early stages of this technology. The low-hanging fruit (appealing yet simple applications) is being plucked. But people like me are working on bigger problems. The development cycle is longer and acceptance is delayed, but the trend is real. Watch as it unfolds.
top
|
| |

Roadmap to Single-Payer
July, 2013 --
How do we get there?
- Pass a Law
- Obtain a Waiver from the Affordable Care Act
- Develop a Strategy to Integrate a State-Coordinated System with Medicare
- Integrate Medicaid and SCHIP with the State System
- Determine How to Deal with Workers' Compensation Health Benefits
- Address Other Federal Health Benefits Programs
- Avoid Being Struck Down on ERISA Grounds
- Determine How to Pay for the Unified Health Care Program
The details are here
in this valuable, easy-to-read document, subtitled How States Can Escape the Clutches of the Private Health Insurance System.
In a related article entitled
Single Payer movement in the era of Obamacare, Daily Kos
offers this diagram of how this would look in California.
Now that we have a roadmap, let's go!
top
|
| |

The Inpatient
Nursing Care
Iceberg
July, 2013 --
I am a nurse. Nursing is a major cost at hospitals, yet it's invisible.
Most nursing is not billed. Rather, nursing is in your hospital's room rate,
as maid service is in your hotel's.
Your hospital bill shows only the tip of the healthcare services iceberg.
This is dramatically evident when you look at what you're charged for an aspirin.
Drugstores charge pennies, but hospitals charge dollars. Crazy!
Or is it? Much of that aspirin's cost is hidden:
the pharmacy that stocks it, the cart that delivers it,
the bar-code scanner that confirms the dosage and, especially,
the nurse who gives it to you, but only after making sure that
this med at this time makes sense in his or her highly-trained clinical judgment,
with an explanation and maybe even a smile.
Nursing is invisible but essential.
On your bill, that overpriced aspirin looks crazy.
But look again. You got a lot more than just an aspirin. And thank a nurse!
top
|
| |

Gimme
Data
June, 2013 --
The story is four years old but its lesson still rings true. "ePatient" Dave DeBronkart is one of those rare, self-empowered patients who took charge of his own data and saved his own life.
Healthcare data silos serve the vendors not the patients. In this YouTube video he recounts the saga of managing his near-fatal cancer by claiming his own medical data, and in this one, he "sings" the epatient rap. The rap is funny and laughter is the best medicine, but patient empowerment through access and control of data remains elusive. We can all learn from Dave.
top
|
| |

Simple
Dollar
May, 2013 --
Rethinking your health insurance strategy? At The Simple Dollar, blogger Trent Hamm has created a resource called financial talk for the rest of us that includes cogent explanations of health insurance options. Especially in the rapidly-changing landscape of Obamacare, concise and timely information like this is valuable and worth a look.
top
|
| |

Data ownership, redux
April, 2013 --
As I have discussed previously, patients do not own the medical data that is about them. The providers (the medical-industrial complex) do. I decried this state of affairs and exhorted industry to relinquish this ownership and the patient himself to take more control and involvement. However, the issue is more nuanced than that. I have investigated it further. Here is what I have learned.
top
|
| |

Doc-by-mail?
March 26, 2013 --
Should we communicate with our doctors by email?
Today
iHealthBeat released
the results of a recent Wall Street Journal survey of physicians.
Results were mixed. Some said it saves time and is easier than calling on the phone.
Others complained that it is inconvenient, a data security risk,
and that, unlike in-person patient encounters,
they are not paid for time they spend emailing.
My opinion? I think it's great. I am a Kaiser patient and Kaiser's web
portal offers a mechanism for secure, online communication.
I would prefer email because then I could keep copies of what's said,
but it's better than nothing.
A related question: are those "patient portals" a good thing?
Yes, in a limited way. It's useful to be able to look up those
portions of my medical record that my provider deigns to share,
and to schedule appointments without enduring phone tree misery.
But they have many flaws. They do not share data with other
providers e.g. from one hospital chain to another, or to my
local pharmacy. They offer me no opportunity to add data of
my own such as immunizations, lab results or procedures from
outside their "network". In general, their objectives are less
the patient's and more the vendor's.
This could be resolved by regulatory legislation. It
would require all healthcare vendors to share data.
(To its credit, Obamacare does include some baby steps in that direction.)
It would put the patient in control of access to that data.
It would require storage and management by a neutral third party.
And more...
This wish list goes way beyond mere email...
I can dream, can't I?
top
|
| |

Biggest carriers
January 29, 2013 --
Who are the biggest health insurance carriers in California?
According to today's Los Angeles Times, this $59-billion market is shared as follows:
| 40% | Kaiser |
| 23% | Anthem Blue Cross |
| 14% | Blue Shield of California |
| 9% | Health Net |
| 5% | UnitedHealth Group |
|
Nationwide, WellPoint is on top with 14%, UnitedHealth is second with 12%, and Kaiser is third with 10%.
How do we feel about this?
As the market consolidates, we approach single-payer, which is devoutly to be wished.
Also good is that some of these are non-profits; provision of health care must not be secondary to the demands of stockholders.
However, without public oversight and transparency, their motivations and incentives remain murky.
Concentration of power and whopping payouts to executives of corporations -- for-profit or not -- have no place in a fair and rational health care system.
Only when the system is run by publicly-selected (elected?) officials, subject to the scrutiny of we the people, and driven by no motives other than what's best for us insured, will this crazed and bloated healthcare "system" acquire a semblance of sanity and justice. We have a long way to go!
top
|
| |

Not a moment too soon
December 31, 2012 --
As part of its annual wrap-up of the year's events in medical care, the Medscape site offers this fascinating summary:
10 Medical Errors that Changed the Standard of Care.
We all know that hospitals are dangerous places.
As I have discussed elsewhere, one of the big reasons for this is
nosocomial infections
(bugs you catch in hospitals). Another is errors -- things like
wrong-site amputation, pressure ulcers, and medication allergies.
Fascinating... and horrifying. The good news is that the industry
is paying attention and making the changes that are making
these errors rare. And not a moment too soon!
top
|
| |

Partisans
December 14, 2012 --
The
New
York Times reports that states with Republican governors are refusing to set up health insurance exchanges as
mandated by Obama's Affordable Care Act.
Why? Because they would rather see the Democratic President's Act fail than their citizens receive health care.
It's partisan politics at its worst.
California has been working on its own exchange for a couple of years and it will come to life soon.
It will be good for me because at last I will be able to shop around for my health insurance, comparing
prices and benefits.
It will be good for millions of uninsured people because, in addition to showing what's available, it will
reveal what subsidies and assistance programs there are.
When people in those Republican-governor states see how their elected representatives are working against
them, let's hope they vote differently -- in their own self-interest -- thenceforth.
It's time to end the partisan self-destruction.
top
|
| |


Against the tide
December, 2012 --
San Francisco's Doctor H. J. Kim says you're better off if you don't get sick in the first place.
But here's the economic undertow: treatment is more lucrative than prevention.
He's swimming against the tide... and the insurance companies. He has invested his savings in high-tech diagnostic imaging equipment (the  Imatron) that detects coronary blood vessel occlusions before they are symptomatic. This is a proven technology that goes unused because the insurance companies won't reimburse. His gamble is that patients are wiser when it comes to looking out for their own health. Imatron) that detects coronary blood vessel occlusions before they are symptomatic. This is a proven technology that goes unused because the insurance companies won't reimburse. His gamble is that patients are wiser when it comes to looking out for their own health.
A disease is easier to treat and the outcomes are better when it's caught sooner. The number one killer is heart disease.
With this technology, its precursors can be detected.
Millions of dollars could be saved. Most importantly, lives and suffering could be spared.
Sometimes the right thing to do is to swim against the tide.
top
|
| |

Scan this!
December 13, 2012 --
Today I got a Heartscan. No, there's nothing wrong with my heart (this was confirmed in the test results) but I wanted to see what this wonderful technology can do.
The machine is an Imatron and it does Electron Beam Tomography (EBT), sort of like CAT scanning but with only a tiny fraction of the CAT scanner's radiation. The study that was done on me is called Cardiac Calcium Scoring. It reveals any build-up of calcium plaque in the vessels that supply the heart muscle. This is the precursor for atherosclerosis which, with time, can occlude those vessels, starve the muscle, and cause a heart attack. Indeed, this is the most common cause of heart attacks, and heart attacks are the deadliest disease in America today.
Because the radiation is so little, you could get this test annually yet remain within FDA limits. That is a good idea for people with family history of heart disease or other risk factors. The disease could be caught before it turns deadly. Then it could be treated with radical lifestyle modification, statins, angioplasty, or whatever the cardiologist deems appropriate. The point is, prevention is always the preferable option.
There's just one little problem: insurance companies don't reimburse for this procedure. That makes no sense; you'd think they'd understand that preventing a heart attack is cheaper than treating it. But insurance company "logic" doesn't work that way.
I saw this when I was a smoking cessation counselor: the insurance companies wouldn't pay for smoking cessation but somehow they were ok with paying (a whole lot more!) for lung cancer, emphysema, etc. Similarly, they won't pay for an EBT scan but they will pay to treat a heart attack... assuming the patient survives it.
Here's how that "logic" works: a dollar saved today is a dollar added to the bottom line in the current quarter. It makes them heroes because they hit their target even though it means they will pay out a hundred times as much a few years from now. Not to worry... they will deal with that when the time comes. What's best for the patient? Who cares? That's not a factor in insurers' calculations.
But it is a factor for me, and for any consumer of health care. In other words, everybody. Perhaps when we finally achieve single-payer health care financing, the short-term "logic" will at last be abandoned. In the meantime, get your Heartscan!
In the SF Bay Area: 
top
|
| |

Being Present
September 12, 2012 --
When she was my professor at USF in 2004, Dr. DorAnne Donesky was one of the best, a clear thinker, effective communicator, and inspiring teacher. In her pathophysiology class I learned how the kidneys and the lungs work together for an astonishingly complex metabolic and chemical balance -- they do much more than pee and breathe -- one of many breakthroughs in my understanding of what goes on in my patients' bodies.
Today, Dr. Donesky articulated to me what is perhaps the central value proposition of NurseMind (I couldn't have said it better myself): it supports nurses in maintaining or even regaining their presence.
The unwary nurse can be caught up in the swirl of myriad technical tasks she must do in the course of her duties. She could devolve into a mere technician, getting the details handled but losing sight of the patient. For the aviator, the pre-flight checklist is not a how-to-fly manual but it does make sure nothing important is overlooked, and he wouldn't take off without it. Nurses need checklists no less. As the checklist lets the flyer concentrate on the skilled part of flying by tracking those details -- nothing forgotten, everything on time -- NurseMind frees up the nurse's brain (there's that word again) to concentrate on the patient, to be truly present.
Presence is to nurses what the stethoscope is to doctors: a tool without which they cannot be effective in their work. Indeed, it is perhaps more central than the stethoscope, which is used to evaluate only one aspect of a patient's health status; when she is present with her patient, the nurse's senses are freed to pay attention to everything about the patient. She attends to subtleties, and her clinical judgement is fully available to see everything that is going on -- responses to therapies, psychosocial needs, life condition. The task at hand may be cleaning a butt, but when she's present, the nurse is looking for much more: mobility, skin breakdown, level of consciousness, body systems status, disease processes, and so on.
When the nurse is distracted by work that has grown so technical, or when the "lower-level" tasks such as hygiene are given to lower-skilled workers, opportunities for this all-important presence are diminished. Though unions are not effective in communicating the importance of this tool in nursing work and the gravity of its denial, it is a big part of why nurses strike: they are frustrated by obstacles to being present for patients.
Unlike the unions, Dr. Donesky is articulate on the topic of nursing presence. As a teacher, she strives to instill it in her students and fellow nurses. It is, she says, what above all distinguishes nursing work. The surgeon performs the operation, the therapist conducts life-restoring procedures, the attending is heroic in delivering emergency care. But it is the nurse who sees the patient in between those brief doses of attention, and who is with them on the night shift and able -- when she can fulfill her presence -- to see the big picture.
She recounts the story of three bricklayers:
They labor in the hot sun, placing and cementing bricks with skill and sweat. Of his work, the first one says, "It's a job. Keeps me out of trouble!" The second one says, "It's more than a job, it feeds my family and secures my place in my community." But the third one says, "Look at the fabulous cathedral that's rising on this spot!"
Not losing sight of the central purpose of the work is this all-important notion of presence. That's the nurse Dr. Donesky inspires me to be.
top
|
| |

UCSF's APeX Go-Live
June 4-8, 2012 --
APeX = Advancing Patient-Centered Excellence = UCSF's implementation of the Epic electronic medical record.
This go-live is like changing the engines on an airplane in flight.
Its objectives are ambitious and important -- to at last free health workers and providers from paper charts.
The information flows that underlie every step of every function are being changed.
The impacts on workflows are ubiquitous and profound.
In this vast complex of hospitals and clinics, everyone's job is changing.
Yet through it all, the beds are occupied, lobbies and corridors are bustling as always, and labs, pharmacies, radiology and imaging units, and other ancillary services are as busy as ever.
 Dr. Russ Cucina has been leading the preparations for this week for a couple of years. His budget, he tells me, is $116 million -- small change compared to the $2 billion Kaiser spent to convert to Epic -- yet a massive project nonetheless. Each implementation of Epic is so unique that it is given its own name -- Kaiser's is HealthConnect, UCSF's is APeX. For a nursing/medical informaticist, this week is history in the making, not to be missed. The project is a remarkable success and I have the good fortune to see it up close.
Dr. Russ Cucina has been leading the preparations for this week for a couple of years. His budget, he tells me, is $116 million -- small change compared to the $2 billion Kaiser spent to convert to Epic -- yet a massive project nonetheless. Each implementation of Epic is so unique that it is given its own name -- Kaiser's is HealthConnect, UCSF's is APeX. For a nursing/medical informaticist, this week is history in the making, not to be missed. The project is a remarkable success and I have the good fortune to see it up close.
During this week, I am enrolled in UCSF's School of Nursing's Summer Academic Enrichment Program (SAEP), an upbeat introduction to its advanced practice and research offerings. For me, the best part is the clinical rotations, selected according to attendees' interest areas. Mine was not in a nursing unit but in the Nursing Ops area of the APeX go-live Command Center.
The Command Center has the staffing, technology, and aura of ground control for a moon shot. Perhaps a military metaphor is even more accurate, as it possesses a spectrum of clearly-defined job roles and responsibilities in a complex hierarchy with logistics, processes and procedures precisely scheduled. Dr. Cucina's team -- a hundred people or more -- is focused and professional.

In my rotations, I shadowed a couple of the Informatics Nurse Specialists (INS RNs) who performed a scout function, rounding from one hospital unit to the next, checking in with the local "super users" (nurses who had received special training in preparation for deployment of the new system) to detect and report software and process issues, and to confirm that fixes are "pushed out" and solve problems as promised.
My INSs were Craig Johnson, RN, and Sandy Ng, RN (pictured here with me). Brilliant and hard-working, they taught me a lot. Many thanks to you both, and congratulations to UCSF on achieving a major milestone!
top
|
| |

Silent organs
Jan. 2012 --
Having worked as a smoking cessation counselor, I can attest to the difficulty of achieving this particular behavior change. Those who work with alcoholics describe their work similarly. Both behaviors have dire health consequences yet are consummately difficult to extinguish. Part of the reason is that the organs that are damaged by these behaviors are "silent" -- without pain or sensation -- until they are in extremis.
If lungs felt pain when their delicate alveoli were damaged by toxic smoke, it would be easier to get people to stop. Finding the sensations unpleasant, they'd be less likely to continue. Assaulted by alcohol, the liver, too, suffers damage silently. Alas, evolution did not anticipate tobacco or alcohol and hence provided no detection of the harm they do. This silence facilitates the denial that perpetuates the harmful behaviors.
Compare this to, say, traumatic injury or heart attacks. These things hurt, so people avoid them. In my smoking cessation work, I would depict the processes occurring in lungs, circulatory system, and even the bladder when assaulted by the toxins from tobacco smoke, in an attempt to apply reason to decisions that are unreasonable. Alas, education is a less effective motivator than pain. Those silent organs make it a hard job.
top
|
| |

Lateral violence
Dec. 2011 --
In an article entitled No Tolerance for Bullying, the Advance Web for Nurses reports that the ten common behaviors of lateral violence in nurses, as described by Martha Griffin, PhD, RN, CS, director of nursing education and research at Boston Medical Center, Boston, are: non-verbal innuendo, verbal affront, undermining actions, withholding information, sabotage, infighting, scapegoating, backstabbing, failure to respect privacy and broken confidences. Have you seen these in the workplace? Whom of us hasn't?
Lateral violence is getting increasing attention in the media. Another recent article at the www.nursetogether.com web site entitled, Ending Incivility in the Nursing Profession posits that lateral violence is often considered normal by nurses and describes it as an "oppressed group behavior".
As I have seen, it starts even before the workplace -- it starts in nursing school. I had several experiences of it there. Though I was careful about interpersonal politics, run-ins with the bizarre personalities of some people in positions of power proved unavoidable. For example, one of my teachers, a rather strange man who in his lectures delighted in showing to our class videos of himself dancing in a pink tutu and boasted about the low prices of prostitutes in Thailand, took a strong and personal dislike to me and on one occasion accosted me in the hallway and, unprovoked, threatened, "I could flunk you! I could get you kicked out!" When asked about it in a meeting with the director, he denied the hallway incident and accused me of "having an agenda" though what that agenda might have been he would not say. The director did nothing.
The problem lies not only with individuals but with institutions. Lateral violence had occurred, yet no action was taken. As in some hospitals, some nursing schools do nothing to curb it. They ignore it rather than deal with it. From the director's perspective, in a few months I would be gone whereas the teacher would likely be there for years so her easiest action was to overlook his transgressions. The lesson to me was to expect no integrity from nursing institutions. Shame on them.
Is it the culture of nursing or the culture of the school that creates the climate of impunity for these behaviors? Does it matter? Regardless of the source, an ethically-run institution should not tolerate such behaviors. I stuck it out, turned the other cheek, and collected my sheepskin. Had I known what to expect, I would have chosen a different school, though it's not clear that another would have handled such issues any better.
Lateral violence should be recognized and dealt with. Instead, in nursing we are taught from the beginning to put up with it and that it's even ok to perpetuate it, as such behavior seems not to have consequences. Shame on us.
top
|
| |

Healthcare and advertising
Practice Fusion conference, 11/11/11 --
With 1300 other healthcare workers, I sat in a convention hall in San Francisco and observed panelists debate the merits and issues of Practice Fusion and the electronic health record industry in which it appears to be thriving. PF is an advertising-funded, free-to-its-users, web-based electronic health record.
The company was founded in 2005 by Ryan Howard, a youthful and energetic entrepreneur with big and timely ideas. Five years ago I had coffee with him, having just discovered word of his startup not far from the more conventional electronic medical record company where I was working at the time. I was interested to learn about the direction he was taking and the technology he was fielding. The marriage of healthcare and the web was, I believed and still believe, made in heaven. Instead, what I experienced was a blizzard of tech-talk buzzwords -- disruptive technology, web-enabling, silo-liberating, blah blah -- nothing about medical data standards, medical office workflow redesign, new paradigms for medical data ownership, and so on -- the meat of the issues that such a system would surely challenge.
The tenor of the conference was much the same -- lots of fluff, a half hour of music by a gospel choir, feel-good cheerleading, not much content. Mr. Howard himself delivered one of the pep talks. In it, he claimed that PF's patient population was bigger than Kaiser and Sutter Health's (our two largest Northern California hospital chains) combined. While it may be true that portions of 22 million patients' medical charts do reside in PF, these patients are not PF customers, they are PF users' patients. Unlike Kaiser and Sutter, PF provides no medical care, nor does it employ thousands of doctors or possess thousands of hospital beds. The comparison is vacuous.
Regardless of flaws in PF's product, is the underlying business model -- and its potential effects on healthcare data management -- sound? Is a database attached to a web server the right place for my medical history? Is the Internet the best way for my caregivers to share and access it? What effect does this model have on costs and especially on outcomes?
The central feature of PF's business model is that it is funded by advertising, not by users. The doctors and clinics that entrust their patients' data to PF pay nothing for it. This surely has some effects on the nature and content of the service PF provides.
This raises several questions. First, is it a strategy for long-term survival? Every Internet user knows that before long, banners and advertisements "disappear". Our eyes learn to ignore them, and we rarely click them. There are even software solutions as popup preventers and flash suppressors to expunge ads from the screen. If the ads don't work, can PF survive?
If the business model is not viable over the long run, how will PF survive? As it is privately held, we cannot know for sure how it is faring financially, but my understanding is that today, after six years, it still runs not on revenue but on venture capital.
The deeper issue, in a medical decision-making setting, is whether advertising is ethical and appropriate. Does it skew treatment decisions? A heatedly-discussed precedent is the advertising of pharmaceuticals. The businesses that advertise make calculations about advertising in any medium, be it television, radio, newspapers, billboards, or the Internet. In any medium, the concern is return on investment. If advertising fails to increase sales, it will not be done for long. Thus, the mechanism must be that well-placed advertisements do indeed skew clinical decision-making toward the advertised products. Is this how we want our treatments chosen?
Any discussion of advertising must recognize the real product; what is being sold to whom. In this regard, the Internet is much like television. As is television to its audience, PF is "free" to its healthcare provider users. The payers are the companies that advertise. These are the real customers, and what is being sold to them is the attention of the users. So, in a sense, PF's product is not an electronic health record but the attention of its users, all those people in that convention hall.
Consequently, PF's product design and support decisions are driven less by the needs of patients, providers, and the exigencies of medical care, and more by what yields the biggest bang for the advertiser's buck. Does PF mine the data? For example, when a diagnosis of diabetes is entered, might an ad for a related product such as Metformin be displayed? I don't know and I bet PF isn't telling.
For strategies such as PF's, improvements in clinical outcomes and reductions in health care costs are at best a side effect.
Is this how we want our health care data stored and managed?
Despite my doubts about Mr. Howard and his company, I believe that the answer is yes.
With HIPAA-compliant confidentiality safeguards, storage on Internet-connected servers enables wide access to patient data.
It can spare us redundant tests, and eliminate the siloing of data in the file cabinets and computers of doctors' offices and hospitals.
Dearest to my heart (as is well known to readers of this blog) is technology's potential to put the patients themselves in control of their medical data. The trend is toward patient empowerment in medical decision-making. If PF moves this industry toward those goals, I applaud its efforts.
top
|
| |

UC
is
in
trouble
September, 2011 --
In the California budget crisis, most of the University's State funding has been cut.
On a personal level, I am saddened and dismayed by our State's repudiation of its noble 1960
Master Plan for Higher Education.
To it, I owe much of my own academic and professional career.
In the bigger picture, to it our State owes much of its economic ascendancy to one of the world's largest economies, an achievement that is now threatened.
Our renouncing of this proud promise to our own future began in the '70s with Jarvis-Gann and accelerates today with mean-spirited anti-tax movements of Grover Norquist and his demagogic Tea Party offspring.
The stepwise gutting of the mighty UC system is both tragic, putting top-flight University and graduate education beyond reach of ever-growing numbers, and short-sighted, reducing the growth of technology and culture, diminishing our prospects for a prosperous future.
This is a sad time indeed.
top
|
| |

Greedy nurses?
September 23, 2011 -- (to the San Francisco Chronicle)
Dear Editor --
I am a California nurse. Yesterday, 23,000 of us went on strike. Passers-by honked and waved and were almost universally sympathetic to our cause. If you are one of the few doubters, this letter is for you.
The nurses' unions are among the few that have not yet been eviscerated.
Unions should be strengthened, especially in the light of the growing chasm between rich and poor, ballooning corporate profits, and what's been called the "Bush Economy."
Without unions there would be no middle class.
In the Bush Economy, profits and tax giveaways go to banks that do not lend and corporations that do not hire.
Gut the unions and the fate of the middle class is sealed.
Yet some have called us "greedy nurses."
There was even a full-page ad in yesterday's SF Chronicle claiming that nurses average salaries of $150K.
In our dreams!
No nurses I know earn six figures, and the one or two I've heard about do it by working overtime hours to exhaustion, a path to certain burnout.
The most important thing to know about nursing work is how hard it is, and how many, many years it takes to acquire that level of expertise and instinct that does, truly, save lives. For more than any other reason, patients go to hospitals for nursing care. Yes, they have procedures like surgeries and therapies, but part of why I prefer nursing to doctoring is that while the doctor gets ten minutes with the patient, the nurse gets an entire shift. That's where real healthcare happens.
The personal, emotional, and professional commitment nurses put in to make this happen is unlike any other job.
You can't imagine this until you've been there.
There is also a surprising amount of pure physical hardship. Here are a few quips from the culture of nursing:
- What nurse hasn't dealt (many times) with a "code brown"?
- And what do you call a nurse with a bad back? Unemployed.
Seriously, the number of workplace injuries -- especially needle-sticks in the age of AIDS, and back injuries from lifting today's epidemic of obese patients -- is shocking. This work is not just emotionally draining, it's dangerous. And you would begrudge nurses their vacation days and health care benefits?
So when I hear talk of "greedy nurses" -- especially from corporate executives like Sutter Health's CEO Pat Fry who awarded himself a $2M bonus this year -- my stomach turns.
The real challenge -- while applauding the nurses for holding their ground -- is to unionize the other professions and redirect some of this nation's wealth back down from the top.
And if ever you get sick and then well again, thank a nurse!
Thanks for listening,
Dan Keller
top
|
| |

Hear
us
roar!
September 22, 2011 --
Today was the strike as planned.
Only about 5% of the union nurses crossed the picket line.
We are nurses, hear us roar!
California Nurses On Strike
Nurses at dozens of Calif. hospitals strike

top
|
| |

Strikes, yikes!
September 18, 2011 --
In three days (on the 22nd) thousands of Sutter Health
nurses will go on strike
and in sympathy with them will go thousands more Kaiser nurses.
These are two of the largest hospital chains in Northern California.
The nurses are defending hard-won employment contract terms (some health care benefits, some sick and parental leave benefits, etc.)
Especially pertinent in California, the only state with mandated nurse:patient staffing ratios (e.g. 1:5 in med-surg units) is participation in the staffing decisions, which, too, Sutter hopes to take away. This is important; it is one of the ways that nurses advocate for patients. Numerous studies have made clear the impact of staffing ratios on health care outcomes.
Of course, there are two sides to every story. The business of hospitals is a tough one (though Sutter is having record profits this year). Medicare reimbursements are being reduced, making it harder to "make the numbers". My friends in hospital management are stressed out (though not top management whose pay has seen handsome raises). Particularly problematic from the hospitals' point of view is
the EMTALA Act that requires hospitals to provide care to anyone needing emergency treatment regardless of ability to pay. This means that the hospitals provide care for the medically indigent for free -- a tough way to run a business.
Nonetheless, I guess it's obvious where my sympathies lie. My
CNA dues are paid up and I'll be out there on the picket line.
top
|
| |

Trimming the fat
September 15, 2011 --
Does Livermore have the most slender people?
Does nearby Los Banos have the fattest?
Or does it have the most bariatric surgeons?
When you're selling a hammer, does everything look like a nail?
Are high-tech healthcare choices driven by doctors who are also businessmen?
(I have written on this topic previously.)
See the data for yourself at
the California Healthcare Foundation's interactive map, released today.
The hardest question: what should we do about it?
top
|
| |

New fraud
September 1, 2011 --
Though retired now, my brilliant and inspiring
grad school professor Dr. Donald W. Simborg
continues to expound and illuminate. He writes
with authority,
having served as co-chair of the expert panel
of a study group related to the
Nationwide Health Information Network (NHIN) that looked at healthcare fraud.
He says, "Healthcare fraud is the most lucrative thing you can do if you're a crook... We're talking about a $250 billion problem."
In this month's J Am Med Inform Assoc (2011 Sep 1;18(5):675-7), he decries new techniques for fraud that have become enabled by modern electronic medical record (EMR) systems. These include:
- Identity theft of provider IDs and patient IDs. This enables the fabrication of fraudulent claims.
- Record cloning -- another way of producing fraudulent claims.
- Copy forward -- data that is entered ahead of its actual collection, e.g. vital signs entered the day before the patient visit.
- Single-click notes -- templated notes entered prior to the patient visit and subsequently left unaltered.
- "Make me an author" -- an EMR feature that enables a physician to substitute their signature attribution for that of the person who actually entered a note.
- Unaudited edits -- another "feature" that enables retroactive editing of a note without logging the amendment. Some vendors even enable the suspension of audit trail logging.
- Evaluation and Management (E&M) code optimization -- Some EMRs suggest "upcoding" (changing the Current Procedural Terminology (CPT) service code from which billing is generated to a more expensive one) of E&M codes, and indeed with the increasing use of EMRs we have seen a rise in Medicare billings.
I applaud my professor's call for better industry oversight.
EMRs can do much to improve quality, continuity, and research in healthcare.
They must not also serve as tools for fraud.
top
|
| |

National Health IT Week
September 12, 2011 --
Today is the first day of the Sixth Annual National Health IT Week,
September 12-16, 2011.
Information technology is essential to healthcare,
a fact our technology-worshipping country
has been paradoxically slow to recognize.
To see why, as always, follow the money.
Our for-profit insurance company middlemen have
a sole incentive: their bottom line.
The long-term benefits of effective IT
systems -- things like quality,
continuity of care,
population-wide and longitudinal
data collection and analysis -- generate no profits.
Hence, they aren't reimbursed.
Hence, we don't have them.
Most US hospitals still lack comprehensive electronic medical record-keeping.
Those that do have them cannot -- indeed prefer not to -- share their data.
Well-intentioned (mostly governmentally-funded) efforts at Regional Health Information Organizations
have gained little traction and in some cases shut down.
So the primary objective of this Health IT Week is "...to educate industry and
policy stakeholders on the value of health IT for the US healthcare system."
It's astonishing and disheartening that we still have such a long way to go.
top
|
| |

Doctors and nurses are not enough
July 19, 2011 --
Today I shook the hand of yet another spirited and passionate public servant,
Fiona Ma, California Assemblymember from my University's San Francisco district.
Her work spans many issues but for me the one of most interest is, of course, health care.
Ms Ma's cause celebre in this arena is
advocacy for Hepatitis B
-- education, screening, vaccination, treatment and San Francisco's
Hep B Free program.
This is yet another ground-breaking collaboration
between government and health care providers. We do a lot of that here;
we are leaders!
Health care services are not enough.
Public advocacy is another essential component
and people like Ms Ma make it happen.
top
|
| |

A good guy at the top
July 14, 2011 --
Today I shook the hand of another warrior for the people:
Dave Jones, California's new Insurance Commissioner.
He describes himself
as an activist.
What he doesn't say in this article but did say in
his speech today at the Public Policy Institute of California
is that he is a whole-hearted supporter of California's
Senate
Bill SB810, our best hope for a
single payer healthcare system.
(I've written lots about it in this blog.)
Inaugurated in January of this year, Mr. Jones hit the ground running,
doing what he can with the limited powers of his office to restrain
the insurance companies.
For example, he has enacted in California (modeled on
the federal reforms) limitations on the "overhead" that
insurers can incur, requiring them to spend $0.80 of
every premium dollar on actual healthcare (hospitals,
doctors, medical and ancillary services and providers.)
To everyone but the employees and shareholders of
Anthem Blue Cross, that's still 20% of pure waste
but it's a step in the right direction.
Go Dave!
top
|
| |

You'll be safe here
July, 2011 --
Some nurses are miracle workers.
With the Mom and the doctors all but resigned to
getting the baby out by C-section, L&D RN Diane says,
"Let me see what I can do." She talks to the baby
(still inside the Mom) and lets it know that it's
safe to come out. The three of them work together,
developing a deep trust, and often this enables
the baby to be born the natural way after all.
Is this miracle work? Or the product of
decades of experience, and the non-quantifiable
but undeniable successes that can be attained with
intuition and spirituality?
Where are the randomized, double-blind, peer-reviewed,
reproducible, gold-standard studies and clinical trials?
Combining these two approaches -- science and
intuition -- gives patients the best outcomes.
It's eye-opening to see it in real life.
top
|
| |

Google Health is dead
June 24, 2011 -- From an announcement on
Google's
official blog,
we learn of the end of a wonderful experiment.
Google Health was a great idea -- empowering patients with control
over their own data -- that
we applauded.
Alas, the business model was weak;
not enough users (and no insurance companies)
saw enough value to get on board.
Its primary virtue was the real life implementation
of a Continuity of Care Record
-- something that we sorely need.
The value was there but it was subtle.
In a fascinating analysis, Missy Krasner observes that the
challenge (that proved insurmountable) was the dominance by "tethered"
health care records, those operated by health care providers (hospitals,
doctors' offices, and tertiary and ancillary providers such as outpatient
services and labs). The drawbacks of these
data silos is that data is
not shared among providers, hindering patient mobility.
Providers don't want to lose business by enabling patients to go elsewhere.
Nonetheless, PHRs (personal health records) such as Google's must ultimately prevail.
KevinMD agrees with me: Google gave up on electronic personal health records, but we shouldn't.
This will happen only with guidance from regulators.
Obama's health care reform does this... alas, too late for Google.
top
|
| |

Cancer cures?
June 2011 -- My friend Dick Karpinski writes about
"known but unused cancer cures"
at his Cure Cancer Now Home web site.
Though I'm not qualified to comment on the specific cures
he discusses, I do not doubt that the unprofitable ones
get little attention. Thanks, Dick, for raising our
awareness.
top
|
| |

Woo Hoo! We're Winning!
May 2011 -- Senator Leno's Single Payer Health Care Bill Passes Health Committee...
California OneCare: Full Care, For All, For Less --
check it out!
top
|
| |

Record Profits for Health Insurers
May 16, 2011 -- Want to know how things really work?
Follow the money! Insurers Take In Record Profits as U.S. Residents Spend Less on Care -- translation: in these times of economic stress, we're living with less yet continuing to enrich these parasites.
Some experts believe the companies are trying to raise premiums before stricter regulations are enacted under the federal health reform law, such as a requirement that companies cover individuals with pre-existing conditions.
Translation: they, too, can read the handwriting on the wall.
Big change is coming -- a vast bureaucracy to be dismantled! -- and not a moment too soon.
top
|
| |

Foreshadowing things to come?
May, 2011 -- When a B-25 bomber crashed into the 79th floor of the Empire State Building at 9:49 a.m. on Saturday, July 28, 1945, killing 14 people, the injured were rushed to Bellevue's Emergency Room. A nursing student at Bellevue at that time, my mother writes:
As students we always said, "If ever I'm in an accident, take me to Bellevue ER."
The ER staff had an amazing ability to respond to the very serious situations that walked in or came by ambulance and to the bizarre, too.
Bellevue had (don't know if it still does) a museum -- a glass cabinet -- of things removed from the bodies of patients who showed up in the Emergency Room. One was a fairly large steel nut removed from a guy who was working in a garage on the night shift. He had screwed it on to his penis which swelled with blood so he couldn't remove it. Fortunately, he wasn't circumcised, so the multi-talented ER doctors circumcised him and in the process were able to unscrew him.
There were no private rooms at Bellevue, but each ward had a room for a V.I.P. or someone with a highly contagious serious disease. The less fortunate patients were housed in the enormous wards with dozens of others.
There was one who repeatedly got out of his bed and peed in the corner. When asked by an angry staffer, "Where do you think you are?" he got himself a psych consult by answering, "Grand Central Station!"
In retrospect, this doesn't seem like an unreasonable reply. It was an enormous ward with 60 to 80 patients. There were beds on both sides and down the middle. There were no call bells. To get a nurse's attention to get a bed pan (or to be on the schedule for when bed pans were passed out from a wheeled stretcher where they were lined up on top), a patient had to get out of bed and find her. Tough luck for the patients who were too sick to get up!
If a Catholic patient died and was not on the "On Serious" list (a code meaning that he or she would need last rites) New York City could be sued. Patients got scared when they were put "On Serious" as a precautionary measure but we did it anyway to protect ourselves.
On the night shift -- even if it was our first time in that ward, and even if we were working it alone -- if an "On Serious" patient died, it was our fault. If the patient was not breathing we would lift their eyelid and shine a light to check for a reaction. Living patients were not happy to be so rudely awakened. Then we rushed to the head nurse's desk to check the patient's card to see if he or she was "On Serious" and above all to see whether the patient was Catholic. If they weren't Catholic, we could breathe a sigh of relief and simply fill out an accident report. The duty of the student was first and foremost to protect the City.
When the night nurse supervisor made rounds during our shift, everything better be in order. (Remember, this was WWII and there were few nurses available; most were in the war zones. Students' education was work-centered, not education-centered.) There was an intern who could be called to the floor if necessary, but he had been answering calls half the night and had conked out in his room. The students hesitated to call him unless the patient was really in trouble so we rarely did. No one thanked us for our heroics but we knew and so did our patients.
That was an unforgettable time.
top
|
| |
|
Non-Profit in Name Only
May 1, 2011 -- In a letter today to the
San Francisco Chronicle, I wrote:
Thank you for
Stacy
Finz's article in today's newspaper
exposing abuses by for-profit professional schools.
These practices are not limited to the for-profit schools.
They also take place in the nominally non-profit schools.
I am a recent graduate of Oakland's Samuel Merritt University's school
of nursing, another that preys on people hungry for employment.
SMU is a cash cow for its parent company, the
Sutter Health hospital chain. According to its
alumni literature, last year
it
earned $10 million profit
on revenue of $40 million, a 25% margin.
It is non-profit in name only.
So where do profits go in non-profits?
Much of that leftover cash is funneled into the pockets of
exorbitantly-paid
executive staff -- profit by another name.
And where does all that cash come from?
We ABSN (Accelerated Bachelor of Science in Nursing)
students
pay $52,000 for a year of poor-quality instruction. For example,
Diana Jennings, the instructor of the so-called Nursing Research
class (included in the curriculum to satisfy the accreditation checklist;
Jennings delivered only one lecture in the entire semester)
brightly proclaims, "Everyone gets an A!"
In addition to the high tuition,
fees such as $420/semester
are charged as "Lab Fees" for a lab that is almost always locked,
and poorly stocked.
In the few hands-on practice sessions that are offered, we must share
and re-use supplies like bandages because the school doesn't buy
them in adequate quantities.
Thanks for helping to expose an exploitative industry.
top
|
| |

California Universal Health Care Act
April, 2011 --
California Senate Bill 810 -- It's back! And coming up for a Senate Health Committee hearing on May 4th.
(Thanks again, Mr. Leno!)
Let's save money (yes, our state budget is deep in the red) and cover everybody at the same time.
How? Eliminate the middle man! Let the State be the single payer.
It works in Massachusetts.
Why not here?
Though I'm no longer a student, I continue to support the goals of the
California Health Professional Student Alliance
(CaHPSA) and participate in its calls to action.
I have telephoned my State Senators and let them know how important it is for California -- along with the national
health care reform -- to move forward. Our "system" is a disgrace... but we can fix it.
We must fix it. Go SB810!
top
|
| |

Beware the 3 Ds
April, 2011 --
"Beware the three Ds," my mother's nursing instructor intoned: "Drugs, drink, and doctors!"
It was 1944 and America was at war. The experienced staff nurses were abroad, serving in the U.S. Nurse Corps, providing medical care for the troops. Judith -- my mother -- had just graduated from high school and, newly-admitted to nursing school, was pressed into service to fill the need here at home. She writes:
In 1944, we were student nurses at Bellevue, a 3,000-bed hospital in New York City, on First Avenue. Described as a city within a city, its many buildings stretched from East 26th St. to East 30th along the East River. It had a prison, a mortuary, and even its own State Supreme Court.
Bellevue could not refuse anyone. If you were a patient in a private hospital and couldn't pay your bill, you were shipped off to Bellevue, no matter how sick you were. That was sometimes referred to as your "last ride".
It was a catchall for paupers, psychotics and criminals. Bowery bums loved to winter at Bellevue, finding some way to get admitted and, once admitted, would figure out how to make their thermometers spike a fever, assuring them of a warm bed for another night.
Bellevue was one of the world's great teaching centers. It was a coveted learning ground for young, new M.D. interns (the third D!) and for student nurses, too. With the seasoned nurses gone, the student nurses filled in, taking classes during the day and covering on the wards at night.
It was hard work. Students were assigned to medical and surgical wards, immense rooms with 60 to 80 patients, none of whom we had seen before. On a good night we had a nurse's aide, but often we were alone with all these very, very sick patients to care for.
At Bellevue, we treated the worst cases of the worst diseases. Nurses who had trained at Bellevue proudly wore their organdy caps with the ruffle all around and were respected wherever they worked.
top
|
| |

April, 2011 --
Though it's already more than a year old, this article (from August, 2010), is such
a valuable explanation of a vexing issue that I'm linking it here.
One of my favorite writers on health care, Atul Gawande in the New Yorker, observes that
modern medicine is good at
staving off death with aggressive interventions — and bad at knowing when to focus,
instead, on improving the days that terminal patients have left.
A good read on an important topic.
top
|
| |

March, 2011 --
As a programmer and nurse, I can tell you that "coding" means something awfully different to each!
top
|
| |

February 24, 2011 --
At my alma mater UCSF, I attended a
symposium on innovation in California. Innovation is our strength (Silicon Valley!) and it will create jobs and revive our economy.
The symposium was a star-studded event. The speakers included one of my heroes, Lieutenant Governor Gavin Newsom. Sitting next to me was Elizabeth Blackburn, a Nobel prize winner.
Another speaker was former California Governor Gray Davis (whose hand I shook). He said, "If you're born in the east, you grow up and you want to join something. If you're born in California, you grow up and you want to start something."
Indeed I do...
Here it is (Powerpoint, of course)...
Wish me luck...
top
|
| |

February, 2011 --
The conventional wisdom says that government-run = low quality and inefficiency... But is that true? Not so fast, says Mike Doyle of Medsphere, a promoter of the Veterans' Administration's electronic health record system, VistA. I had an opportunity to learn and use VistA on one of my clinical rotations and found it excellent. Furthermore, the VA itself is a success story. In his well-researched blog, Mike writes:
By all rights, after all, the VA should offer the worst care anywhere: it's a gigantic, unionized bureaucracy, micromanaged by Congress and political appointees, and beset by an uncertain budget, an aging infrastructure, and a legacy of scandal. That it nonetheless outperforms the rest of the U.S. health-care system, on metrics ranging from patient satisfaction to cost-effectiveness and the use of evidence-based medicine, suggests that much of what we think we know about health care simply isn't true.
The VA is not the only example. Medicare proceeds with 3.9% administrative overhead (acccording to the New England Journal of Medicine's "Cost of Health Care Administration..."), compared to private insurer's 15-35% overhead, depending on whose numbers you use. For example, the Physicians for a National Health Reform's peer-reviewed studies say 31% of our health care dollar is spent not on medical care but on the overhead and profit of the private insurers (Anthem, Blue Shield, Aetna, Humana, etc.)
And while it's true that
the plural of anecdote is not data,
my family's experience with Medicare has been excellent.
VistA works well and I found it easy to learn and use. Furthermore, the source code is in the public domain (open source) and stands a good chance of setting the standard for the industry. It makes electronic health record software affordable.
Even  Fox News has gotten behind it.
Nonetheless, Doyle cites research that says: Fox News has gotten behind it.
Nonetheless, Doyle cites research that says:
Astonishingly, 20 years after the digital revolution, only 1.5 percent of hospitals today have integrated IT systems like the VA uses, and those that do often find their commercial software programs to be buggy and inadequate.
It's time for an end to the myth of quality and efficiency in private sector health care!
top
|
| |

February, 2011 --
Occidental cultures generally hold that the
human identity resides somewhere behind the eyes --
in the brain. For example, the Mind-Brain
Identity Theory says that, "...mental states are identical with brain states."
Not so fast, say I.
Damage to the brain is often associated with damaged thought processes.
For example, Oliver Sacks
"...throughout his career as a physician and neurologist,
...studied patients who exhibited 'a strange mixture of [mental] strengths and weaknesses.'
His patients had autism, William's Syndrome, Tourette's Syndrome, amnesia and other conditions."
When the brain malfunctions, thoughts malfunction.
However, this does not preclude the involvement of other bodily organs in personal identity and thought.
Our Western notion that identity, thoughts, and feelings reside exclusively within our skulls is at best
dubious, more likely erroneous. Ask anyone who has undergone an amputation. As nurses we are taught
that phantom pain is real pain but more than that the amputee will tell you that part of themselves --
not merely an extremity -- is gone.
 Another way in which our sense of self encompasses more than the contents
of our heads becomes clear with the deaths of family and friends. In a real and profound
way, with each such passing we lose part of ourselves. We exist not just in the context of our
bodies but also in terms of the people who know (or knew) us, our accomplishments, personalities,
and personal histories.
As our isolation increases, our place in the world is diminished. There are vocabularies for
discussing this, for example Carl Jung's collective unconscious
in which we exist not only individually but also in community.
Another way in which our sense of self encompasses more than the contents
of our heads becomes clear with the deaths of family and friends. In a real and profound
way, with each such passing we lose part of ourselves. We exist not just in the context of our
bodies but also in terms of the people who know (or knew) us, our accomplishments, personalities,
and personal histories.
As our isolation increases, our place in the world is diminished. There are vocabularies for
discussing this, for example Carl Jung's collective unconscious
in which we exist not only individually but also in community.
Nearly every Latin love song refers to the coraçon -- the heart -- as the locus of emotion.
Eastern religion and medicine recognize a dozen or so
chakras -- pathways for flows of
energies in the body -- located along the spine, in the ovaries or prostate, the throat, and so on.
In our own western culture we speak of visceral emotions and gut feelings.
Our skin crawls; we know things in our bones; and so on.
The point is that all these organs participate in the formation of our consciousness
and our emotional state.
My hypothesis here is that the kidneys are especially central to emotional state.
In nursing school, we learn that they regulate fluid and electrolyte balances.
These in turn drive cognition and mood.
When the kidneys do not sufficiently remove ammonia from the bloodstream,
we become demented. When they imperfectly regulate our bodies' acid-base
balance, we become acidotic or alkalotic and thus agitated or lethargic.
We think with our brains and with our kidneys.
The distinction between mind and body is a paradigm of our western culture, at times useful
but at other times driving us to discussions of placebos (with which
the mind bluffs the body), etc., that emerge as corollaries.
We believe this dichotomy deeply.
But what if it weren't entirely true?
Another model might serve us better.
What might it be called? The Thinking Body? Placebonics?
Kidneys 'r us?
We do think with our brains...
Also our hearts, guts, skin, bones, kidneys --
the mind is the whole body!
What a concept!
top
|
| |

February, 2011 --
California RN license #790869. At last.
top
|
| |

February, 2011 --
Healthcare dollars are spent in two fundamentally different ways and should be collected and managed accordingly.
These are:
- Preventive and predictable health care expenses: our children's immunizations, prenatal care, our routine diagnostics (PSA tests for older men, mammograms for older women, etc.), and our periodic checkups. These things are completely predictable from the moment we're born -- indeed, from the moment we're conceived -- through our entire lives. The costs should be budgeted and funded for every one of us without exception. We should all pay into a system that provides them, and there is no reason for anyone to earn a profit from it. It's a public service like law enforcement and fire departments and should be funded and provided similarly, by publicly-funded, local community clinics. There is no place in the preventive/routine care part of a rational health care system for for-profit insurers. The incentives in such a system are wrong and result in a system that's unfair and that delivers inadequate care.
- Costs of casualties and illnesses (unpredictable): should be managed as insurance in which risk is shared across an entire population. The services are best delivered (as they are today) by for-profit, centralized, high-capital-cost, acute-care facilities (hospitals and specialized service units such as dialysis centers, imaging centers, clinical labs, psychiatric offices, and hospices). Anyone to whom a casualty or illness happens would be covered, and everyone would pay in to the fund equally (the "triple mandate"). The fund would reimburse the service providers with preference and incentives for those that provide the best care and the lowest prices.
This is just common sense.
None of this would prevent anyone from buying any other health care service, or from using the provider of their choice who might be "outside the network". Anyone can buy whatever they want if they have the money. The Canadians have forbidden this, saying that it would create a two-tier system and perhaps they're right. Alas, we already have a two-tier system in the USA, and it's ugly: those with and those without.
Obama has taken some baby steps toward an overhaul... A good start. We need that and a whole lot more!
top
|
| |

January, 2011 --
...And pound-foolish. Health insurance (mine is Blue Cross) will not pay for medicines if they are over-the-counter. They pay only for prescription medications, those that are ...licensed medicine that is regulated by legislation to require a prescription before it can be obtained. The term is used to distinguish it from over-the-counter drugs which can be obtained without a prescription.
 For example, my eye doctor prescribed Ocuvite, shown by controlled, randomized studies to delay onset of age-related macular degeneration. My Dad had that; if I live as long as he did, I will probably get it, too. There are some treatments (not cheap) but of course it would be better to delay or not to get the disease at all. But Blue Cross won't pay for Ocuvite because it's not a prescription drug.
For example, my eye doctor prescribed Ocuvite, shown by controlled, randomized studies to delay onset of age-related macular degeneration. My Dad had that; if I live as long as he did, I will probably get it, too. There are some treatments (not cheap) but of course it would be better to delay or not to get the disease at all. But Blue Cross won't pay for Ocuvite because it's not a prescription drug.
Why is that foolish? Because health insurers save a nickel today and spend ten dollars later; their business model requires that they be stingy regarding prevention but generous regarding cure.
I also saw this when
I worked as a tobacco cessation counselor.
My patients could not get reimbursed for the few hundreds of dollars cessation classes cost, but when they cost tens of thousands later for their lung and other cancers, heart disease, and COPD... no problem!
Why is it so? These short-sighted policies are demanded by how corporations work: they must show continually-rising short-term profits. This is done by minimizing expenditures in the present quarter. Higher costs in the future? They'll deal with that when the time comes. This is the behavior that's good for Wall Street, but it's bad for our health. The incentives are wrong. This is why -- by definition -- for-profit companies should not be in the business of making health care decisions. What would be a suitable alternative?
Single-payer, of course!
top
|
| |

December 19, 2010 --
Today was nursing school pinning (that's what nurses call graduation.)
Now I have the "N" in "RN"... To get the "R", I will soon take the
NCLEX, the State Board exam that gets me my license to actually do nursing
work.
 What's remarkable is how little we new grad nurses know about how
to do the work nurses do...
Especially given the $52K/yr we've spent to get here.
Hospitals are reluctant to hire us because we are nearly useless.
Hiring us is a big commitment because hospitals must
make such a big investment in us (lots of mentoring and
initially low productivity) to get us up to speed.
What's remarkable is how little we new grad nurses know about how
to do the work nurses do...
Especially given the $52K/yr we've spent to get here.
Hospitals are reluctant to hire us because we are nearly useless.
Hiring us is a big commitment because hospitals must
make such a big investment in us (lots of mentoring and
initially low productivity) to get us up to speed.
It doesn't need to be this way;
nursing education could be effective.
My school was mediocre but (and I have evidence for this)
they all are.
But that's a topic for a different discussion...
For now, I am just celebrating.
Hurray for pinning!
top
|
| |

December 12, 2010 --
In one week I will graduate from nursing school. At long last! The ceremony is called "pinning" and is a throwback to the old days when nurses wore little white hats and making tight hospital corners mattered more than patient care.
I am a new nurse, entering this as a second (well, third, but who's counting?) profession. I bring the perspective of experience in other work realms, and I have less tolerance for mediocrity than my fellow nursing school students who are half my age. More to the point, I have little tolerance for mediocrity in my nursing school faculty whom, to their chagrin, I perceive as peers (indeed, most are younger than me.)
Evidently there are many like me: older men entering nursing as a second profession. "Nearly 40 percent of students studying to become registered nurses are over age 30... candidates who already have four-year degrees," [from the New York Times, Nov. 7, 2010: 45, Male and Now a Nurse]. I'm not 45 but 56, and have both a four-year degree and a Master's, but the idea is the same. My nursing class exactly matches that in the NYT article: 15% male. What the article doesn't mention is the darker side of this trend: education to produce degrees like mine (the school sells BSNs) is now a big business. My school (which I'd better leave nameless for now, since I'm still in its clutches) is -- let's be magnanimous here -- lackluster in the quality of its teaching though expensive ($52,000/year not including books and supplies) and very profitable ($10M profit on $40M gross revenue).
Fortunately, the quality of the education is largely irrelevant to the quality of the nurses entering the profession. Most of what we new nurses need we will learn on the job, not in the classroom. In other words, we emerge from this expensive and unnecessarily fractious process knowing almost nothing of what we'll need to know to be good at our work. New nurses need lots of nurture from the institutions that accept them before they become useful.
This raises several important questions: how can nursing education be made effective? How can new nurses ("nurses eat their young") come up to speed without getting beaten up along the way?
Why does this matter? Because we want good health care. Given that the 3.2 million RNs now in practice form the vast majority of the health care work force, we need them to be good at their jobs and to get there quickly. The present dysfunctional system of producing new nurses is ripe for an overhaul. That will be good for us all.
top
|
| |

Dear diary (excerpts from my clinical journal)
In nursing school, the most valuable part of the process we undergo is the clinical rotations.
The clinicals are where the rubber meets the road.
Here, we work with live patients in local hospitals.
Each semester, we are assigned to a different type of
nursing unit so that by the end of the program we have
had a taste of med-surg (the most important), peds,
SNF, ICU, oncology, emergency, psych, telemetry,
a community clinic, and perhaps others.
These are fascinating, difficult, and stressful.
Some of us kept journals. I did. Here are my writings.
Feb. 18, 2010, Kaiser, med-surg, Santa Clara:
At the same time exhilarating and challenging is the access granted by nursing work. In ordinary human interactions, there isn't permission to poke and pry...
More
Feb. 23, 2010, Kaiser, med-surg, Santa Clara:
Infection transmission precautions are driving me nuts. Those bacteria have us whipped...
More
March 3, 2010, Kaiser, med-surg, Santa Clara:
I remember distinctly a comment made by one of my clinical instructors
from the first time I went to nursing school about four years ago. She
observed that I was having difficulty finding my "rhythm"...
More
March 17, 2010, Kaiser, med-surg, Santa Clara:
Nursing education is focused on the hospital setting with its enormous resources and fine-tuned protocols. What about nursing in other environments? ...
More
July 8, 2010, O'Conner Hospital, monitored (telemetry) med-surg unit, San Jose:
Listening is a challenge. I could not hear 9121's heart!...
More
July 17, 2010, O'Conner Hospital, monitored (telemetry) med-surg unit, San Jose:
Still have occasional moments of, "OMG what (of the hunded possible tasks) should I do next?" but they last only five seconds...
More
Aug. 23, 2010, Veteran's Administration Hospitals, Palo Alto and Menlo Park:
After all the flack in the press about the sorry state of affairs
at Walter Reed hospital and the right-wing excoriations of our
government's purported neglect of our brave men and women formerly
in uniform (i.e. veterans) it was eye-opening to see how well, in
fact, they are cared for...
More
Aug. 30, 2010, Veteran's Administration Hospital, Menlo Park:
I'll be blunt: the time doesn't feel very productive...
More
Sept. 13, 2010, Veteran's Administration Hospital, Menlo Park:
A couple of brief but illuminating patient interactions have given me pause. In the first, Mr. F., one of the more belligerent and combative patients...
More
Sept. 29, 2010, Veteran's Administration Hospital, Menlo Park:
On a personal note, at the risk of appearing unprofessional, I'd like to add that I felt at least a twinge of disappointment at my inability to "connect" with this patient...
More
Nov. 25, 2010, Emergency Dep't, Kaiser, South San Francisco:
Nursing is, of course, about people. As a student on this rotation I had the luxury of being able to take time to listen...
More
top
|
| |

December, 2010 --
Nurses carry information in their heads --
a lot of it! How do they remember everything they need to remember?
They use their brains!
This sounds silly but what nurses mean by the term "brain" is the piece of
paper they carry in their pocket on which they keep track of the zillion
patient and task details their job demands.
(Sharon McLane, MS, MBA, RN-BC, and now PhD of the University of Texas at Houston
documented this in her 2009 PhD dissertation,
Understanding Nurse Created Cognitive Artifacts.
"Cognitive artifact" is a fancy term for that piece of paper.)
I collect brains and you can see my collection in my
brain museum.
Each brain is in its own way clever and meets its
nurse-creator's memory needs. Fascinating... and brainy!
top
|
| |

December, 2010 -- This month I am completing my clinical rotations with a stint
in the emergency room of a major local hospital. I have seen some awfully sick people
walk in that automatic door or, worse, roll in on gurneys and wheelchairs.
It is sobering to see suffering, and gratifying to occasionally be
able to do something about it. Health care is like no other work in the world!
My friend and fellow
UCSF alumnus Mark Wandro
blogs about his lengthy and impressive experience as an emergency nurse.
Also fascinating is the Emergency
Nurses Association web site.
Good reading -- give them both a visit!
top
|
| |

Public option, public sector
November 19, 2010 -- Today I shook the hand of another of my heroes, California State Senator
Mark Leno.
He is a man of principle!
Part of my University (UCSF, where he spoke) is in his district.
Contrary to the loathsome and self-serving declarations of such right-wing demagogues as Grover
("shrink government to the size we can drown in a bathtub") Norquist,
the public sector, says Mr. Leno, is critically important. Not only because it is the best mechanism
for delivering such services as public safety and justice, but because without it there can be no revival
of the private sector. It creates the foundation upon which growth can occur. Around the world,
the countries where growth is limited are those with little infrastructure. And (dear to our UC hearts)
public education is a big part of any robust infrastructure. An educated middle class has been an
essential part of what has made California the world's eighth economy.
Mr. Leno has been instrumental in the revival of Sheila Kuehl's Senate Bill 840
(which, placating his monied friends, Governator Schwarzenegger twice vetoed) as SB 810.
Don't be fooled by the misinformation, Mr. Leno tells us -- no one is asking for "socialized medicine".
Rather, what we need is health care that continues to be privately provided but publicly funded.
Eliminate those middlemen, the health insurance companies, whose profit was $12B last year yet added
no value. Like me and a lot of people, he is convinced of the need for a single payer.
This is the only way to contain costs.
With Jerry Brown in the Governor's seat, Mr. Leno will reintroduce this bill. Will Mr. Brown sign it?
When he campaigned with Bill Clinton, Mr. Brown was a knowledgeable advocate for a single payer system.
As Governor he will no doubt feel pressure from the right and how he will respond is anyone's guess.
Expect, said Mr. Leno, a huge disinformation campaign from the insurance companies.
We must innoculate the public with education about single payer -- "Medicare for all" -- an idea
whose time has come and yet another opportunity for California to lead the nation.
Guided by visionaries like Mark Leno, we have hope once again.
top
|
| |

October, 2010 -- Calling all angels! Well, not all angels, just the right angel...
an angel with vision, insight into the challenges of health care, and that burning fervor to change the world.
Well, not the whole world but an important part (nursing) of an important part (health care) of the world.
What needs to change about nursing? It's a hard job (no surprise) with lots of details
to keep track of (ditto) and a zillion tasks nurses must remember to do (ditto ditto) yet
they get no help (whoops!) No one teaches (or has even thought much about) how nurses
can/should do time management and no one has provided tools to help with this...
until now!
What do angels have to do with it?
Our development time and marketing efforts could benefit from angel funding.
Are you the angel we seek? Get in touch... Let's do well while we do good.
Join the team and together let's change the world!
top
|
| |

Want a hero?
Or a checklist?
October, 2010 -- What do you want from your doctor, heroism or checklists?
Say you're going in for surgery.
Do you want your surgeon to exhibit "expert audacity"?
Here's how Atul Gawande describes it in The New Yorker, Dec. 10, 2007, in
The Checklist:
|
We have the means to make some of the most complex and dangerous work we do --
in surgery, emergency care, and I.C.U. medicine -- more effective than we ever thought possible.
But the prospect pushes against the traditional culture of medicine, with its central belief
that in situations of high risk and complexity what you want is a kind of expert audacity...
Checklists and standard operating procedures feel like exactly the opposite, and that's what rankles many people.
|
Or would you prefer that your surgeon follow a checklist as did
the pilot Sullenberger who brought down his failing passenger jet
in the Hudson River without losing a single passenger?
He said he was no hero but was well-trained and following the procedures.
We Americans love to say of our advanced medical care that we had the best doctor...
That our doctor is a genius... That a good outcome is thanks to that skill, that extraordinary person...
But this is not a model that scales well nor is it conducive to widespread good outcomes.
Only a few people get to be worked on by that genius.
And if evidence-based medicine is truly at work, then the "genius" is simply following the best evidence,
which every well-trained practitioner should do. (Here is Gawande in 1/29/2009 NEJM,
A Surgical Safety
Checklist to Reduce Morbidity and Mortality in a Global Population.)
Dr. Gawande says that medicine should be more like aviation -- no pilot would
fly without first running through his pre-flight checklist, and then using yet
another checklist for each situation and task that arises.
Checklists are so valuable that he has even made a checklist of
steps for making checklists.
Of Sullenberger he says:
...it wasn't flight ability, but instead adherence to discipline, and teamwork...
Because there were checklists, and because everybody used them...
The heroic part of that flight was not the flight ability of
Capt. Sullenberger, it was the willingness of the entire team
including the flight attendants, who... acted through their protocols.
For my doctor I don't want a hero.
It's time to end the culture of expert audacity.
I want a well-trained expert, equipped with the best evidence... and the best checklists!
top
|
| |

October, 2010 -- Environmentalism and nursing? What's the connection?
Turns out it's a strong one, and we learned about it at the
Children First: Promoting Ecological Health for the Whole Child conference at UCSF this month.
The intersection of environmentalism and nursing includes:
...nutrition, education, socio-economic status,
exposures to toxic chemicals, and access to preventive health care.
If you're a nurse -- you care for people -- how can you not be an
environmentalist?
Join us at www.enviRN.org.
top
|
| |

September, 2010
-- As nurses, how do we perceive the work we do?
This semester, my clinical rotation is in mental health ("psych") nursing.
One of the terms of art is patient compliance -- are they taking all their
pills? But we don't call it that any more. Now the preferred term is,
in the spirit of patient empowerment, adherence.
In other words, we prefer to think they take their pills by choice.
In her heart of hearts, though, the psych nurse will admit
misgivings about mental health care being little more than
polypharmacy.
Oh yes, and we don't call them patients anymore, either.
Now they're clients.
Perception is everything.
top
|
| |

August, 2010 -- The irony in this pair of billboards speaks for itself.
Thank you, Friends of Irony.
top
|
| |

Double mandate? Make it triple!
August, 2010 --
When we were arguing about health care reform, much was made
of the proposed double mandate.
This is the idea that the obligation is on both sides --
insurance companies could no longer turn anyone away,
and every health care consumer (you and me) is obliged to buy in.
For example, the Huffington Post says, in
A Double Mandate for
Health Works for Europe: "Most European countries mandate that every citizen must buy insurance coverage. They also mandate that every local insurance company who wants to do business in the country must sell coverage to any citizen who applies for that coverage. Health screens are not allowed."
This is eminently fair and reasonable.
The system works best when everyone participates.
But I propose we take it one more step.
I propose an even higher degree of fairness -- a triple
mandate: everyone must be covered, everyone must participate, and
everyone should pay the same.
Being young and healthy should not entitle you to a special price.
Most people are or were once young and healthy.
If you're sick you shouldn't have to pay more.
Sooner or later most of us get sick, at least somewhat.
Sure, some people won't be able to afford it.
So subsidize them with a government program.
We already have government programs to help people who
cannot afford health care; the cost of these programs would
stay the same or perhaps even decrease due to the larger
coverage pool. But this is a detail.
Here's the point:
We are a nation of realists; I help my neighbor knowing
that someday I may need the favor returned.
I do not deserve punishment for my health misfortunes and
neither do you. Sharing the risk makes us all stronger.
Sharing it equally is fairest.
And a system that is truly fair would be something for us all to be
proud of. Push for a triple mandate!
top
|
| |

Control your own medical data? Try it!
May, 2010 --
I am one of those "empowered" patients.
I labor under the illusion that I retain some
control of my medical data.
Try it yourself -- run this little experiment:
- Next time you get an order from your doctor for a routine lab test,
have him or her write the following instruction on the order:
"Send results directly and only to patient."
- Make sure your mailing address and fax number are included.
- Then find a lab that will perform as ordered.
Good luck!
Here in San Francisco I went to three different retail clinical labs
before I found one that was willing.
And even so it took some arm-twisting and remonstrating to convince
them that yes, they should do exactly as the order said...
no, they should not send the results to the doctor...
yes, they should send them (only) to me...
yes, it's legal...
yes, my insurance (Blue Cross) would reimburse as usual...
no, it's not a violation of anything, and...
it shouldn't even be unusual.
Yet it is.
Get with it, people!
Take possession of your own data!
Insist on it!
Of course you should share it with your doctor.
But it should be yours to share, in your control.
Our being empowered patients shouldn't be unusual.
It's time for the labs (and everyone else) to get used to us!
Postscript (two weeks later): Surprise.
The lab completely ignored the instructions
and sent the test results to the MD.
I have filed a HIPAA violation complaint.
Here are the
instructions and forms on the web site of
the U.S. Department of Health & Human Services
in case you, too, need to do this.
Stay tuned... I'll record any progress right here on this page.
Post-postscript (two months later): The Dep't of Health and Human
Services replied to my complaint.
They pointed out that the law says
that clinical lab test results must be provided only to the licensed
health care provider who ordered them. So the lab, in defying my
instructions was "right"... it's the law that's wrong!
Not only does the patient not own the data,
he/she doesn't even have the right to see
it unless the MD assents. Disempowerment
gets no worse than that. Broken laws? Let's fix them!
top
|
| |
Conformity and stethoscopes
May, 2010 --
Who is reluctant to try something new?
It's not whom you'd think.
Is it the oldsters, set in their ways? Guess again!
I recently called ThinkLabs with a technical question about
my new digital stethoscope.
The phone was answered by Clive Smith,
the inventor of the device and CEO of the company.
We proceeded to have an animated discussion about his
product and its users.
They're not whom you might have guessed:
younger, more experimentative healthcare practitioners.
On the contrary, said Mr. Smith, it's the older ones
who are willing to try something new.
Stethoscopes are a powerful cultural icon.
Wearing one around your neck is a kind of badge of honor.
Its appearance is determined more by
tradition than by function.
Like Leo Fender's cutaway electric guitar body
from whose shape few have dared deviate in 50 years,
stethoscopes must appear just so.
I can confirm Mr. Smith's statement.
My nursing school classmates all wear Littmanns.
They wouldn't dare try something slightly non-conformist
even if it worked much, much better.
Indeed, none of my classmates have even asked to try mine.
Yet the ThinkLabs is much, much better.

Imagine this: a volume control!
You have an obese patient and you can hardly
hear anything through that flesh?
Turn it up! What a concept!
By the way,
Nurse
Jackie wears a ThinkLabs.
This sounds like a commercial
but really what I'm describing is
the freedom of being an old-timer.
The youngsters don't feel free to experiment.
They are afraid to look different.
Mr. Smith faces a challenging obstacle.
top
|
| |

April, 2010 --
The California Healthcare Foundation reports in its
Survey: Nurses Divided on Whether EHRs Have Improved Patient Care
that half of nurses say that electronic health records have had "a positive
effect on the overall quality of care."
And then there's the other half.
My own experience -- now that I've worked with yet another
EHR (Kaiser's HealthConnect by Epic) on a few clinical rotations -- is that
nurses do spend an awful lot of time in front of the computer. This could
easily lead to the perception that it takes away from time with patients.
But is that true? Didn't they also spend a lot of time charting on paper before
there were electronic charts? And isn't it also true that record-keeping and
access is far better than it ever used to be? Especially with bar code
readers and the electronic Medications Administration Record (MAR) the chances
for errors are substantially reduced. So in this writer's humble opinion,
computerization has helped make nursing care a lot better.
Or at least half of it.
top
|
| |

April, 2010 --
Working my clinical rotations this semester I saw first-hand in the
suffering of a patient our medical system's dysfunctional approach
to pain management. This young man suffers from a gastrointestinal
condition that is painful and cannot be cured. Yet his doctors
will not give him ongoing opiate analgesics, the only thing that
enables him to get through a day relatively pain-free. They do
prescribe these drugs for his acute episodes but then they send
him home with non-opiates that, he says, "...do not touch the pain."
Evidently, the concern is that he might become addicted. But I
wonder, so what? He has the disease for life, why not the treatment
for it, too, for life? I cannot second-guess the doctors but I can
commiserate with his frustration.
top
|
| |

March, 2010 -- In another New York Times op ed entitled
Health Reform Myths,
Nobel prize-winning economist Paul Krugman points out three myths that bedevil proponents of health
care finance reform. Lots of people believe:
- President Obama is proposing a government takeover of one-sixth of the economy, the share of G.D.P. currently spent on health.
- The proposed reform does nothing to control costs.
- Health reform is fiscally irresponsible.
Go read the article
if you've fallen for any of these.
top
|
| |

Recognizing diabetes
March, 2010 --
We fledgling nurses spend a lot of our time dealing with diabetes.
It's grown to be an epidemic. I'm studying for an exam.
There will be questions about how to recognize it in our patients.
When you read the symptoms of a disease,
sometimes it seems like every disease has every symptom.
But anyway, here goes...
| Hypoglycemia | Hyperglycemia |
|---|
Fasting
Blood
Glucose | <60 | >100 |
|---|
| Onset | rapid | gradual |
|---|
| Skin | cool, pale, diaphoretic | warm, dry, flushed |
|---|
| Mental status | disoriented, comatose | awake, lethargic |
|---|
| Disposition | shaky, dizzy, agitated | hungry, blurred vision |
|---|
| Respiration | normal | deep, rapid, fruity odor |
|---|
| Pulse | normal or fast | fast, weak |
|---|
| BP | normal or high | normal or low |
|---|
| Seizure | common | uncommon |
|---|
| Urine | | polyuria |
|---|
| Thirst | | polydypsia |
|---|
| Treatment | PO or IV glucose | SQ or IV insulin, K+ |
|---|
| Recovery | rapid (minutes) | gradual (days) |
|---|
top
|
| |

A new stethoscope... and a sermon
March, 2010 --
I have decided to buy a fancy new stethoscope, one of the digital ones with ambient noise rejection
and other cool stuff... hurray! Maybe now those elusive murmurs will be a little less elusive.
Clive Smith, the CEO of the company (Thinklabs) that manufactures it has
a spirited blog.
He writes:
...let me make a prediction on healthcare reform. A bill will be passed, one way or another. Due to the special interests that have written this bill and influenced both parties, no "cost cutting measures" will be truly effective. Congress will mandate coverage of pre-existing conditions and many more people will have insurance coverage, which is a good thing. However, with no real cost cutting, insurance companies will skyrocket premiums, arguing that Congress forced them to provide all that new coverage. That the insurance companies wrote the laws will be forgotten.
Opponents of reform will argue that it was an abject failure due to skyrocketing costs. That these opponents of reform prevented cost-cutting measures to pass will be forgotten.
The people will complain that they wanted healthcare reform and cost cutting and instead, they got increased premiums and healthcare costs even more. That they, too, were supposedly opposed to healthcare reform and wanted no government intervention to contain costs will, too, be forgotten.
What will not be forgotten, by those who have tried to promote true healthcare reform, will be that they were painted as the enemy, they were maligned, and they were blamed for the outcome when the mob, influenced by special interests, attacked them for their efforts. What will not be forgotten is that trying to reform healthcare is a losing political position and it's not worth risking one's neck...
the politicization of this discussion, the hysteria, the lobbying money, and the abject ignorance of The People... resulted in the destruction of all rational thinking and analysis. We will all be the worse off for that sad outcome.
I like this guy. And I'm buying his product.
Health care financing may be a mess
but at least I'll be hearing my patients' insides better.
top
|
| |

Blame the Lawyers
Feb., 2010 --
My friends on the Right love to blame the lawyers.
Who doesn't?
In an Oct. 1, 2009 article in the
Los Angeles Times entitled
Tort reform is the healthcare debate's frivolous sideshow,
Michael Hiltzik writes:
You know the argument: Disgruntled patients, goaded on by unscrupulous lawyers, file frivolous malpractice lawsuits and walk off with millions of dollars in undeserved awards granted by teary-eyed jurors. Doctors respond by practicing "defensive medicine," ordering lots of unnecessary tests to cover their behinds. Bingo! Medical costs hit the stratosphere.
But then he goes on to dispel this myth.
The truth is that medical liability isn't a big driver of health costs... the cost of malpractice litigation, in court and through defensive medicine, [is] roughly 2% to 3% of all U.S. healthcare spending.
So the tort reform "talking point" is indeed a "frivolous sideshow."
Instead, let's focus on where we can make real change.
top
|
| |

Turkeys voting for Christmas
Jan., 2010 --
(Cross-cultural note for us Americans: in the UK, the traditional
Christmas dinner is turkey.)
A fascinating article by BBC contributor David Runciman entitled
Why do people often vote against their own interests?
reviews writings by Drew Westen and Thomas Frank about
the psychology of many American voters:
...it is striking that the people who most dislike the whole idea of healthcare reform - the ones who think it is socialist, godless, a step on the road to a police state - are often the ones it seems designed to help.
In Texas, where barely two-thirds of the population have full health insurance and over a fifth of all children have no cover at all, opposition to the legislation is currently running at 87%.
...Why are so many American voters enraged by attempts to change a horribly inefficient system that leaves them with premiums they often cannot afford?
Why are they manning the barricades to defend insurance companies that routinely deny claims and cancel policies?
The answer does not increase my respect for the decision-making processes of American voters. Westen's explanation is paraphrased:
...stories always trump statistics, which means the politician with the best stories is going to win: "One of the fallacies that politicians often have on the Left is that things are obvious, when they are not obvious.
"Obama's administration made a tremendous mistake by not immediately branding the economic collapse that we had just had as the Republicans' Depression, caused by the Bush administration's ideology of unregulated greed. The result is that now people blame him."
Paraphrasing Frank, the article observes:
...voters' preference for emotional engagement over reasonable argument has allowed the Republican Party to blind them to their own real interests.
The Republicans have learnt how to stoke up resentment against the patronising liberal elite, all those do-gooders who assume they know what poor people ought to be thinking.
Right-wing politics has become a vehicle for channelling this popular anger against intellectual snobs. The result is that many of America's poorest citizens have a deep emotional attachment to a party that serves the interests of its richest.
The article is part of a series entitled
Turkeys voting for Christmas... How apt.
top
|
| |

The Incentive that Works
Dec., 2009 --
The benefits of prescribing electronically ("e-prescribing")
are numerous:
- Fewer errors
- Fewer avoidable adverse drug events
- Decision support
- Detection of drug-drug interactions
- Improved record-keeping
- Faster communication with pharmacies
- And so on...
|
Indeed, e-prescribing is low-hanging fruit; many MDs have
adopted this practice and prescribe this way... But not
for the above reasons.
The true incentive? Money, of course.
The Centers for Medicare and Medicaid Services (CMS)
has implemented a program named MIPPA
(Medicare Improvements for Patients and Providers Act of 2008)
giving eligible e-prescribers an incentive payment of
2% of their Medicare Part B charges in 2009 and 2010.
All that quality-of-care stuff?
Do-no-harm stuff?
Nah! It's the green stuff that gets it done!
top
|
| |

Doctors? Businessmen? Or Both?
Nov., 2009 --
Reform of how we pay for healthcare is the hot topic of the day.
I myself have expounded on this
with excoriations of the health insurance industry.
Blue Shield, Anthem, Aetna, Humana and their ilk
are now everybody's favorite whipping boys and it's not undeserved.
The relationship of these companies with their customers is by definition adversarial.
They do their job "best" (in terms of profit-making)
when they succeed in denying health care.
But there is another, less obvious villain driving our costs up and our outcomes down:
doctors who are also businessmen.
I am not the first to recognize doctors' conflict of interest.
It has been documented in widely-circulated articles such as
NPR's
October 8, 2009 story, "The Telltale Wombs of Lewiston, Maine".
Another article on the same theme in June's New Yorker has also gotten a lot of attention.
Named The
Cost Conundrum, it observes that when MDs are businessmen, health care gets expensive.
Indeed, there is an entire science devoted to the analysis
of patterns of consumption of medical care and their effectiveness in terms of cost and and outcomes.
It's termed utilization review
and is naturally a topic of great interest to health care payers.
Why has it failed to bring to light these maldistributions of service? Why is this issue not part of today's debate?
The NPR story describes how "...in Lewiston, 70 percent of its women would have a hysterectomy by age 70."
The reason is not an unusually high rate of uterine disease;
a now-famous longitudinal study revealed that numerous communities around the country
have anomalous rates of certain medical procedures.
The study showed "...how bizarre the distribution of care was.
People in one town would get their hemorrhoids removed
five times more often than people in another town only 30 miles away.
Ditto with mastectomies, prostate operations, back surgery."
How are these anomalies explained?
It is doctors, not patients, who drive consumption of medical services.
Doctors who are paid for each service they render ("fee-for-service") tend to recommend those services to their patients.
In other words, money.
This is not to say that doctors are intentionally exploiting their patients
but it is clear that their objectivity and judgement is colored by their own financial interest.
"The U.S. health care payment system rewards doctors for taking action and doing procedures.
This reality is so powerful that it hasn't just changed the individual behavior of doctors...
the specialties themselves have changed, bending like flowers to the sun, moving toward the source of heat."
How should we solve this problem?
Neither article goes so far as to propose a solution but I will.
I propose that our healthcare payment reform legislation
include language to do away with medical fee-for-service.
A primary care doctor who also offers (and orders)
ancillary services or tertiary care
has, by definition, a conflict of interest.
Why is this a revelation?
Why hasn't it always been prohibited?
What should we do about it?
Here's what: put all doctors on salary instead.
They should be paid the same no matter how many (or how few) hysterectomies they perform.
Of course this is politically impossible.
The AMA and others would rebel and not mildly.
But I have seen other countries (e.g. Italy where I just came back
from living for a year and was most impressed by
the quality and equity of the healthcare system) where it works just fine.
For me personally, this conundrum has an additional dimension.
Among my closest friends are several doctors.
Some of them are quite entrepreneurial and thriving.
They work hard and well, and their ethics are impeccable.
They would not appreciate the sentiments I express here.
In conclusion, it can be said only that the healthcare debate is convoluted indeed.
top
|
| |
|
Gullibles, Libertarians, Partisans, Shills
Sept. 3, 2009 -- In a letter today to the
San Francisco Chronicle, I wrote:
Dear Editor,
In raucous town halls around the country, opponents to proposed
health care reforms seem mostly to fall into four categories that
I label as follows:
- The Gullibles -- listeners to right-wing talk radio screeds and outright fabrications such as Palin's death panels
- The Libertarians -- those who oppose government in any form or role and view its actions (except perhaps military and law enforcement) as intrusion and theft-by-taxation
- The Shills -- militant loudmouths delivered by buses paid for by Big Pharma and Big Insurance
- The Partisans -- those who hope to see Obama fail at any cost
(to these people, expense, outcomes, and
quality of life are irrelevant... all that matters is
Republicans "winning")
Every opinion deserves to be heard but now let's recognize the uninformed ones for what they are, move on, and get the job done!
Thanks for listening,
Dan Keller
PS -- They didn't publish it. Maybe next time.
top
|
| |

Jackie Speier Gets It!
Sept. 1, 2009 -- This evening, at a UCSF event to welcome our new Chancellor, we were
privileged to hear a brief talk by Congresswoman
Jackie Speier.
Her congressional district includes UCSF (where I am Pres. of the Graduate Division Alumni Association).
She welcomed Chancellor-elect Susan Desmond-Hellmann and talked about
the hot-button issue of the day: health care reform.
Of course, the issue is not so much health
care as health insurance.
The insurance company practices of rescission (canceling your policy when you get sick)
and pre-existing conditions
(if they suspect you might eventually need health care, they deny your application for coverage)
must, Speier said, be forbidden. She also supports the "public option"
-- the watered-down compromise (a proposed government-created non-profit health insurance provider,
a distant second to genuine single-payer health care) but perhaps the best we can get --
on which President Obama is backing down, under pressure from the richly-funded Big Pharma/Big
Insurance lobbyists and from the partisan, conservative talk show-driven agitators.
Rescission: no; pre-existing conditions: no; public option: yes. Speier gets it!
top
|
| |

How Do Italians Pay for It?
In 2008-2009 I am living in Italy and learning a lot.
Italy has much to be proud of,
including a health care system that in recent years
has improved in quality
to match that of nearly any western country.
In addition to its quality of care,
the Italian system is commendable
for its equality of distribution;
for all Italians (and often foreigners, too)
most procedures are covered.
Tests and prescription drugs
demand copayments but primary care and inpatient care are free.
The Italian National Health Service was established in 1978
by law number 833 (the Riforma
Sanitaria) whose preamble states that health care
is a human right and is to be delivered equally to all citizens.
However, the way public health care in Italy is paid for
is less fair.
Most of its funding comes from a payroll tax that is regressive;
regular employees bear a disproportionate burden.
The other sources of funding are the income taxes
and value-added (VAT) sales taxes collected
by the federal and regional (regioni) governments.
Equity of taxation is one of the
most contentious issues in Italian public life
and is, in my judgment, the one most responsible
for the resurgence of power of the right wing and Berlusconi.
From the provider standpoint, too, the medical system
is far from generous.
Compensation received by physicians and other providers
is based on capitation and is low relative to
that of providers in most western countries
and also relative to workloads.
Doctors here work hard!
Neither is the economics of Italian health care kind to hospitals.
Public funding of health care is doled out by the regioni.
The Lazio regione (which includes Rome,
where I live) has for the past
decade run an annual health care budget deficit of 1 billion Euros.
Hospitals are paid according to
diagnosis-related group (DRG) formulae,
as is done by Medicare in the USA.
Today, hospital budgets are shrinking and several of
Rome's most prominent are closing for lack of funding.
 For example,
Forlanini
hospital, one of Europe's most technologically-advanced and,
in recent years, the recipient of substantial infusions of
capital for equipment, is slated to close in March of
2009 for lack of operating funds.
My friend Maura who is a nurse on a respiratory rehab unit there
says she no longer has most of the drugs in the usual formulary
to dispense to their patients; patients are receiving
inferior care due to the cutbacks.
For example,
Forlanini
hospital, one of Europe's most technologically-advanced and,
in recent years, the recipient of substantial infusions of
capital for equipment, is slated to close in March of
2009 for lack of operating funds.
My friend Maura who is a nurse on a respiratory rehab unit there
says she no longer has most of the drugs in the usual formulary
to dispense to their patients; patients are receiving
inferior care due to the cutbacks.
Another
is San Giacomo hospital
(including its reknowned orthopedics unit) in the center of Rome,
which just last year had a 15 million Euro upgrade.
(In the photo: Sept. 25, 2008, police presence at a sit-in
to save San Giacomo. Note the protest banners.)
There is considerable outcry in the Italian press
but recent changes in governmental priorities make these
and other closures appear inevitable.
This is a great detriment to the healthcare options available to
Romans and Italians nationwide.
For an even less sympathetic view than mine, see
Tanner (Cato Institute), The Grass Is Not Always
Greener: A Look at National Health Care Systems
Around the World (but see below for
my opinion on those Cato whack jobs.)
For overviews of the economics of health care in other countries,
see Healthcare
Economist.
For Italy in particular, see Health Care Around the World: Italy.
top
|
| |

Google Health knows when you're sick
November, 2008 --
Google has discovered that it can detect influenza outbreaks
and other "...snapshots of what's on the public's collective mind"
by mining aggregated search data.
Using this data, they are several days
ahead of the federal Center for Disease Control (CDC) in
detecting disease trends.
In other words, when people get sick, they
search for terms like "flu symptoms" and many more.
And Google is paying attention.
You, too, can stay atop these trends via
Google
trends.
Watch flu trends and more...
As Google says,
"Google search isn't just about looking up football scores
from last weekend or finding a great hotel for your next vacation.
It can also be used for the public good."
Do you agree? Draw your own conclusions.
top
|
| |

How Do Americans Pay for It?
March, 2008 -- In America, most health care insurance premiums are paid
by employers. Workers receive them as a job benefit.
There are several problems with the American scheme.
The first problem is that the cost to employers rises
with each new employee they hire.
(Increasingly, this cost is also born by the employee
who today is often asked to share it, but that is
a topic for another discussion.)
Thus, it is a kind of employment tax.
Enlightened tax policy is driven by decisions about activities
that, for the good of society, we want to discourage.
For example, we have
sin
taxes to discourage consumption of tobacco and alcohol.
Employment is not one of those!
We want to encourage employers to do it!
Thus, if we could find another way to fund health care in America,
we could have more jobs. Who would argue against that?
Another problem is that in this system only employed people
(and the relatives thereof) are covered.
When the economy is strong and provides full employment,
coverage almost suffices but in leaner times,
even more are left out.
Indeed, no one must be left out, in lean times or good.
top
|
| |

When is health care reform not health
care reform?
June, 2009 -- When it's a snow job. (Thanks to Ron Knox, Sun, 07 Jun 2009,
for this item.) See: How Pharma and Insurance Intend to Kill the Public Option, And What Obama and the Rest of Us Must Do.
Note the new term of art... we no longer talk
about a "single payer".
Now it's "the public option."
Senator Olivia Snowe, "...well-respected and considered
non-partisan, and [who] therefore offers some cover to Democrats
who may need it" has proposed a Byzantine set of conditions
under which "the public option" can take place and
probably won't. In other words, she and her cronies
can look like they're fixing our desperately broken system
while in reality defending Big Insurance/Big Pharma's hegemony.
Robert Reich has it right:
"Big Pharma and Big Insurance are gaining ground
in their campaign to kill the public option in
the emerging health care bill."
It's time for Ms. Snowe to get out of the way
and for government to step in and make sure
we all get the health care we need, at prices we can afford,
paid for fairly and equitably. No Snowe jobs!
top
|
| |

Unfair Advantages? Now We're Getting Somewhere!
In a Jan. 16,
2009 Herald Tribune article entitled Bipartisan Reform
Vowed on Healthcare Daschle Calls the System Unsustainable
some partisan hack named James Gelfand is quoted as saying,
in regard to Obama's plan to reform health care:
"The public plan option is a terrible idea - one of our top
concerns in the health reform debate..."
Well, ok, he's not just a hack, he's senior manager of
health policy at the United States Chamber of Commerce.
And he's a shill for the insurance industry, giving a
thinly-disguised defense of entrenched interests.
If he'd finished the sentence, it would have been,
"It might put some of my clients out of business!"
The article goes on,
...the proposal is anathema to many insurers,
employers and Republicans.
They say the government plan would have unfair advantages,
[emphasis mine]
like the ability to impose lower fees,
and could eventually attract so many customers
that private insurers would be driven from the market.
Um, lower fees? Isn't that the point?
Not for Mr. Gelfand.
top
|
| |

Surprised! ...Again
February, 2008 -- Many healthcare procedures are routine,
e.g. immunizations for kids and the
every-5-years-after-age-50-colonoscopy.
If your doctor is doing her job, these
are ordered for you
at entirely predictable times in your life.
Every American should be getting them.
Budgeting and resource allocation for these things can
(and should) be rational and planned. Why aren't they?
In our present system, they seem to be surprises every time.
We must submit lengthy paperwork for insurance claims,
argue about what's covered, etc. Ridiculous.
Furthermore, there should be routine tracks for the various
chronic illnesses (with variations planned for differing degrees
of severity, complicating factors, and responses to treatment)
according to plans derived from medical evidence
(best practices based on outcomes).
It's silly that the predictable, plan-able procedures should be
regarded (from a financial standpoint) the same as the
unpredictable ones. Why are the paperwork and eligibility
issues the same for a vaccination as for a broken bone?
Money to pay for routine medical procedures should be
budgeted for each of us from birth.
These procedures
should be paid for by a fund that's managed conservatively
and whose inputs are known precisely because its outputs are.
A second fund would cover non-routine healthcare,
i.e. accidents and acute diseases.
The outputs of this fund are known less precisely
yet can be predicted by actuarial techniques.
Both funds should be fed from a progressive taxation mechanism.
"To each according to need, from each according to ability."
Yet we do none of this.
It's hard to believe that we continue to be so financially naive
about healthcare!
top
|
| |

A Medical System to be Proud Of? No, One to be Ashamed Of!
December, 2007 -- How is it we Americans are so brainwashed about our medical care?
Why do the candidates for public office tout our system as the
world's finest... with straight faces?
"What is particularly shameful is how poorly this country
compares with other industrialized countries.
In 1960, the United States ranked 12th lowest
in the world in infant mortality.
By 2004, the last year for which comparative data are available,
it had dropped to 29th, tied with Poland and Slovakia."
[The New York Times Op Ed
piece, Oct. 18, 2008.]
Traditionally, the quality of a country's health care is measured
by three criteria:
- Life expectancy
- Morbidity
- Infant mortality
It
has been argued that,
"...life expectancy and infant mortality are both
poor measures of the efficacy of a health care system
because they are influenced by many factors
that are unrelated to the quality and
accessibility of medical care."
Nonetheless, health care outcomes in America remain unacceptable.
The NYT concludes, "The chief lesson we draw is that the American health care system, despite the highest expenditures in the world, is badly in need of an overhaul."
top
|
| |

Medicine in the Post-Oil World
Strategies for Delivering Medical Care
In a World without Cheap Energy
(" Powerdown Medicine")
January, 2007 -- I'm just getting started thinking about this...
And I'm not the only one.
Johnston et al, in
Modern Medicine And Fossil Fuel Resources
observe that the story of oil in the 21st century
is like that of the boy who cried wolf, the point being
that finally the wolf did come.
Walter Youngquist writes in The
post-petroleum paradigm -- and population:
Reaching and passing the peak of world oil production will be the
most important happening in human history to date,
affecting more people in more ways than any other event.
It will happen, and during the lives of most people now living.
Johnston continues this theme:
Increasing scarcity and expense of fossil fuels will present
medicine with great challenges, especially at its high-tech end...
Petroleum-based products are used all throughout the medical sector.
Following these lines of thought, various corollaries suggest
themselves...

- High-tech interventions will be available only to a
shrinking elite.
- Community and locality will grow in importance.
- In medical care, labor will overtake capital (the way
it does in the third world).
- There will be fewer disposables and more reuse.
When oil is scarce, plastic is expensive.
- Let's learn from the Cubans. I intend to travel there.
This will be a reverse foreign aid mission --
the evidence says these folks are the experts.
(Ahem, I thought of this before Michael Moore did.)
- It won't be all bad -- if we're smart about it, we'll
use it as an opportunity to emphasize lifestyle and prevention.
When healthcare technology gets scarce,
it will be better not to get sick in the first place.
Lots of work to be done!
top
|
| |
 Chronic Disease Management Systems
Chronic Disease Management Systems
Technology is not just an expensive frill.
Used well, it can make a genuine difference not only in the high-tech hospital
but in the daily lives of people with chronic diseases:
asthma, diabetes, hypertension, and others.
Such tools can help to:
- Automate recall processes
- Incorporate risk factors and lab test results in decision-making
- Enable quality improvement based on data analysis that far exceeds
what could until now be achieved only through traditional chart audits.
Here is an excellent article on how
these are done at four community clinics.
top
|
| |
 I've been blogging lately...
I've been blogging lately...
And I agree with
what
Russell Mokhiber says about "...the war between the American
people and the health insurance industry." [SleptOn Magazine, Sept.
19, 2007]
top
|
|
Eliminating the middle man does not
mean "socialized medicine"!
Health insurance is not to be confused with health care.
It is a distinct industry.
And it is a parasitic one.
It is expensive yet it creates no value.
We need to shut it down.
Defenders of the status quo use scare tactics (see
Krugman, above) to defend their hegemony.
But common sense dictates otherwise.
"[This] bureaucracy consumes 31 percent of health spending,
versus 17 percent in Canada.
The difference translates into $350 billion
frittered away annually here, where a million healthcare
workers, as well as hundreds of thousands in the insurance
industry, spend their days on useless paperwork.
"This waste is a natural byproduct of private insurance.
Private plan overhead is eleven times that of Canada's NHI
program. Each dollar spent on private premiums buys only
78 cents of care; the rest pays for insurer's marketing,
underwriting, utilization review and profits -- and for
the billions paid to their CEOs. Fragmented coverage also
means duplication of claims-processing facilities and
mountains of paperwork for doctors and hospitals, which
must deal with multiple insurance products each with its
own eligibility rules, co-payments, referral networks,
etc. -- tasks that are absent in Canada. Our multiplicity
of insurers also precludes the payment to hospitals of a
global, lump-sum budget. In Canada, global budgets
obviate the need for most hospital billing and much of the
internal accounting needed to attribute costs to
individual patients and payers."
The Nation, April 14, 2008.
Cartoon by my Dad, Charles Keller.
(Yes, that's Jimmy Carter...
Our health care dysfunction is not a new problem.)
top
|
| |

Yes on California Senate Bill 840!
Up for a vote soon in our
state legislature will be Senate Bill 840, crafted by
State Senator Sheila Kuehl.
It proposes to replace the
existing expensive and dysfunctional private health
insurance scheme -- what you have if you're well-off in
America -- with a State-administered one.
No doubt the
powerful insurance lobby and media machine will trot out
the tired nostrums about socialism, government
inefficiency, and the boogeyman of state-run healthcare.
The truth is that around 25 cents of every dollar we
spend on healthcare goes to the insurance company
bureaucracy, not for medicines, hospitals or doctors.
If
we're concerned about rising costs (and who isn't?) then
eliminating this overhead is an obvious strategy for cost
control.
Furthermore, the federal Medicare program -- one
of the most popular public programs of all time -- has
proven that in overseeing the delivery of healthcare,
government can be both effective and efficient. Medicare
recipients (my parents, for example) are pleased with
their care, and the overhead is less than 2%.
Of course, if you're not well-off in America, then what
you have for healthcare is zilch.
Yes, emergency rooms
are required by law to serve everyone who walks in the
door. But it is undeniable that there are two tiers of
patients -- I have worked in several hospitals and I've
seen it with my own eyes.
Patients without coverage
really do get inferior care. The incentive to the
hospital to push those patients back out the door is
irresistible. If the hospital is lucky, some county money
will help cover the cost. More likely, the hospital will
eat it itself.
In the end, we all pay because the
hospital must charge its paying customers enough to stay
in business. And this is the second breakthrough offered
by SB 840: universal coverage.
Similar bills have twice before been passed. And twice
our Governor has vetoed them.
Why would populist
Governor Schwarzenegger
oppose such an obviously smart move for the
people of the State of California? To save the jobs of
his insurance company friends and their powerful lobbies
in Sacramento (our state capital).
Let's hope that this
time the legislature will override him. And let
California lead the country with a healthcare system that
is affordable yet leaves no one out.
Postscript: With little fanfare and barely a mention in the press,
on Sept. 30, 2008,
Governor Schwarzenegger
vetoed SB 840. He defended
this action saying that he could not support "...a bill that places
an annual shortfall of over $40 billion on our state's economy."
Chalk up another one for the lobbyists of Anthem (Blue Cross),
Blue Shield, Aetna, Humana, Kaiser, Unicare...
top
|
| > |
 That Is Sick!
That Is Sick!
Jan. 11, 2006 -- In our sick healthcare system:
- Amputating a diabetic's foot is profitable.
- Delivering the preventive care that could have saved
the foot loses money.
- See the January 11, 2006 New York Times:
In the Treatment of Diabetes, Success Often Does Not Pay:
In "...the byzantine world of American health care,
...the real profit is made not by controlling chronic diseases
like diabetes but by treating their many complications.
Insurers, for example, will often refuse to pay $150 for a
diabetic to see a podiatrist, who can help prevent foot
ailments associated with the disease. Nearly all of them,
though, cover amputations, which typically cost more than
$30,000."
top
|
|
 No Butts
No Butts
In my work as a smoking cessation counselor
(please see my web site,
www.tobaccoteacher.com)
I see this short-sighted policy in insurance companies
that pay tens of thousands of dollars for radiation and chemotherapy
but not mere hundreds of dollars
for smoking cessation classes and nicotine
replacements (patches and gum).
Our own
Governor Schwarzenegger
in 2005 vetoed
(despite my letter)
legislation that would have required them to pay for these
sensible preventive measures, bowing to their powerful lobbies
and their "logic":
"By the time a situation is acute...
the insurer, which has been
gambling on never being asked to cover procedures that far
down the road, has little choice but to cover them, if only to
avoid lawsuits, analysts said." [NYT]
In other words, the thinking goes: "We won't pay for prevention
because by the time you get sick you'll be somebody else's
customer or dead."
This is why healthcare does not belong in the
domain of private business. The short-term thinking demanded by
performance for stockholders leads to poor decisions like these.
Only public institutions have the capacity to make decisions
driven by long-term considerations.
Thus, though it's enlightened public policy, spending on
preventive care will always be shunned by corporate (private)
decision-makers.
Conclusion:
Single-payer healthcare is better for our health!
top
|
| |

The Medical-Industrial Complex
One of my heroes, Paul Krugman (winner of the 2008
Nobel prize
in economics) writes in the
New York Times
on 7/9/7 regarding Michael Moore's Sicko
and the Canadian healthcare system:
For more than 60 years, the
medical-industrial complex and its political allies have used
scare tactics to prevent America from following its conscience
and making access to health care a right for all citizens...
Yes, Canadians wait longer than insured
Americans for elective surgery. But overall, the average
Canadian's access to health care is as good as that of the
average insured American -- and much better than that of
uninsured Americans, many of whom never receive needed care at
all.
The only things standing in the way of
universal health care are the fear-mongering and
influence-buying of interest groups. If we can't overcome
those forces here, there's not much hope for America's future.
top
|
| |

Homework-O-Matic
Here's my
Arterial Blood Gas (ABG) Analysis homework-o-matic.
Hey all you fellow-nursing-classmates, have at it!
top
|
| |

Nosocomial Infections
Hospitals are dangerous places. Here are some of the things you
can catch there. You probably wouldn't catch them anywhere
else... and the probability there is surprisingly high.
Only recently have a very few hospitals begun to report the rates
of these infections. Such reporting should be required!
- Ventilator-associated pneumonia
- Bloodstream infections caused by catheters
- Methicillin-resistant staphylococcus aureus (MRSA) --
Causes an "alarming
number of infections and a very significant number of
deaths." This bug kills more Americans each year
than does HIV. The primary vector? The unwashed hands of
healthcare workers.
- Surgical site infections
- Clostridium difficile ("C-diff"), a bacterium that causes
severe colon infection and stomach pain
And infections are only part of the story.
Here are more preventable bad things that happened to hospital patients
(in California during the period July 2007 to May 2008
as reported by the Los Angeles Times on 6/30/08):
- Severe bedsores (466 patients)
- Foreign objects such as surgical equipment left inside (145 patients)
- Died under anesthesia (34 patients)
- Wrong procedure or operated on the wrong body part or patient (41 patients)
This is not to blame the caregivers or the organizations in all cases;
it's to point out that the delivery of healthcare is complex and near-impossible
to do with total reliability. There are no easy solutions.
top
|
| |

Paradigm shifts are happening and quality is rising.
Here, excerpted from
Reflections on Nursing Leadership (Fourth Quarter 2005)
is the most succinct statement I've seen of...
Healthcare's shifting paradigms
From process orientation (what professional is doing)
To outcomes orientation (value of what professional is doing)
From focus on provider-patient relationship
To focus on work setting as a learning organization
From do no harm as an individual responsibility
To safety as a system concern
From caregiving that is time and place bound
To caregiving with time and place limitations removed
From focus of care that emphasizes patient compliance
To focus of care that emphasizes best practices
From workarounds being the norm
To crucial conversations being the norm
From decision making based on training and experience
To evidence-based decision making
From organizations that encourage professional silos
To organizations that encourage interdisciplinary collaboration
From seeking cost reductions
To continuously decreasing waste
From emphasis on discharge planning
To emphasis on lifestyle change
top
|
| |
 Neurosurgery
Neurosurgery
Mission
to
Vietnam
I've been helping Dr. Gary Heit to run his nonprofit,
Americare Neurosurgery
International.
In March, 2008, we ran our third medical mission,
this time to Hue, Vietnam.
Quite literally, we saved lives.
Gary is an amazing neurosurgeon!
top
|
| |

Obama Gets It!
In a January 8, 2009 article,
Health Data Management reports:
In a major speech on Jan. 8 to push his
forthcoming economic stimulus package,
President-elect Barack Obama pledged to have
all medical records electronic within five years.
"To improve the quality of our health care
while lowering its costs, we will make the immediate investments
necessary to ensure that within five years,
all of America's medical records are computerized," Obama said.
We applaud!
The image on the left was not associated with
the Health Data Management article;
it is included here for your amusement.
It is an example
of the disinformation and fear-mongering -- much like the entrenched
interests did to Hillarycare -- that is being ramped up once again
by the forces that continue to oppose (for narrow self-interest only)
these moves toward progress.
The unspoken sub-text is beware (so-called)
socialized medicine.
top
|
| |
 Kucinich Gets It!
Kucinich Gets It!
"Health care for all," he says.
"Insurance companies make money not providing health care.
As the co-author of HR 676,
a universal, single-payer, not-for-profit health care system,
Medicare for All,
I understand millions of Americans want health care that is accessible
and affordable."
Medicare for All -- what a concept!
"Medicare for All will help businesses large and small,
create jobs as well as save the jobs of thousands of people
including those of doctors, nurses
and other healthcare workers who are currently leaving medicine because it
is run by the insurance companies.
1 in every 3 dollars of the $2.4 trillion spent annually in America
for health care goes to the insurance companies.
If we take that money ($800 billion in unproductive wasteful spending)
and put it directly into care, we will have
enough money to cover everyone.
We are already paying for Medicare for all, but not receiving it.
HR 676 changes that!"
He also proposes to end the Medicare Part D boondoggle
and go to the heart of the problem: getting drugs to
the people who need them:
"[I have proposed a] Prescription Drug Benefit for Seniors,
HR 6800,
the MEDS Act, which provides a fully paid prescription drug benefit,
under Medicare, for all seniors.
I wrote this bill to help alleviate the
economic pressure that comes from the high cost of prescription drugs.
We can pay for it by letting the government
negotiate drug prices with the
pharmaceutical companies as well as by permitting re-importation."
Hard to believe that this is considered radical... It's
common sense to me.
top
|
| |
 Gore Gets It!
Gore Gets It!
And not just about the environment.
Here he is, speaking in favor of universal health care
coverage. Go Al!
top
|
| |
 Gavin Gets It!
Gavin Gets It!
Mayor Gavin Newsom has launched a program
that makes me proud to be a San Franciscan. In
his words:
We are still the first and only city in America on its way to universal health care.
Our Healthy
San Francisco program has already enrolled nearly
30,000 previously uninsured San Franciscans into a comprehensive health access program.
While the state and nation falter on health care - San Francisco is showing the way.
But there's more. In my opinion, the most radical aspect of this program is
that it provides health care, not health insurance.
In other words, our public health service in San Francisco
funds the providers directly. No middlemen! Brilliant!
top
|
| |
|
That's right. You don't.
Who does? Usually, the hospital, clinic, or doctor
who created the data.
In other words, not you.
Here is an excerpt from
Physician's
News Digest, March 1999:
Underlying the entire health care informatics industry is
the basic issue of who owns data and how data may be used
by others. There is limited public law on this question
and parties almost invariably address the issue as a
matter of private agreement. Generally, the law in most
states gives ownership of the medical and business records
to the provider who creates the records, subject to a
general duty of confidentiality and in some states a right
of access for patients to their own records.
These issues are partly addressed by the Federal law known as
HIPAA,
the Health Insurance Portability and Accountability Act of 1996.
It says that you have these five rights regarding
your medical records:
- An unconditional right to be informed of the
data-handling practices of medical practitioners and providers;
- The right to request, but not necessarily to
always obtain completely, the privacy protection of your
healthcare information;
- The right to review and copy your medical record;
- The right to request that inaccuracies in your record be
corrected; and
- The right to know who has
accessed your medical records in the past.
The text of the HIPAA law can be found at the US
Department of Health and Human Services.
It does not actually discuss ownership of medical data,
only access to it and control of it.
Decisions about ownership are left to the states.
Kate Jackson writes in Whose
Medical Record Is It, Anyway?
in For the Record magazine:
It may vary somewhat by state law, but the healthcare
record is owned by the healthcare provider that created
it... [You] generally have the right to see and request a
copy of [your] entire medical record. The exceptions to
that rule are records pertaining to psychiatric
conditions, HIV status, and mental health care...
[complete list]
most states consider psychiatric records to be
"hyperconfidential".
And they can charge you for making the photocopy...
of their data.
top
|
| |

Go Aussies!
Imagine having the peace of mind that comes from knowing
that you can always afford health care,
that your insurer can never cut you off (or deny you
coverage in the first place) if
you get sick (and expensive) or they suddenly "discover" a
"pre-existing condition." This is insane! Life itself is a
"pre-existing condition"!
Imagine that, no matter what, you could
always have the healthcare you need.
They get it in Australia. Go Aussies!
top
|
| |
 Beat It
Beat It
Some heart sounds
for our nursing class to learn.
top
|
| |
 Higher Education: Revolution Needed
Higher Education: Revolution Needed
Sept. 2005 --
The teaching that's done in colleges and universities stinks!
I offer some solutions.
top
|
| |
 USHealthCrisis.com: Another One for Francine
USHealthCrisis.com: Another One for Francine
In yet another brilliant move, Francine Hardaway has created
USHealthCrisis.com,
a web site whose purpose, in her words, is to:
...bring about health care reform.
If you have a story [about a failure of the US healthcare or health
insurance system] please post it to the
site, and tag it patient, provider, or payer.
We are aggregating this information and will take
it to the Obama administration. Right now,
reprepresentative stories will be a big help.
top
|
| |
 Getting Clear about Single Payer
Getting Clear about Single Payer
Francine Hardaway writes
a fascinating and often
brilliant blog in which the topics are sometimes medical:
Rarely do I disagree with her, but I did when, in 2007, she wrote:
I don't think we will accept a single payer system, because that's
just another way to say "rationing health care."
Here's my reply.
What does "single payer" really mean?
The significance of
the number of payers is that when there is more than
one, the incentive structure changes. The rewards no
longer go to those who provide prevention and care.
They go to those who stick the other guy with the bill.
We already do have rationing, Francine. Every country
and every system has rationing; it has to. There's
always a gatekeeper (as it's called in the UK, where
health care is provided primarily by public funding.)
Why ration? Because resources are finite.
Many people are frightened by the idea of gatekeeping
by governmental agencies. Consider, though, that
the activities of government are subject to the scrutiny
of we who elect them; they don't have the impunity of
corporations that operate behind closed doors.
Corporations are beholden primarily to stockholders.
To them, doing a good job means increasing the dividend each quarter.
Over corporate officers and management the public has even less
control than they do over governmental officials.
As long as we have a democracy, I prefer that gatekeeping be done by
government, thank you.
The problem with our system is that with multiple
payers, we have an additional, unproductive layer of
bureaucracy -- all those insurance company claims
adjusters who do their jobs "best" when they deny
treatments, drugs, and care.
They're not evil people but what they do is evil
because the incentives are wrong.
Insurance companies add 15-25%
(depending on whose numbers you use)
to the cost of our healthcare.
Yes, there must be rationing.
But the rationing process needn't be so expensive.
Eliminating these middlemen is unlikely, alas.
They command huge resources and their lobbies
are powerful. To protect their bottom line, they run
vast disinformation campaigns and promote myths
such as the one Francine has voiced. And their job
is to ration.
But don't take my word for it...
Here is an op-ed piece from the New York Times on
March 28th, 2006:
U.S. Should Implement
Government-Sponsored, Single-Payer System.
top
|
| |
 The Electronic Medical Record (EMR): Still Waiting
The Electronic Medical Record (EMR): Still Waiting
Rates of adoption of EMRs in the United States continue to be
abysmal. Here are some recent numbers (per the California
Healthcare Foundation's Snapshot:
The State of Health Information Technology in California,
2008):
- Just 12% of California physicians use alerts to warn them
about potential adverse drug events, receive electronic
warnings about abnormal lab results, and send reminder notices
to patients about regular or preventive follow-up care.
- Only 25% of hospitals are using bar-coding technology
fully for tracking lab specimens and only 13% have implemented
EMRs.
- Many patients do not communicate with their physicians
online because they are concerned that on the
Internet their privacy might be compromised.
Nearly three-quarters of medical groups in California continue to
rely on paper records.
Healthcare information Technology (HIT) offers substantial,
well-documented benefits both to reduce costs and to increase
quality. Why aren't we using it?
The EMR has always been a focal point of my
career. When I graduated from UCSF in 1983 with an MS degree in
this area (having built a rudimentary EMR for my master's thesis)
there were no jobs where I could put these skills to work.
But that has changed.
Today medical informatics is an industry. For example, both of my
recent hospital employers -- Sutter Health and Kaiser Permanente
-- have huge EMR implementation projects underway. Several
doctors I know are investigating EMRs for their offices.
However, industry-wide standards remain largely absent and paper
charts remain the norm.
We're still waiting for the revolution.
top
|
| |
 Doesn't Compute
Doesn't Compute
One of the places where I have worked as a volunteer was a post-op and
orthopedic floor high up in a tall tower in a hospital that shall remain
nameless.
In this hospital (and, I suspect, in most)
the manual, paper-based procedure
for reviewing and renewing medication orders
is stunningly labor-intensive and error-prone.
This is a task for which computer implementation would be ideally suited.
It is astonishing to me that this hasn't been done.
Here's how it works today:
In the MAR (Medication Administration Record)
portion of a patient's chart there are two sheets:
- PRN (drugs administered on an as-needed basis)
and One Time Medication Record
- Routine Medication Record.
Each has seven rows (one row for each medication that has been ordered)
and five columns (one for each of five days, e.g. Oct. 5-10).
In each cell, the nurse records the administration of a med on a date.
(For meds that are administered several times per day,
the cells can accommodate several entries.)
On each fifth day of each patient's hospital stay,
the nursing station secretary must see that
the form is full and must complete a new form,
copying from the old one all the following information:
- Patient allergies and contra-indications
- All the drugs, their routes, dosages, schedules, and formulations.
The probability of error is high, so the work must be checked by a nurse.
The only possible reason I can see for
lack of automation of this procedure is to
guarantee that it periodically gets a pair of eyes
to review the medication orders.
But are the secretary's eyes qualified to perform this review?
Is five days the right review period or just the number of columns
that fit on the page?
Is the labor cost justified?
Have errors ever been caught this way?
If indeed there does appear to be something
dubious about a drug order,
is there a mechanism for having it reviewed
(and perhaps modified) by a doctor,
especially the doc who made the order in the first place?
I suspect the answers to these questions are mostly no.
top
|
| |
 Providing Emotional Support
Providing Emotional Support
Another place where I volunteered is
San Francisco's HIV / AIDS/ HepC Nightline,
a department of San Francisco Suicide Prevention.
It is a telephone-based emotional support service.
Training to become qualified to deliver this service is
a couple of months of weekly evening classes.
The work itself is surprisingly challenging
but uniquely rewarding and I learned a lot.
An essential skill is listening without attempting to problem-solve.
Your job is simply to listen.
Often that's the best therapy in the moment.
People who are struggling need an ear that hears them.
It's something that's in surprisingly short supply.
And there was lots more.
Here are my notes and observations.
top
|
| |
 Don't Just Protect Me, Put Me in Charge!
Don't Just Protect Me, Put Me in Charge!
Privacy will always be a major concern regarding medical data.
One of the ways in which patients will be empowered by EMRs/PHRs is
by having explicit control over access. While
HIPAA
goes a long way
toward protecting privacy, it leaves the actual enforcement
in the hands of the caregivers and their institutions. Under today's system,
the patient is protected but not in control. This must change.
Here are the aspects of personal health records generally
considered most sensitive:
- Alcohol and substance abuse
- Biometric information
- Child or adult abuse or neglect, including sexual assault
- Communicable diseases
- Genetic information
- HIV/AIDS
- Mental health
- Minors' information
- Prescriptions
- Reproductive health including pregnancy
- Sexually transmitted diseases
With the electronic medical record system we need,
the patient will be the owner of the data (see What
Do You Mean I Don't Own My Own Medical Data? above)
and will have complete control over who sees it and which
parts are withheld from whom.
In other words, don't just protect me.
HIPAA does that and that's good but it's not enough.
Put me in charge! Let me decide where that data
goes... and doesn't go.
top
|
| |

Health Sites
In
a January 7, 2009 article, the Wall Street Journal reports
on a crop of new and increasingly useful web sites
for people seeking (and collecting and sharing)
information about health care, especially their own.
These include:
The article offers a good collection of links and brief site reviews for the informed patient.
top
|
| |
 Google Gets It
Google Gets It
Google says (and
I do not doubt it) that the most commonly-sought information on the Web regards health.
So it's a no-brainer that their business should do a good job of helping
their users find what they seek.
Though medical data searching is huge, what's at stake is even bigger.
The data to be managed is not
just generic -- diseases, treatments, research, institutions, services, etc.
It's also each of our personal medical histories, status, progress, and plans.
She who controls the data controls the process.
Empower the patient.
And be the supplier of that power. Thus,
Google Health.
Great strategy!
top
|
| |
 Help for Nurses On the Job
Help for Nurses On the Job
April, 2006 -- In my two years of nursing training I learned many things.
One was that it's a hard job, sometimes unnecessarily so.
Here's one of my ideas
about how to fix that.
top
|
| |
 The Art of Volunteering
The Art of Volunteering
In the years leading up to my nursing school stint,
I volunteered in lots of San Francisco
hospitals, clinics, and healthcare services.
You don't just walk in the door and magically transform lives...
There's an art to it.
Most important are the things that -- even with the best of intentions --
you must never do. A volunteer must never:
- Do anything invasive
- Give medical advice or information to a patient or family
- Give food or water without authorization
- Tell a family that a patient has died
- Make judgements about lifestyle, esp. domestic violence
- Handle controlled substances
- Help break up a fight or restrain a patient
- Do schoolwork in the ER
- Read medical records
Here are more thoughts on my experiences as a volunteer...
top
|
| |
 Pritikin's Still Got It!
Pritikin's Still Got It!
June, 2006 -- Concerned about health, fitness, longevity, weight loss?
Pritikin is the diet that works. Here it is in a nutshell.
- Choose foods that are big in size but small in calories. Avoid calorie density.
- Choose unrefined carbohydrates that are naturally rich
in fiber and water: fruits, vegetables, beans, whole grains.
- Avoid high-fat foods, especially those with saturated
fats like meat and cheese and those with refined sugars.
- "Eat" your water, that is, fruits and vegetables.
- Protein should not exceed 10-15% of diet (3 oz, size of
deck of cards). Use meat for flavor, not as the main
bulk of a meal.
- Sugars, added and natural, should not exceed 10% of diet.
- Salt: less than 2000 mg daily.
- One hour/day of moderate exercise, e.g. walking.
These practices and principles are borne out by experience and research.
Here is some perspective.
- The World Health Organization of the United Nations (WHO)
recommendations are very similar to Pritikin's.
- Compare it to, for example, the Atkins diet (high fat, high protein).
Atkins (and most others) are discredited by
research, but popular because it gets initial results
quickly and people like to be told to eat meat and cheese.
- The global epidemic of obesity, heart disease, and chronic
disease is due to:
- Western-style staples like red meat and dairy,
vegetable oils, sugar-rich drinks and sweets,
and salty snacks replacing traditional, closer-to-nature
staples like beans, potatoes, corn, and fresh vegetables
- Sedentary lifestyles
The Pritikin program has 30+ years of experience.
Their track record is unmatched -- this is the real deal.
Check it out... and get healthy!
top
|
| |
|
November, 2008 -- Are we getting the message about health and personal responsibility?
Here is a gem I found on the web...
people really do eat at the
Heart Attack Grill.
They even have cigarettes on the menu!
top
|
| |
 Cato Schmato
Cato Schmato
September, 2007 --
Want to set your teeth on edge?
Read
the
"scholarly" writings of the whack-jobs over at Cato.
These are no more than
industry-sponsored puff-pieces:
- Exxon-Mobil, Shell Oil, Tenneco Gas, Amoco Foundation,
Atlantic Richfield Foundation, Chevron Companies,
and the American Petroleum Institute
re: global warming "myth"
- Philip Morris, R.J. Reynolds re: "smokers' rights"
- Other sources of funding include Bell Atlantic Network Services, BellSouth Corporation,
Digital Equipment Corporation, GTE, Microsoft, NYNEX,
Sun Microsystems, Viacom International, American Express,
Chase Manhattan Bank, Chemical Bank, Citicorp/Citibank,
Commonwealth Fund, Prudential Securities and Salomon Brothers.
Writings on the medical system are sponsored by the
pharmaceutical industry (Eli Lilly, Merck, Pfizer).
The intent is to influence policy under the guise of researched wisdom.
Don't vote for any politician who can't see through this sham!
For example, an article on healthcare funding,
Socialized Medicine is Already Here,
reveals its bias in the title; "socialized medicine"
is derogatory and no one would choose anything with that name.
It's like Bush saying about Iraq, "We want victory, not defeat!"
Well, duh.
In high school, we learned to call such statements tautologies,
vacuous statements that set my teeth on edge.
Now let's get to work on the real issues.
top
|
| |
 Getting It Explained?
Getting It Explained?
July, 2006 -- Do you know what your insurance covers? Do you understand the invoices
you get from your hospital or your provider? Do you understand the
EOB
(Explanation of Benefits)
your insurance company provides when you make a claim?
Have you actually read your policy?
If you have, did you understand what you read?
Did it give you confidence that your medical needs would be met?
When you go for medical care, do you know
what you'll be charged out of your own pocket? Or do you cross your fingers
and hope for the best? Can your doctor (or your doctor's receptionist)
provide clarity on any of this? Do you even bother to ask?
Have you ever tried not to pay an insane medical bill? Have you seen what that
does to your credit rating?... And then tried to buy a car or a house or
get a credit card? Why is any of this OK?
top
|
| |
 Vaccinate!
Vaccinate!
January, 2009 -- Ever seen a list of all the vaccinations in one place?
Useful! Here they are... Among medicine's greatest achievements.
- Diphtheria
- Tetanus
- Pertussis
- Poliomyelitis
- Haemophilus influenzae type b - Hib
- Measles
- Mumps
- Rubella
- Varicella
- Hepatitis A
- Hepatitis B
- Influenza
- Pneumococcal Disease
- Meningococcal Disease
- Human Papillomavirus
- Rotavirus

The details about these and lots more
excellent information for practitioners about vaccinations
(is it possible they aren't taught this stuff in med school?!?)
can be
found at docsimmunize.org.
This valuable web site is run by Terri Olson, RN
(wife of Pat).
top
|
| |
 Pat Rants
Pat Rants
May, 2005 --
My lifelong pal Pat Olson
has had a distinguished career as a US Navy flight surgeon.
He learned much about "...a practice of socialistic medicine called the US Navy."
He goes on:
Does it promote itself as socialistic? Obviously not.
Is it a perfect system? Obviously not.
But even its critics admit that with access to care
for servicemembers and their families regardless of rank or ability to pay,
in terms of objectively verifiable outcome measures it betters the US
private sector.
This leads me to something I see as the Dark Side of medical informatics.
As long as we have a 'pro-competition' insurance industry,
rewards will go to those who cherry-pick. Beyond HIPAA,
you've got the specter of cyber sleuthing medical records for the familial
trait here, the genetic deletion there, that incurs increased risk. It
terrifies me to think of a child being denied care because of something
in a record somewhere and broadcast unknowingly to the wolves
of the insurance industry.
Okay, I'm outta control...
But we agree, Pat, we agree.
top
|
Updated Tuesday, 20-Aug-2024 16:51:14 MDT
|

